Overview
A goiter (GOI-tur) is the irregular growth of the thyroid gland. The thyroid is a butterfly-shaped gland located at the base of the neck just below the Adam's apple.
A goiter may be an overall enlargement of the thyroid, or it may be the result of irregular cell growth that forms one or more lumps (nodules) in the thyroid. A goiter may be associated with no change in thyroid function or with an increase or decrease in thyroid hormones.

Enlarged thyroid
Widespread enlargement of the thyroid can expand the gland well beyond its typical size (left) and cause a noticeable bulge in the neck (right).
The most common cause of goiters worldwide is a lack of iodine in the diet. In the United States, where the use of iodized salt is common, goiters are caused by conditions that change thyroid function or factors that affect thyroid growth.
Treatment depends on the cause of the goiter, symptoms, and complications resulting from the goiter. Small goiters that aren't noticeable and don't cause problems usually don't need treatment.
Symptoms
Most people with goiters have no signs or symptoms other than a swelling at the base of the neck. In many cases, the goiter is small enough that it's only discovered during a routine medical exam or an imaging test for another condition.
Other signs or symptoms depend on whether thyroid function changes, how quickly the goiter grows and whether it obstructs breathing.
Underactive thyroid (hypothyroidism)
Signs and symptoms of hypothyroidism include:
- Fatigue.
- Increased sensitivity to cold.
- Increased sleepiness.
- Dry skin.
- Constipation.
- Muscle weakness.
- Problems with memory or concentration.
Overactive thyroid (hyperthyroidism)
Signs and symptoms of hyperthyroidism include:
- Weight loss.
- Rapid heartbeat (tachycardia).
- Increased sensitivity to heat.
- Excess sweating.
- Tremors.
- Irritability and nervousness.
- Muscle weakness.
- Frequent bowel movements.
- Changes in menstrual patterns.
- Sleep difficulty.
- High blood pressure.
- Increased appetite.
Children with hyperthyroidism might also have the following:
- Rapid growth in height.
- Changes in behavior.
- Bone growth that outpaces expected growth for the child's age.
Obstructive goiter
The size or position of a goiter may obstruct the airway and voice box. Signs and symptoms may include:
- Difficulty swallowing.
- Difficulty breathing with exertion.
- Cough.
- Hoarseness.
- Snoring.
From Mayo Clinic to your inbox
Causes
How the thyroid gland works
Two hormones produced by the thyroid are thyroxine (T-4) and triiodothyronine (T-3). When the thyroid releases T-4 and T-3 into the bloodstream, they play a role in many functions in the body, including the regulation of:
- The conversion of food into energy (metabolism).
- Body temperature.
- Heart rate.
- Blood pressure.
- Other hormone interactions.
- Growth during childhood.
The thyroid gland also produces calcitonin, a hormone that helps regulate the amount of calcium in the blood.
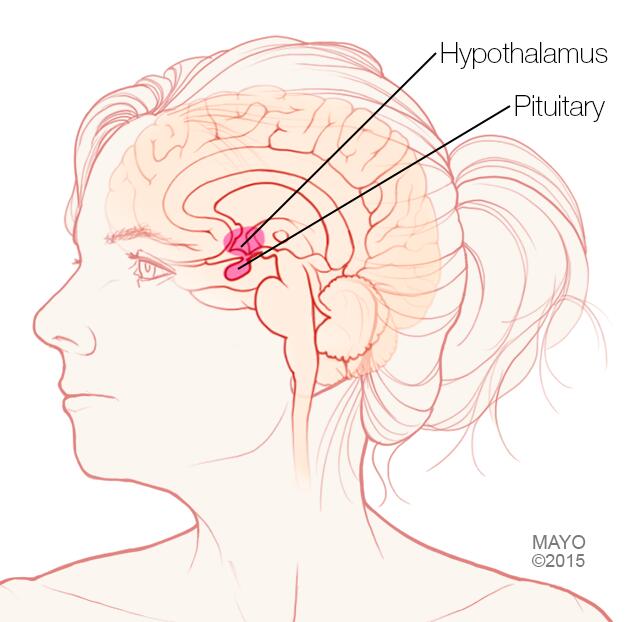
Pituitary gland and hypothalamus
The pituitary gland and the hypothalamus are located within the brain and control hormone production.
How the thyroid is regulated
The pituitary gland and hypothalamus control the rate at which T-4 and T-3 are produced and released.
The hypothalamus is a specialized region at the base of the brain. It acts as a thermostat for maintaining balance in multiple body systems. The hypothalamus signals the pituitary gland to make a hormone known as thyroid-stimulating hormone (TSH).
The pituitary gland — located below the hypothalamus — releases a certain amount of TSH, depending on how much T-4 and T-3 are in the blood. The thyroid gland, in turn, regulates its production of hormones based on the amount of TSH it receives from the pituitary gland.
Causes of goiter
A number of factors that influence thyroid function or growth can result in a goiter.
- Iodine deficiency. Iodine is essential for the production of thyroid hormones. If a person does not get enough dietary iodine, hormone production drops and the pituitary gland signals the thyroid to make more. This increased signal results in thyroid growth. In the United States, this cause is uncommon because of iodine added to table salt.
- Hashimoto's disease. Hashimoto's disease is an autoimmune disorder, an illness caused by the immune system attacking healthy tissues. The damaged and inflamed tissues of the thyroid don't produce enough hormones (hypothyroidism). When the pituitary gland detects the decline and prompts the thyroid to create more hormones, the thyroid can become enlarged.
- Graves' disease. Another autoimmune disorder called Graves' disease occurs when the immune system produces a protein that mimics TSH. This rogue protein prompts the thyroid to overproduce hormones (hyperthyroidism) and can result in thyroid growth.
- Thyroid nodules. A nodule is the irregular growth of thyroid cells that form a lump. A person may have one nodule or several nodules (multinodular goiter). The cause of nodules is not clear, but there may be multiple factors — genetics, diet, lifestyle and environment. Most thyroid nodules are noncancerous (benign).
- Thyroid cancer. Thyroid cancer is less common than other cancers and generally treatable. About 5% of people with thyroid nodules are found to have cancer.
- Pregnancy. A hormone produced during pregnancy, human chorionic gonadotropin (HCG), may cause the thyroid gland to be overactive and enlarge slightly.
- Inflammation. Thyroiditis is inflammation of the thyroid caused by an autoimmune disorder, bacterial or viral infection, or medication. The inflammation may cause hyperthyroidism or hypothyroidism.

Thyroid nodules
Enlargement of your thyroid can expand the gland well beyond its typical size and cause a noticeable bulge in your neck. This can be caused by single or multiple nodules, also called lumps, in your thyroid, or by an autoimmune process.
Risk factors
Anyone can develop a goiter. It may be present at birth or occur at any time throughout life. Some common risk factors for goiters include:
- A lack of dietary iodine. Iodine is found primarily in seawater and in the soil in coastal areas. In the developing world in particular, people who don't have enough iodine in their diets or access to food supplemented with iodine are at increased risk. This is rare in the United States.
- Being female. Women are more likely to develop a goiter or other thyroid disorders.
- Pregnancy and menopause. Thyroid problems in women are more likely to occur during pregnancy and menopause.
- Age. Goiters are more common after age 40.
- Family medical history. Family medical history of goiters or other thyroid disorders increases the risk of goiters. Also, researchers have identified genetic factors that may be associated with an increased risk.
- Medications. Some medical treatments, including the heart drug amiodarone (Pacerone) and the psychiatric drug lithium (Lithobid), increase your risk.
- Radiation exposure. Your risk increases if you've had radiation treatments to your neck or chest area.
Complications
A goiter itself usually doesn't cause complications. The appearance may be troublesome or embarrassing for some people. A large goiter may obstruct the airway and voice box.
Changes in the production of thyroid hormones that may be associated with goiters have the potential for causing complications in multiple body systems.