There are several types of psoriasis. Each has its own signs and symptoms and can look different from person to person. It also is possible to have more than one type at the same time.
Psoriasis happens when skin cells grow too quickly, causing a buildup of dry, scaly patches on the skin. These patches can be small or they can cover large areas of the body. Psoriasis is not contagious — you can't spread it to others or get it from someone else.
Psoriasis is a long-term condition that doesn't have a cure. But treatments can help you manage your symptoms. The exact cause of psoriasis isn't known, though it's thought to be an immune system condition.
Find out about the symptoms, treatments and self-care tips for the main types of psoriasis:
- Plaque psoriasis
- Nail psoriasis
- Guttate psoriasis
- Inverse psoriasis
- Pustular psoriasis
- Erythrodermic psoriasis
Plaque psoriasis
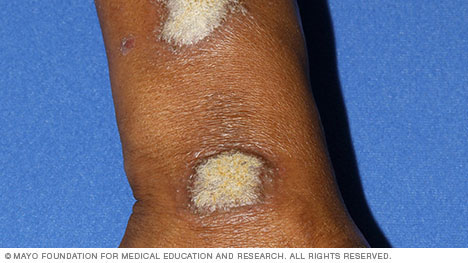
Plaque psoriasis
Plaque psoriasis is the most common form of psoriasis. It causes dry, raised patches of skin called plaques. These patches are covered with silver scales and can look red, purple, gray or brown, depending on your skin color. You may have only a few plaques or many.
Try these self-care tips to help manage plaque psoriasis:
- Bathe or shower daily with mild soap and lukewarm water to soothe your skin.
- Use steroid creams you can buy without a prescription and a thick, ointment-type moisturizer to keep your skin soft and reduce irritation.
- Learn what triggers your psoriasis to flare and try to avoid those things. Common triggers include infections, stress and sunburns.
People with moderate or severe plaque psoriasis may need stronger treatment, such as light therapy, prescription creams, coal tar products, and prescription medicines taken by mouth or given as a shot.
Nail psoriasis
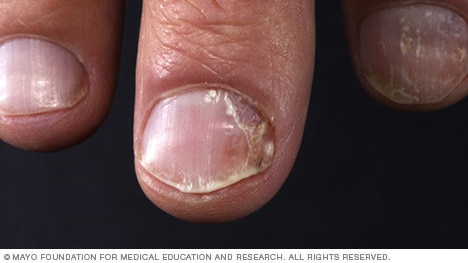
Nail psoriasis
Psoriasis can affect fingernails and toenails. It may cause small dents, changes in how the nails grow, or discoloration. Sometimes the nails can loosen and pull away from the skin underneath. When the condition is more serious, the nails may thicken or crumble. Nail psoriasis often happens along with other types of psoriasis, such as plaque psoriasis.
These self-care tips can help you manage your symptoms:
- Keep nails clean and trimmed.
- Avoid biting or picking at nails and cuticles.
- Moisturize nails and cuticles often.
- Wear gloves when doing housework and yard work.
For mild nail psoriasis, prescription steroid creams and creams with vitamin D can help improve nail appearance over time. For moderate to severe symptoms, prescription medicines that calm the immune system are often the most effective treatment.
Guttate psoriasis
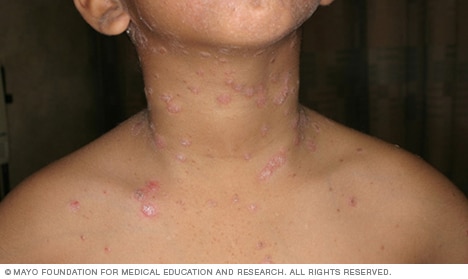
Guttate psoriasis
Guttate psoriasis is most common in children and young adults. It often starts after an infection, such as strep throat. This type of psoriasis causes small, drop-shaped spots on the trunk, arms or legs. The spots are covered with flaky, silver scales and may look red, purple, gray or brown, depending on your skin color. They also can be itchy.
Treatment often includes light therapy, prescription steroid cream, or other creams that contain vitamin D. If you have more serious symptoms, you may need prescription medicines taken by mouth or given as a shot. If you have an infection, your healthcare professional may prescribe an antibiotic medicine to treat it.
Inverse psoriasis
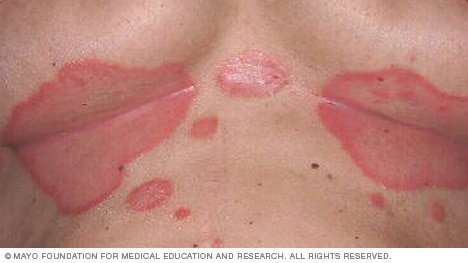
Inverse psoriasis
Inverse psoriasis causes smooth, shiny patches of skin in areas where skin touches or rubs together, such as under the breasts, in the groin or in the armpits. The patches may look red, brown or purple, depending on your skin color. The skin may feel sore or itchy. Common triggers are infection, certain medicines, and skin cuts or scrapes.
Heat and moisture can worsen symptoms. Try these self-care tips for managing inverse psoriasis:
- Wear loose-fitting, lightweight clothing that allows air flow.
- Keep the affected skin as dry as possible. Pat with soft tissues or use a blow dryer on cool and low settings.
- Try to avoid getting hot and sweaty.
For mild inverse psoriasis, treatment often starts with steroid creams you can buy without a prescription. Your healthcare professional also may prescribe creams that contain vitamin D or medicines called calcineurin inhibitors that calm the immune system. If you have more serious symptoms, you may need light therapy, prescription steroid creams, or prescription medicines taken by mouth or given as a shot.
Pustular psoriasis

Pustular psoriasis
Pustular psoriasis is a rare type of psoriasis that causes areas of pus-filled bumps or blisters on the skin. It can appear in smaller patches on the hands or feet or cover large parts of the body. The affected skin may appear pink, gray, purple or dark brown, depending on your skin color.
The skin may become swollen, sore and discolored shortly before blisters form, often within hours. The blisters usually heal within a few days but can come back. Triggers include infections, certain medicines and stopping some medicines too fast.
Small patches often are treated with steroid creams or ointments you can buy without a prescription. Larger areas may need treatment with prescription medicines taken by mouth or given as a shot. Light therapy may help after the blisters heal and the skin is less sensitive. Treating or avoiding triggers also can help the skin heal.
Erythrodermic psoriasis
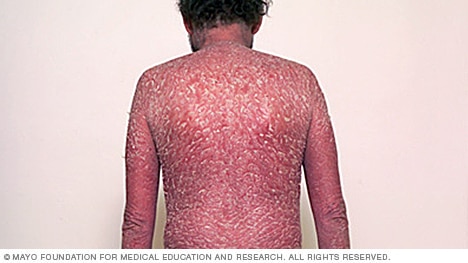
Erythrodermic psoriasis
Erythrodermic psoriasis is the rarest and most severe form of psoriasis. It causes a scaly rash that can cover most of body. The skin may feel very itchy and have a strong burning sensation. Triggers can include certain medicines, stopping some medicines too quickly, severe sunburn and infection.
Treatment may include:
- Medicine applied to the affected skin and covered with wet bandages.
- Steroid medicine taken by mouth.
- Prescription medicines taken by mouth or given as a shot.
Some people with erythrodermic psoriasis may need hospital care.