Overview
Contact dermatitis
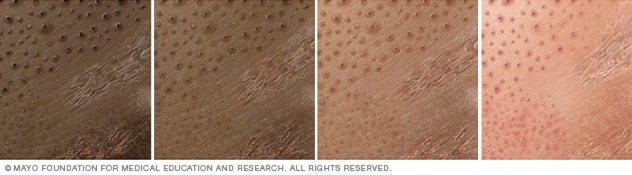
Contact dermatitis
Illustration of contact dermatitis on different skin colors. Contact dermatitis can appear as an itchy rash.
Contact dermatitis is an itchy rash caused by direct contact with a substance or an allergic reaction to it. The rash isn't contagious, but it can be very uncomfortable.
Many substances can cause this reaction, such as cosmetics, fragrances, jewelry and plants. The rash often shows up within days of exposure.
To treat contact dermatitis successfully, you need to identify and avoid the cause of your reaction. If you avoid the substance causing the reaction, the rash often clears up in 2 to 4 weeks. You can try soothing your skin with a cool, wet cloth and other self-care steps.
Products & Services
Symptoms
Contact dermatitis on the face
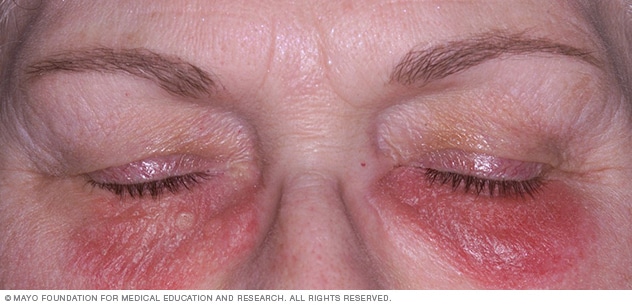
Contact dermatitis on the face
Contact dermatitis often affects skin directly exposed to an offending substance. Here, the rash is likely caused by cosmetics.
Poison ivy blisters
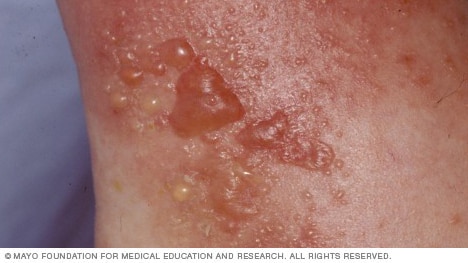
Poison ivy blisters
Here, the blisters are caused by contact with the oily substance in poison ivy (urushiol) that causes allergic reactions.
Contact dermatitis shows up on skin that has been directly exposed to the substance causing the reaction. For example, the rash may show up along a leg that brushed against poison ivy. The rash can develop within minutes to hours of exposure, and it can last 2 to 4 weeks.
Signs and symptoms of contact dermatitis vary widely and may include:
- An itchy rash
- Leathery patches that are darker than usual (hyperpigmented), typically on brown or Black skin
- Dry, cracked, scaly skin, typically on white skin
- Bumps and blisters, sometimes with oozing and crusting
- Swelling, burning or tenderness
When to see a doctor
See your health care provider if:
- The rash is so itchy that you can't sleep or go about your day
- The rash is severe or widespread
- You're worried about how your rash looks
- The rash doesn't get better within three weeks
- The rash involves the eyes, mouth, face or genitals
Seek immediate medical care in the following situations:
- You think your skin is infected. Clues include fever and pus oozing from blisters.
- It's hard to breathe after inhaling burning weeds.
- Your eyes or nasal passages hurt after inhaling smoke from burning poison ivy.
- You think an ingested substance has damaged the lining of your mouth or digestive tract.
Causes
Contact dermatitis is caused by exposure to a substance that irritates your skin or triggers an allergic reaction. The substance could be one of thousands of known allergens and irritants. Often people have irritant and allergic reactions at the same time.
Irritant contact dermatitis is the most common type. This nonallergic skin reaction occurs when an irritant damages your skin's outer protective layer.
Some people react to strong irritants after a single exposure. Others may develop a rash after repeated exposures to even mild irritants, such as soap and water. And some people develop a tolerance to the substance over time.
Common irritants include:
- Solvents
- Rubber gloves
- Bleach and detergents
- Hair products
- Soap
- Airborne substances
- Plants
- Fertilizers and pesticides
Allergic contact dermatitis occurs when a substance to which you're sensitive (allergen) triggers an immune reaction in your skin. It often affects only the area that came into contact with the allergen. But it may be triggered by something that enters your body through foods, flavorings, medicine, or medical or dental procedures (systemic contact dermatitis).
People often become sensitized to allergens after many contacts with it over years. Once you develop an allergy to a substance, even a small amount of it can cause a reaction.
Common allergens include:
- Nickel, which is used in jewelry, buckles and many other items
- Medications, such as antibiotic creams
- Balsam of Peru, which is used in many products, such as perfumes, toothpastes, mouth rinses and flavorings
- Formaldehyde, which is in preservatives, cosmetics and other products
- Personal care products, such as body washes, hair dyes and cosmetics
- Plants such as poison ivy and mango, which contain a highly allergenic substance called urushiol
- Airborne allergens, such as ragweed pollen and spray insecticides
- Products that cause a reaction when you're in the sun (photoallergic contact dermatitis), such as some sunscreens and cosmetics
Children develop allergic contact dermatitis from the usual offenders and also from exposure to diapers, baby wipes, jewelry used in ear piercing, clothing with snaps or dyes, and so on.
Risk factors
The risk of contact dermatitis may be higher in people who have certain jobs and hobbies. Examples include:
- Agricultural workers
- Cleaners
- Construction workers
- Cooks and others who work with food
- Florists
- Hair stylists and cosmetologists
- Health care workers, including dental workers
- Machinists
- Mechanics
- Scuba divers or swimmers, due to the rubber in face masks or goggles
Complications
Contact dermatitis can lead to an infection if you repeatedly scratch the affected area, causing it to become wet and oozing. This creates a good place for bacteria or fungi to grow and may cause an infection.
Prevention
You can take the following steps to help prevent contact dermatitis:
- Avoid irritants and allergens. Try to identify and avoid the cause of your rash. For ear and body piercings, use jewelry made of hypoallergenic material, such as surgical steel or gold.
- Wash your skin. For poison ivy, poison oak or poison sumac, you might be able to remove most of the rash-causing substance if you wash your skin right away after coming into contact with it. Use a mild, fragrance-free soap and warm water. Rinse completely. Also wash any clothing or other items that may have come into contact with a plant allergen, such as poison ivy.
- Wear protective clothing or gloves. Face masks, goggles, gloves and other protective items can shield you from irritating substances, including household cleansers.
- Apply an iron-on patch to cover metal fasteners next to your skin. This can help you avoid a reaction to jean snaps, for example.
- Apply a barrier cream or gel. These products can provide a protective layer for your skin. For example, a nonprescription skin cream containing bentoquatam (Ivy Block) may prevent or lessen your skin's reaction to poison ivy.
- Use moisturizer. Regularly applying moisturizing lotions can help restore your skin's outermost layer and keep your skin supple.
- Take care around pets. Allergens from plants, such as poison ivy, can cling to pets and then be spread to people. Bathe your pet if you think it got into poison ivy or something similar.
Video: Allergy or irritant: The truth about your rash
Vivien Williams: Hand-washing is essential for preventing the spread of germs. But, sometimes, all this scrubbing can cause a rash. Does this mean you're allergic to the soap?
Dawn Davis, M.D., Dermatology, Mayo Clinic: One important thing to differentiate from allergic contact dermatitis is irritant contact dermatitis.
Vivien Williams: Dr. Dawn Davis says allergic contact dermatitis means a substance is causing an allergic reaction on your skin. But irritant contact dermatitis means your skin is inflamed from repeated exposure to something.
Dr. Davis: If I used lye soap on my skin, and I used it over and over again, I would develop an irritant contact dermatitis simply from eroding away the natural barrier of my skin with repetitive washing.
Vivien Williams: Dr. Davis says it's not always easy to tell the difference between an allergy or irritant.
Dr. Davis: So it's very helpful to go to a health provider, especially a dermatologist, to help differentiate between irritant contact dermatitis
Vivien Williams: and an allergy. That way you can properly treat the rash and prevent it from happening again.
For the Mayo Clinic News Network, I'm Vivien Williams.