Overview
Buerger disease
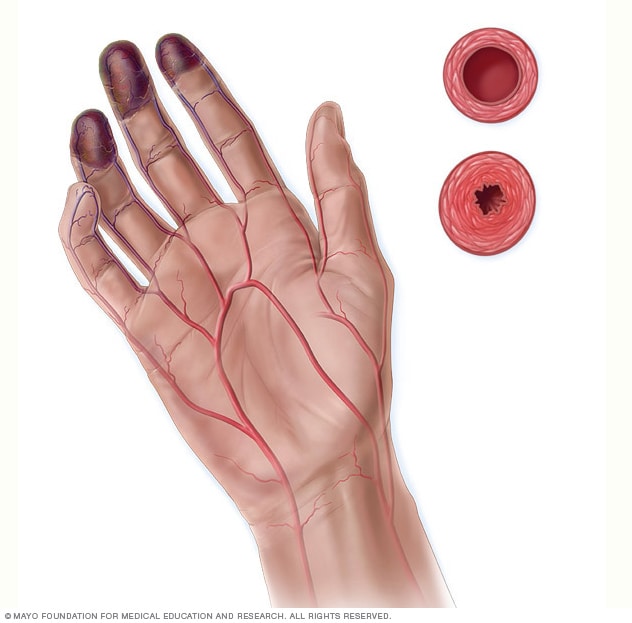
Buerger disease
In Buerger disease, the small blood vessels of the feet and hands become blocked with blood clots. Over time, skin tissue is damaged or destroyed. Open, painful sores develop on the toes and fingers. Not using tobacco is the best way to stop the disease from getting worse.
Buerger disease is a rare disease of the arteries and veins in the arms and legs. In Buerger disease — also called thromboangiitis obliterans — blood vessels become blocked. This reduces blood flow to the affected areas. Blood clots may form in the blood vessels.
Over time, the lack of blood flow damages or destroys skin tissue. The damage can lead to infection and death of body tissue, called gangrene. Buerger disease is usually first seen in the feet. It may eventually affect the blood vessels of the hand. Blood clots may form in the small veins of the arms and legs.
People who get Buerger disease almost always smoke cigarettes or use other forms of tobacco, such as chewing tobacco. Quitting all forms of tobacco is the only way to stop Buerger disease. For those who don't quit, surgery to remove fingers and toes might be needed.
Products & Services
Symptoms
Buerger disease symptoms include:
- Tingling or numbness in the fingers or toes.
- Changes in skin color in the hands and feet. The skin may look pale gray, red or blue. Depending on your skin color, these color changes may be harder or easier to see.
- Fingers and toes that turn white then blue when exposed to cold, known as Raynaud's disease. Depending on your skin color, these color changes may be harder or easier to see.
- Pain in the feet that occurs with walking. The pain may make it difficult to walk long distances.
- Painful open sores on fingers and toes. Pain in the fingers and toes may become severe and occur at rest.
- Inflammation of a vein just below the skin's surface, due to a blood clot in the vein.
When to see a doctor
See a health care provider if you think you have symptoms of Buerger disease.
Causes
The exact cause of Buerger disease is unknown. The condition is strongly linked to tobacco use. It's thought that chemicals in tobacco may hurt the lining of the blood vessels.
Experts think that some people have genes that make them more likely to get Buerger disease. It's also possible that the disease occurs when the body's immune system attacks healthy tissue by mistake.
Risk factors
The biggest risk factor for Buerger disease is smoking or using any type of tobacco. The disease can occur in people who smoke cigarettes, use cigars and chew tobacco. The rates of Buerger disease are highest in areas of the Mediterranean, Middle East and Asia where heavy smoking is most common.
Some research says that long-term use of marijuana, also called cannabis, also raises the risk of blood vessel problems similar to those of Buerger disease.
Other risk factors for Buerger disease include being male and being younger than 45 years old. Long-term infection of the gums in the mouth may also increase the risk. But more study is needed to confirm this link.
Complications
Buerger disease decreases blood flow to the hands and feet. As the disease gets worse, the skin and tissue in the affected areas do not get enough blood. This can cause painful open sores that do not heal. The sores may lead to a complication called gangrene.
Symptoms of gangrene include black or blue skin, a loss of feeling in the affected finger or toe, and a bad smell from the area. Gangrene is a serious condition. Surgery is usually needed to remove the affected finger, toe or other tissue.
Prevention
Nearly everyone who has Buerger disease has smoked or used some form of tobacco. To prevent Buerger disease, it's important to not use tobacco.
Quitting smoking can be hard. Talk to a health care provider about ways to quit.
Dec. 19, 2024