Overview
A myomectomy is a surgery to take out fibroids from the uterus. Fibroids are common lumps that grow in the uterus, which is the part of the body where babies develop. These lumps are also called leiomyomas. Fibroids usually grow during the years when a person can have children, but they can happen up at any age.
Uterine fibroids are not cancer, but they can still cause problems. These problems include very heavy periods and pain in the lower belly. The purpose of a myomectomy is to remove fibroids that cause these issues.
After taking out the fibroids, the uterus is repaired and left in place. Unlike a hysterectomy, which takes out the whole uterus, a myomectomy removes only the fibroids.
Why it's done
The goal of a myomectomy is to take out fibroids that cause problems or get in the way of your day-to-day activities. This surgery removes the fibroids but keeps the uterus.
There are other ways to treat fibroids, including having a hysterectomy. A hysterectomy is a surgery to take out the uterus. You might choose a myomectomy instead of a hysterectomy if:
- You want to have a baby in the future.
- Fibroids are stopping you from getting pregnant.
- You want to keep your uterus.
Risks
Myomectomy has a low rate of complications. Still, the procedure poses some risks. Risks of myomectomy include:
-
Blood loss. Heavy bleeding from uterine fibroids can cause anemia. Anemia happens when you don't have enough healthy red blood cells. These cells carry oxygen throughout the body. People with anemia may have a higher risk of problems after surgery because of blood loss. To help, your care team may suggest ways to build up your red blood cell count before surgery.
During the procedure, your surgeon may take extra steps to avoid too much bleeding. This might include using a tourniquet to stop blood flow from the uterine arteries. Medicines injected around fibroids also can narrow blood vessels for a short time, reducing blood flow. But even with these steps, sometimes a blood transfusion is needed.
- Scar tissue. When the uterus is cut during surgery, bands of scar tissue called adhesions can form. This scar tissue can sometimes cause problems with future pregnancies or other surgeries. Some types of fibroid surgery may cause less scar tissue than others.
- Pregnancy or childbirth complications. Getting pregnant after having a myomectomy may put you at risk for problems during labor and delivery. In rare cases, the uterus could tear during labor. This is called a uterine rupture. Fibroids themselves can also make pregnancy more difficult. Because of these risks, you may need a C-section if you've had a myomectomy.
- Small chance of needing a hysterectomy. In rare cases, the surgeon may need to remove the whole uterus during the surgery. This could happen if there's too much bleeding or if something other than fibroids is found.
- Small chance of spreading cancer. Rarely, a lump thought to be a fibroid may actually be cancer. If it's removed using a method called morcellation — where the tissue is cut into small pieces to take it out — the cancer could spread. This risk is higher in older women and after menopause. Be sure to talk with your surgeon about the risks and benefits of morcellation before surgery.
Ways to lower the risk of problems during myomectomy
To help make myomectomy safer, your care team may suggest certain things you can do before the procedure:
- Iron and vitamins. If you have anemia from heavy periods, your healthcare professional might have you take iron supplements and vitamins. These can help you build up your red blood cell count before surgery.
- Hormone treatment. Another way to treat anemia before surgery is with hormones. Hormone treatments can stop or reduce bleeding during your period. Some types include birth control pills or medicines known as gonadotropin-releasing hormone agonists, also called GnRH agonists. These keep your body from making certain hormones, which can stop your period and help increase your blood's iron levels.
- Shrink fibroids before surgery. Some hormone treatments, such as GnRH agonists, can also make fibroids and the uterus smaller. This might help your surgeon do the surgery with smaller cuts, which often means a quicker recovery. In some cases, shrinking the fibroids may even mean you don't need surgery at all.
GnRH agonists can cause side effects that feel like menopause. These may include hot flashes, night sweats and vaginal dryness. These symptoms usually go away after you stop taking the medicine. To help with side effects, your healthcare professional also may have you take estrogen and progestin, hormones that treat menopause symptoms. You may need to take these medicines for a few months before your surgery.
GnRH agonist therapy isn't right for everyone. Sometimes it can shrink fibroids so much that they are hard to find during surgery. The medicine can also be expensive and may cause unwanted side effects. Your healthcare professional will help you decide if this treatment is a good choice for you.
How you prepare
Before having a myomectomy, you'll likely meet with your surgeon to talk about your fibroids and the different ways the surgery can be done. Your surgeon and care team will help you choose the best option for you. It's a good idea to bring a list of questions, so that you can understand everything about the surgery and its risks.
To get ready for your myomectomy:
- Tell your care team about all the medicines, vitamins or supplements you take. Some of them could affect the surgery.
- Follow the instructions your care team gives you. For example, you may need to stop taking some medicines days or even a week before the surgery to help reduce bleeding. You may also need to stop eating or drinking for several hours before the procedure.
- Bring someone with you. You'll need someone to drive you home after surgery. That person should also listen to your care instructions, since you may still be sleepy from the medicine they give you during surgery.
Other things to know
Ask your care team what kind of anesthesia will be used during the surgery. Depending on the type of myomectomy surgery that's planned, you may have:
- General anesthesia. This puts you completely to sleep, and a tube is placed in your throat to help you breathe. General anesthesia is used for laparoscopic, robotic or abdominal myomectomies. Sometimes it's also used for hysteroscopic myomectomies.
- Monitored anesthesia care. This makes you feel like you're asleep, and you likely won't remember the surgery. It doesn't require a breathing tube. It's often used for hysteroscopic myomectomies because these are less invasive and need less anesthesia.
Other types of anesthesia also may be used. Talk to your care team about how pain will be managed after surgery and how you'll take pain medicine.
You may need to prepare for a hospital stay. How long you stay in the hospital depends on the type of surgery you have. Many people can go home the same day. Others may need to stay in the hospital for 1 to 3 days.
What you can expect
Fibroid locations
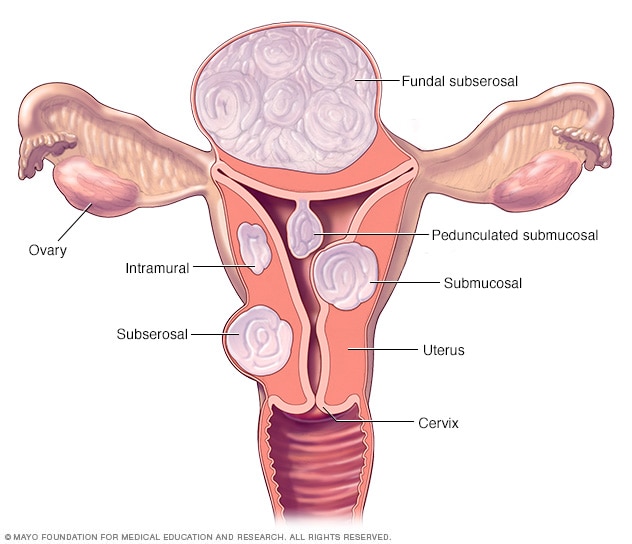
Fibroid locations
There are three main types of uterine fibroids. Intramural fibroids grow within the wall of the uterus. Submucosal fibroids grow into the space inside the uterus. Subserosal fibroids grow on the outside of the uterus. Some submucosal or subserosal fibroids hang from a stalk inside or outside of the uterus. This is called a pedunculated fibroid.
The way your surgeon will remove the fibroids depends on how big they are, how many there are and where they are in the uterus.
Abdominal myomectomy
In this type of myomectomy, the surgeon makes a cut in the lower part of your belly to reach the uterus and take out the fibroids. This kind of surgery is sometimes called a laparotomy.
Most of the time, the surgeon will make a low, side-to-side cut near the bikini line. But if the uterus is very big, the surgeon may need to make a straight up-and-down cut instead.
Because this surgery needs a bigger cut than other types of myomectomy, it usually takes longer to heal.
Laparoscopic myomectomy
In this type of myomectomy, the surgeon removes the fibroids through one or more small cuts in your belly using tiny cameras and surgical tools. This is called laparoscopy.
Compared to open surgery, which uses a larger cut, laparoscopy usually causes less bleeding, has fewer complications and leaves less scar tissue. You also are likely to spend less time in the hospital and recover faster.
Sometimes the fibroid is cut into smaller pieces so it can be taken out through one of the small cuts. Other times, the surgeon may need to make a bigger cut to take the fibroid out in one piece. In rare cases, the fibroid is removed through a small cut in the vagina.
Robotic myomectomy
In this type of myomectomy, the surgeon uses a special robot to help with the surgery. Small cuts are made in your belly, and tiny tools are put in through those cuts. The surgeon sits at a nearby console and uses robotic arms to move the tools. There's a surgical team in place at the bedside to help during the surgery.
Robotic myomectomy is a lot like laparoscopic surgery. Both usually cause less bleeding, help you heal faster, and have fewer complications compared to open surgery.
Robotic myomectomy can take more time and cost more than laparoscopic myomectomy, but the results are usually about the same. There haven't been many studies comparing the two types of myomectomy.
Hysteroscopic myomectomy
In a hysteroscopic myomectomy, a surgeon uses a thin, lighted tool and gently puts it through the vagina and cervix to reach the inside of the uterus. A clear liquid is put into the uterus to make it bigger so the surgeon can see better.
The surgeon removes the fibroid by cutting it into smaller pieces. To do this, the surgeon might use a wire loop that uses electricity or a tool with a small blade to shave pieces from the fibroid.
This type of surgery is usually done for smaller fibroids that stick out into the uterus, called submucosal fibroids. If the fibroid is too big, the surgeon might not be able to remove it all at once, and you may need a second surgery.
After the surgery
After the surgery, you'll go to a recovery area where your healthcare team will keep a close watch over you as you wake up.
You can expect some light vaginal bleeding, such as spotting or staining. This can last a few days or up to six weeks, depending on the type of surgery you had.
Most people feel some pain or discomfort after surgery. Your healthcare team may suggest over-the-counter pain medicine, such as acetaminophen (Tylenol, others) or ibuprofen (Advil, Motrin IB, others). Be sure to follow your healthcare team's instructions.
Before you go home, your healthcare team will explain how to take care of yourself. They may talk to both you and the person helping you get home. You'll get information about:
- How to care for the area where you had surgery.
- What pain medicine you can use.
- When to start taking your regular medicines again.
- Limits on activity as you heal, including work, sex and sports.
- Signs to watch for that tell you something's wrong.
- How to get in touch with your healthcare team.
- When your next medical appointments are.
Results
After a myomectomy, you may have:
- Relief from symptoms. After surgery, many people often feel better. Periods may be lighter, and pressure or pain in the belly usually improves.
- Better chances of getting pregnant. A myomectomy can help some people who are trying to have a baby. Doctors usually recommend waiting 3 to 6 months after the surgery before trying to get pregnant. This gives the uterus time to heal.
Sometimes, fibroids that weren't seen during surgery can still cause problems. Fibroids that weren't completely removed may grow again. New fibroids can also show up later. These may or may not need treatment.
If you only had one fibroid, you're less likely to get more fibroids compared to someone who had many fibroids. Getting pregnant after surgery may also lower the risk of new fibroids forming.
If new fibroids form or you have fibroids that grow back, you may have treatment options besides myomectomy. Other treatment options include:
- Uterine artery embolization. Tiny particles are put into the blood vessels feeding the fibroids. This cuts off their blood supply, making them shrink and easing symptoms.
- Radiofrequency ablation. Heat or friction is used to destroy the fibroids. This process is called ablation. A special ultrasound helps guide the treatment.
- MRI-guided focused ultrasound. This treatment also uses heat to destroy fibroids. It's guided with magnetic resonance imaging.
- Hysterectomy. Surgery to remove the uterus also may be an option if you're sure that you don't want to get pregnant in the future.
Aug. 09, 2025