Overview
Knee comparisons
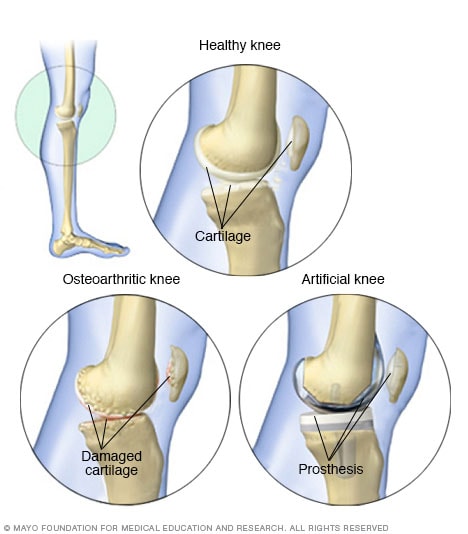
Knee comparisons
One of the most common reasons for knee replacement surgery is serious pain from joint damage. Joint damage is often caused by wear-and-tear arthritis, also called osteoarthritis. An artificial knee joint has metal caps to resurface the thighbone and shinbone, and high-density plastic to replace damaged cartilage. Each of these artificial parts is called a prosthesis.
Knee replacement surgery replaces parts of injured or worn-out knee joints. This also is known as knee arthroplasty. During the surgery, damaged bone and cartilage are replaced with parts made of metal and plastic.
Knee replacement surgery can help ease pain and make the knee work better. To decide whether a knee replacement is right for you, a surgeon checks your knee's range of motion, stability and strength. X-rays help show the extent of damage.
The right artificial joints and surgical techniques needed depend on many factors including age, weight, activity level, knee size and shape, and overall health.
Products & Services
Why it's done
The most common reason for knee replacement surgery is to ease pain caused by arthritis. People who need knee replacement surgery often have problems walking, climbing stairs and getting up out of chairs.
If only one part of the knee is damaged, surgeons often can replace just that part. This is called a partial knee replacement. If the entire joint needs to be replaced, the ends of the thighbone and shinbone are reshaped, and the entire joint is resurfaced. This is called a total knee replacement. The thighbone and shinbone are hard tubes that contain a soft center. The ends of the artificial parts are inserted into the softer central part of the bones.
Ligaments are bands of tissue that help hold joints together. If the knee's ligaments aren't strong enough to hold the joint together by themselves, the surgeon may choose implants that can be connected so they can't come apart.
Risks
Knee replacement surgery, like any surgery, carries risks. They include:
- Blood clots. Surgeons often recommend blood-thinning medicines to prevent this risk. The most common location for blood clots is in the leg. But they can travel to the lungs and become deadly.
- Nerve damage. Nerves in the area where the implant is placed can be injured. Nerve damage can cause numbness, weakness and pain.
- Infection. Infection can occur at the incision site or in the deeper tissue. Surgery is sometimes needed to treat an infection.
The implants used for knee replacements are durable, but they may loosen or become worn over time. If this happens, another surgery may be needed to replace the loose or worn parts.
How you prepare
Food and medicines
Your healthcare team might advise you to stop taking certain medicines and dietary supplements before your surgery. You'll likely be instructed not to eat anything after midnight the day of your surgery.
Prepare for your recovery
For several weeks after the procedure, you might need to use crutches or a walker, so arrange for them before your surgery. Make sure you have a ride home from the hospital and help with everyday tasks, such as cooking, bathing and doing laundry.
To make your home safer and easier to navigate during recovery, consider doing the following:
- Create a living space on one floor since climbing stairs can be difficult.
- Install safety bars or a secure handrail in your shower or bath.
- Secure stairway handrails.
- Get a stable chair with a firm seat cushion and back, and a footstool to elevate your leg.
- Arrange for a toilet seat riser with arms if you have a low toilet.
- Get a stable bench or chair for your shower.
- Remove loose rugs and cords.
What you can expect
When you check in for your surgery, you'll be asked to remove your clothes and put on a hospital gown. You'll be given either a spinal block, which numbs the lower half of your body, or a general anesthetic, which puts you into a sleep-like state.
Your surgeon also might inject a numbing medicine around nerves or in and around the joint to help block pain after your surgery.
During the procedure
Knee replacement surgery usually takes 1 to 2 hours. To perform the procedure, the surgeon:
- Makes an incision over the knee.
- Removes diseased and damaged bone and cartilage, leaving healthy bone intact.
- Implants the replacement parts into the thighbone, shinbone and kneecap.
After the procedure
Knee replacement surgery
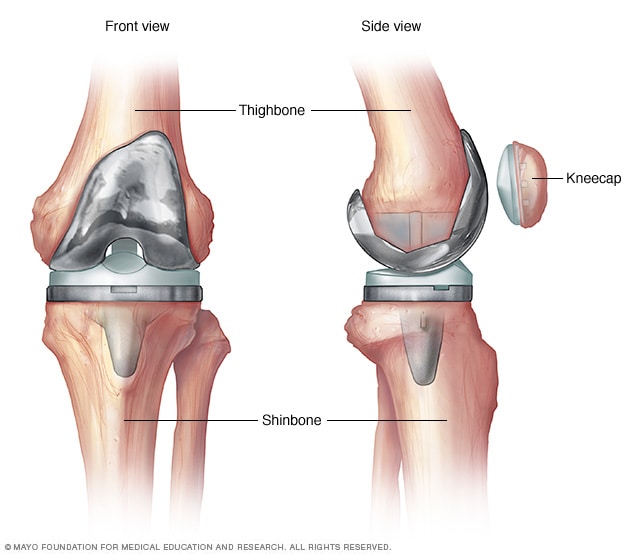
Knee replacement surgery
Artificial knee joints used in knee replacement surgery are typically made of metal and plastic. Metal parts replace the damaged thighbone and shinbone. Plastic replaces cartilage on the shin and kneecap parts.
After surgery, you'll rest in a recovery area for a short time. How long you stay in the hospital after surgery depends on your individual needs. Many people can go home the same day.
The risk of blood clots increases after knee replacement surgery. To prevent this complication, you may need to:
- Move early. You'll be encouraged to sit up and walk with crutches or a walker soon after surgery.
- Apply pressure. Both during and after surgery, you might wear elastic compression stockings or inflatable air sleeves on your lower legs. The air sleeves squeeze and release your legs. That helps keep blood from pooling in the leg veins, reducing the chance that clots will form.
- Take blood thinners. Your surgeon might prescribe an injected or oral blood thinner after surgery. Depending on how soon you walk, how active you are and your overall risk of blood clots, you might need blood thinners for several weeks after surgery.
You'll also likely be asked to do frequent breathing exercises and gradually increase your activity level. A physical therapist can show you how to exercise your new knee. After you leave the hospital, you'll likely continue physical therapy at home or at a center.
Results
For most people, knee replacement provides pain relief, improved mobility and a better quality of life. Most knee replacements can be expected to last at least 15 to 20 years.
After recovery, you can engage in various low-impact activities, such as walking, swimming, golfing or biking. But you should avoid higher impact activities, such as jogging, and sports that involve contact or jumping. Talk to your healthcare team about ways to stay active after knee replacement.
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.
Nov. 15, 2024