Overview
Hyperbaric oxygen therapy increases delivery of oxygen to the body by providing pure oxygen in an enclosed space with higher than normal air pressure.
Hyperbaric oxygen therapy treats a condition called decompression sickness that's caused by rapid drops in water pressure in scuba diving or air pressure in air or space travel. Other conditions treated with hyperbaric oxygen therapy include serious tissue disease or wounds, trapped air bubbles in blood vessels, carbon monoxide poisoning, and tissue damage from radiation therapy.
Products & Services
Why it's done
The goal of hyperbaric oxygen therapy is to get more oxygen to tissues damaged by disease, injury or other factors. In a hyperbaric oxygen therapy chamber, the air pressure is increased 2 to 3 times higher than normal air pressure. The lungs can gather much more oxygen than would be possible breathing pure oxygen at normal air pressure.
The effects on the body include:
- Removing trapped air bubbles.
- Enhancing the growth of new blood vessels and tissues.
- Supporting immune system activity.
Hyperbaric oxygen therapy is used to treat multiple conditions.
- Lifesaving treatment. Hyperbaric oxygen therapy can save the lives of people who have:
- Air bubbles in blood vessels.
- Decompression sickness.
- Carbon monoxide poisoning.
- Serious trauma, such as a crushing injury, causing blocked blood flow.
- Limb-saving treatment. The therapy can be an effective treatment for:
- Infections of tissues or bone that cause tissue death.
- Nonhealing wounds, such as a diabetic foot ulcer.
- Tissue-saving treatment. The therapy can help with the healing of:
- Skin grafts or skin flaps at risk of tissue death.
- Tissue and skin grafts after burn injuries.
- Tissue damage from radiation therapy.
- Other treatments. The therapy also may be used to treat:
- Puss-filled pockets in the brain called brain abscesses.
- Low counts of red blood cells from serious blood loss.
- Sudden hearing loss from an unknown cause.
- Sudden vision loss from blocked blood flow to the retina.
Risks
Hyperbaric oxygen therapy is generally a safe procedure. Most complications are mild and do not last. Serious complications are rare. The risk of complications increases with longer and repeated therapies.
Increased air pressure or the pure oxygen can result in the following:
- Ear pain.
- Middle ear injuries, including eardrum rupture and leaking fluid from the middle ear.
- Sinus pressure that can cause pain, runny nose or nose bleeds.
- Short-term changes in sight.
- Cataract formation with long courses of treatment.
- Short-term decline in lung function.
- Low blood sugar in people who have diabetes treated with insulin.
Uncommon, more-serious complications include:
- Lung collapse.
- Seizures from too much oxygen in the central nervous system.
Some people may experience anxiety while being in an enclosed space, also called claustrophobia.
Oxygen-rich environments increase the risk of fires. Certified programs that provide hyperbaric oxygen therapy must follow guidelines to prevent fires.
Preventing side effects
Steps to lessen certain side effects include the following.
- Your healthcare team will explain tips, such as yawning or swallowing, to help you relieve the pressure or feelings of fullness in your ears.
- If you have more-serious ear side effects and need repeat treatments, your healthcare team may recommend the placement of ear tubes.
- If you have hay fever or other nasal symptoms, you might take a decongestant, steroid or antihistamine to prevent sinus pain or runny nose.
- If you are anxious about being in an enclosed space, you may be given a drug to help you relax.
How you prepare
Your healthcare team will provide instructions on how to prepare for hyperbaric oxygen therapy. You'll be given a hospital-approved gown or scrubs to wear in place of regular clothing during the procedure.
For fire prevention, items such as lighters or battery-powered devices that generate heat are not allowed in the hyperbaric chamber. You also will be asked not to wear or use any hair or skin care products such as lip balm, lotion, makeup or hair spray.
In general, you should not take anything into a chamber unless a member of your healthcare team says it's OK.
What you can expect
During hyperbaric oxygen therapy
Individual hyperbaric oxygen unit, also called monoplace hyperbaric oxygen unit

Individual hyperbaric oxygen unit, also called monoplace hyperbaric oxygen unit
In an individual hyperbaric oxygen unit, a person rests inside a clear plastic tube and receives treatment. This chamber also is called a monoplace hyperbaric oxygen chamber.
Hyperbaric oxygen therapy hood
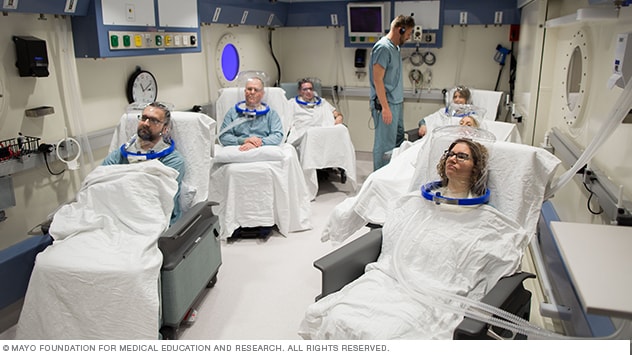
Hyperbaric oxygen therapy hood
Hyperbaric oxygen therapy also can be given to more than one person in a large room. In this case, each person gets oxygen through a lightweight, clear hood.
Hyperbaric oxygen therapy typically is performed as an outpatient procedure, but it also can be provided while you are hospitalized.
In general, there are two types of hyperbaric oxygen chambers:
- A chamber for one person. This chamber, called a monoplace chamber, is a clear tube. You will lie on a bed that slides into the chamber. The air inside the chamber is pressurized, pure oxygen.
- A chamber for several people. A chamber for two or more people is called a multiplace chamber. The normal air in the room is pressurized. Each person inhales pure oxygen through a mask or a clear hood placed over the head.
The treatment effects of hyperbaric oxygen therapy are the same in monoplace and multiplace chambers.
For most conditions, hyperbaric oxygen therapy lasts 1 1/2 to 2 hours. Members of your healthcare team will monitor you throughout your treatment.
After hyperbaric oxygen therapy
Your therapy team assesses you, including looking in your ears and taking your blood pressure and pulse. Once the team decides you are ready, you can get dressed and leave.
You may feel somewhat tired or hungry following your treatment. This doesn't limit your typical activities.
Results
The number of sessions depends on your medical condition. Some conditions, such as carbon monoxide poisoning, might be treated with a few sessions. Other conditions, such as nonhealing wounds, may require 40 treatment sessions or more.
Hyperbaric oxygen therapy is often a part of a broader treatment plan that includes other medical or surgical specialists.
Dec. 06, 2024