Overview
Full-thickness cornea transplant
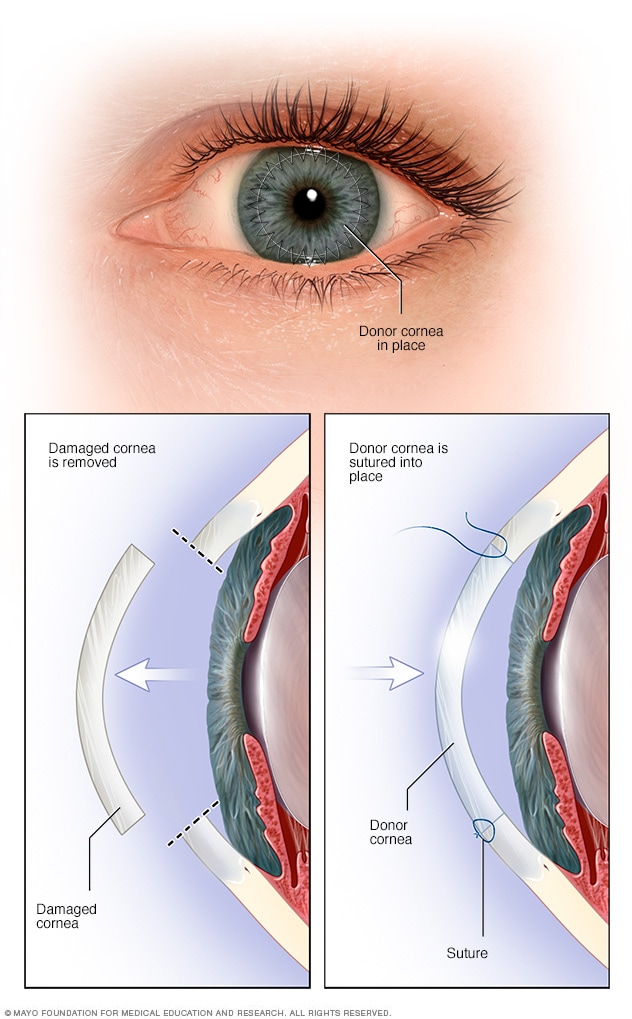
Full-thickness cornea transplant
During a full-thickness cornea transplant, a circular disk-shaped portion of the cornea is removed and replaced with a similarly sized portion of cornea from a donor. This operation is called penetrating keratoplasty.
A cornea transplant is an operation to replace part of the cornea with corneal tissue from a donor. This operation is sometimes called keratoplasty. The cornea is the transparent, dome-shaped surface of the eye. Light enters the eye through the cornea. It plays a large role in the eye's ability to see clearly.
A cornea transplant may:
- Restore vision.
- Reduce pain.
- Improve the appearance of a damaged or diseased cornea.
Most cornea transplant operations are successful. But cornea transplant carries a small risk of complications, such as rejection of the donor cornea.
Products & Services
Why it's done
Anatomy of the eye

Anatomy of the eye
Your eye is a complex and compact structure measuring about 1 inch (2.5 centimeters) in diameter. It receives millions of pieces of information about the outside world, which are quickly processed by your brain.
A cornea transplant is most often used to restore vision to a person with a damaged cornea. A cornea transplant also can relieve pain or other symptoms associated with cornea diseases.
A number of conditions can be treated with a cornea transplant, including:
- A cornea that bulges outward, called keratoconus.
- Fuchs dystrophy, a genetic condition.
- Thinning or tearing of the cornea.
- Cornea scarring, caused by infection or injury.
- Swelling of the cornea.
- Corneal ulcers not responding to medical treatment.
- Complications caused by previous eye surgery.
Risks
Cornea transplant is relatively safe. Still, it does carry a small risk of serious complications, such as:
- Eye infection.
- Pressure increase within the eyeball, called glaucoma.
- Problems with the stitches used to secure the donor cornea.
- Rejection of the donor cornea.
- Bleeding.
- Retinal problems, such as retinal detachment or swelling.
Symptoms of cornea rejection
The body's immune system can mistakenly attack the donor cornea. This is called rejection. Rejection might require medical treatment or another cornea transplant.
Make an urgent appointment with your eye doctor if you notice symptoms of rejection, such as:
- Loss of vision.
- Eye pain.
- Red eyes.
- Sensitivity to light.
Rejection occurs in about 10% of cornea transplants.
How you prepare
Before cornea transplant surgery, you will undergo:
- A thorough eye exam. Your eye doctor looks for conditions that might cause complications after surgery.
- Measurements of your eye. Your eye doctor determines what size donor cornea you need.
- A review of all medications and supplements you're taking. You may need to stop taking certain medications or supplements before or after your cornea transplant.
- Treatment for other eye problems. Unrelated eye problems, such as infection or swelling, can reduce your chances of a successful cornea transplant. Your eye doctor will treat those problems before your surgery.
Finding a donor cornea
Corneas used in transplants come from people who have died. Corneas from people who died from unknown causes are not used. Corneas from people who had previous eye surgery, eye disease or certain conditions, such as diseases that are passed from one person to the next, also are not used.
Unlike people who need organs such as livers and kidneys, people needing cornea transplants don't require tissue matching. In the United States, donor corneas are widely available, so there's usually not a long waiting list.
Operations to transplant a portion of the cornea
A cornea transplant removes either the entire thickness or the partial thickness of the diseased cornea and replaces it with healthy donor tissue. Your cornea surgeon will decide which method to use. These types of operations include:
-
Penetrating keratoplasty. This operation involves a full-thickness cornea transplant. Your surgeon cuts through the entire thickness of the irregular or diseased cornea to remove a small button-sized disk of corneal tissue. A special instrument is used to make this precise circular cut.
The donor cornea, cut to fit, is placed in the opening. Your surgeon then uses stitches, also called sutures, to keep the new cornea in place. The stitches might be removed at a later visit with your eye doctor.
-
Endothelial keratoplasty. There are two types of endothelial keratoplasty. These operations remove diseased tissue from the back corneal layers. The layers include the endothelium and a layer of tissue called the Descemet membrane, which is attached to the endothelium. Donor tissue replaces the removed tissue.
The first type of operation, called Descemet stripping endothelial keratoplasty (DSEK), uses donor tissue to replace up to one-third of the cornea.
The second type of operation, called Descemet membrane endothelial keratoplasty (DMEK), uses a much thinner layer of donor tissue. The tissue used in DMEK is extremely thin and fragile. This operation is more challenging than DSEK but is commonly used.
-
Anterior lamellar keratoplasty (ALK). Two different methods remove diseased tissue from the front corneal layers, including the epithelium and the stroma. However, they leave the back endothelial layer in place.
The depth of cornea damage determines the type of ALK operation that's right for you. Superficial anterior lamellar keratoplasty (SALK) replaces only the front layers of the cornea. This leaves the healthy stroma and endothelium intact.
A deep anterior lamellar keratoplasty (DALK) operation is used when cornea damage extends deeper into the stroma. Healthy tissue from a donor is then attached to replace the removed portion of the cornea. This process is known as grafting.
- Artificial cornea transplant. If you aren't eligible for a cornea transplant with a donor cornea, you might receive an artificial cornea. This operation is known as keratoprosthesis.
Your doctor will discuss which method of cornea transplant surgery is best for you, tell you what to expect during the operation and explain the risks of the operation.
Full-thickness corneal transplants involve removing the diseased cornea and stitching in a new one from a donor. But now, for diseases that affect only the inner lining of the cornea, doctors can do a partial-thickness transplant. This involves removing only the damaged layer and transplanting it with donor tissue.
What you can expect
During the procedure
On the day of your cornea transplant, you'll be given a medicine to help you feel calm or less anxious or a medicine that numbs your eye. Either way, you shouldn't feel pain.
Surgery is done on one eye at a time. The amount of time spent in surgery depends on your situation.
After the procedure
After your cornea transplant, you can expect to:
- Receive medicines. Eye drops and other medicines can help control infection, swelling and pain. Eye drops to suppress the immune system help prevent cornea rejections.
- Wear eye protection. Eye shields or glasses protect your eye as it heals.
- Lie on your back. Depending on the type of transplant, you might have to do this for a while after surgery. This helps the new tissue stay in place.
- Avoid injury. Plan to take it easy after your cornea transplant. When approved by your eye surgeon, slowly work your way up to your typical activities, including exercise. Don't rub or press on your eye. For the rest of your life, you'll need to take extra precautions to avoid harming your eye.
- Return for frequent follow-up exams. Expect to see your eye doctor regularly in the year after surgery. This is to monitor your progress and look for complications.
Results
Most people who receive a cornea transplant will have their vision at least partially restored. What you can expect after your cornea transplant depends on your health and the reason for your surgery.
Your risk of complications and cornea rejection continues for years after your cornea transplant. For this reason, see your eye doctor yearly. Cornea rejection can often be managed with medicines.
Vision correction after surgery
At first, your vision might be worse than it was before your surgery. Your eye needs time to adjust to the new cornea. It can take several months for your vision to improve.
It may take several weeks to several months after surgery for the outer layer of your cornea to heal. When it heals, your eye doctor will make adjustments that can improve your vision, such as:
- Correcting unevenness in your cornea. The stitches that hold the donor cornea in place on your eye might cause irregularities in your cornea. This uneven surface can cause astigmatism. Astigmatism can make your vision blurry. Your eye doctor might address the astigmatism by releasing some stitches.
- Correcting vision problems. Refractive errors, such as nearsightedness and farsightedness, can be corrected. Your eye doctor may recommend glasses, contact lenses or, in some cases, laser eye surgery.
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.
Sept. 19, 2024