Feb. 16, 2021
Mayo Clinic uses the latest technology for shoulder replacement surgery, including analytical tools that provide understanding of an individual patient's glenoid wear pattern. Sophisticated preoperative planning and the use of patient-specific instrumentation are key to optimizing glenoid component choice and position and maximizing surgical outcomes.
"We've learned over time that understanding the glenoid bone's three-dimensional anatomy is enormously helpful in planning shoulder replacement surgery," says John W. Sperling, M.D., an orthopedic surgeon at Mayo Clinic in Rochester, Minnesota. "These tools allow us to develop a surgical plan based on the individual patient's anatomy and then to accurately execute that plan once we get to the operating room."
3D surgical and depth control guides
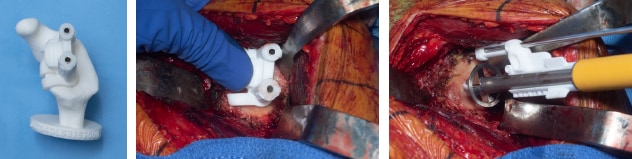
3D surgical and depth control guides
On the left, photograph shows a 3D glenoid model with a patient-specific guide. In the center, perioperative photograph shows the patient-specific guide matching the patient's glenoid surface. On the right, perioperative photograph shows a depth control guide for glenoid reaming, to maximize the preservation of glenoid bone.
With the highest-volume shoulder replacement practice in the United States, Mayo Clinic is at the forefront of advances in this complex procedure. In addition to implementing 3D surgical guides based on an individual patient's anatomy, Mayo's orthopedic surgeons use recently developed depth controls for glenoid reaming.
"A 3D-printed guide attached to the reamer allows for precise preparation of the glenoid surface and maximizes glenoid bone preservation," Dr. Sperling says. "During surgery, the depth control helps us prepare the glenoid in the manner that we planned preoperatively."
Initially, patient-specific instrumentation was reserved for patients with complex anatomy, including dysplasia, bone deficiency or deformity secondary to prior trauma. "But due to the benefits we've seen, we are broadening our use to the full range of conditions, from minimal glenoid deformity to highly complex underlying shoulder pathologies," Dr. Sperling says.
Mayo Clinic's team approach facilitates this individualized orthopedic care. The CT scans needed for pre-surgical planning and patient-specific instrumentation can be pre-scheduled to coordinate with surgical and medical appointments. "The patient experience here is very time efficient," Dr. Sperling says.
The CT scans are uploaded to a system that uses advanced software to allow the surgeon to plan the orthopedic procedure and order patient-specific surgical guides. "In the operating room, the preoperative plan and patient-specific instrumentation increase the procedure's efficiency," Dr. Sperling says. "We can execute our plan to preserve bone and optimize the positioning of the implant."
Augmented baseplate for reverse shoulder arthroplasty
Augmented glenoid baseplate
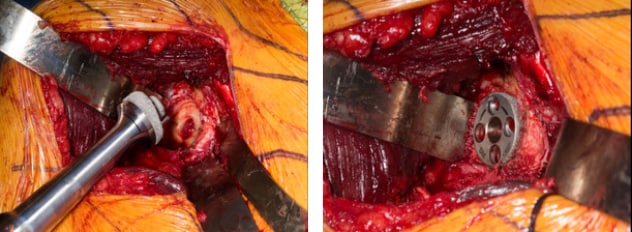
Augmented glenoid baseplate
Perioperative photographs show the use of an augmented glenoid baseplate. On the left, an augmented glenoid baseplate is placed in a patient. On the right, the augmented baseplate's ability to create tilt and provide lateralization are demonstrated.
To preserve glenoid bone in patients who have reverse shoulder arthroplasty, Dr. Sperling uses an augmented glenoid baseplate.
"The augmented component minimizes bone removal compared with eccentric reaming, preserves the best-quality cortical bone and allows for longer screw fixation," Dr. Sperling says. "Recent research has shown that the routine use of augmented baseplates in reverse arthroplasty, along with preoperative planning, can result in over 50% preservation of glenoid bone compared with the use of a standard glenoid baseplate."
As the major shoulder arthroplasty center in the United States, Mayo Clinic is committed to continued innovation. "In the future, as preoperative planning and patient-specific instrumentation continue to evolve, we will be able to further customize our procedures for individual patients," Dr. Sperling says.