May 22, 2018
Significant papilledema in a young female diagnosed with Henoch-Schonlein purpura IgA vasculitis
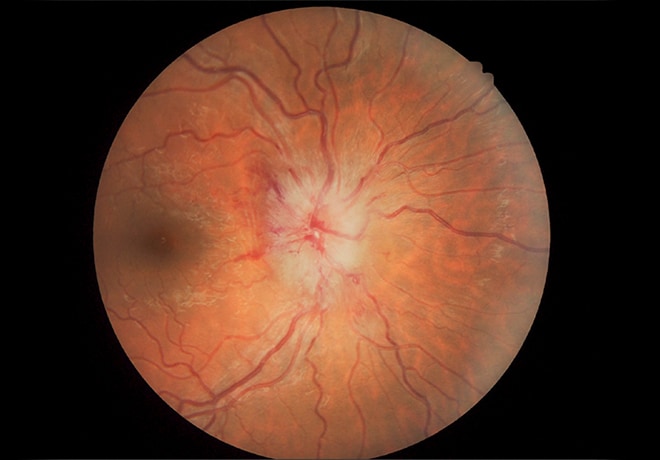
Significant papilledema in a young female diagnosed with Henoch-Schonlein purpura IgA vasculitis
The papilledema is due to elevated intracranial pressure secondary to a cerebral venous sinus thrombosis, presumably associated with the vasculitis. She has visual field compromise and is being closely medically managed on an anticoagulant and a diuretic prior to determining if optic nerve decompression surgery is warranted. Her treatment at Mayo Clinic involves a multidisciplinary approach including specialists in neurology, neuro-ophthalmology, hematology and rheumatology.
Mayo Clinic provides subspecialized team care for people with neurological disorders affecting their vision and visual pathways. At all three Mayo Clinic campuses, neuro-ophthalmologists work closely with Mayo's neurologists and neurosurgeons to treat people with any problems involving sight or eye movement that arise from the nervous system, including issues caused by:
- Tumors
- Migraine
- Stroke
- Multiple sclerosis (MS)
- Radiation treatment
- Idiopathic intracranial hypertension
- Cerebral venous sinus thrombosis
- Parkinsonian disorders
- Traumatic brain injury
"Neuro-ophthalmologists are sort of a rare breed. We are a subspecialty of both neurology and ophthalmology, and there aren't many of us practicing full time," says Marie D. Acierno, M.D., a neuro-ophthalmologist at Mayo Clinic in Phoenix/Scottsdale, Arizona. "We have unique training to evaluate patients from the neurological, ophthalmological and medical standpoints."
As a fully integrated group practice, Mayo Clinic can offer patients the subspecialized evaluations they need in a single day. "A patient might come in to have neuroimaging, then have a visual-system assessment and then go on to see the neurosurgeon," Dr. Acierno says.
"It's important to transfer all this information," she adds. "For example, because the pituitary gland sits across the visual pathway, a pituitary tumor of sufficient size can compromise the visual field. A complete neuro-ophthalmological evaluation can help a neurosurgeon make a better surgical decision for the patient."
For nonsurgical cases, neuro-ophthalmologists provide expertise for patients with visual disorders associated with an underlying condition, such as migraine.
"As our neurologists work to control the frequency and severity of a patient's migraine episodes, the neuro-ophthalmologist can advise on the visual disturbance that a patient might have during the episodes," Dr. Acierno says. "These disturbances are often frustrating and worrisome for patients. As neuro-ophthalmologists, we can let these patients know that their ocular and visual systems are intact and that this experience is part of their migraine events."
Patients who experience visual loss after a stroke can also benefit from a neuro-ophthalmological evaluation. "These patients might not realize that the visual loss isn't coming from the ocular system itself, but emanating from the brain or the nervous system if the stroke has affected the visual cortex of the brain," Dr. Acierno says.
In addition, people with MS are a large part of Mayo's neuro-ophthalmological practice. "We have many referrals of patients with MS who experience optic neuritis, eye-movement disorders, problems with ocular motility or double vision," Dr. Acierno says.
For Mayo's neuro-ophthalmologists, collaboration extends beyond the fields of neurology and neurosurgery. Dr. Acierno often works with radiation oncologists to treat patients who experience visual problems after radiation treatment for cancer. She also hopes to start a combined service — with neurologists, neurosurgeons and bariatric surgeons — for people with idiopathic intracranial hypertension.
"Many of these patients can lose vision due to the elevated intracranial pressure and may require surgery to decompress the optic nerve or a shunt to relieve pressure from cerebrospinal fluid," Dr. Acierno says. "That surgery might be done by a neuro-ophthalmologist or by a neurosurgeon. In addition, our neurologists work to control these patients' headaches. But it's also important for these patients to lose weight, which might involve bariatric surgery.
"As a center of excellence in the neurosciences, Mayo Clinic has subspecialists in place to offer the best care for patients," she adds.