Feb. 28, 2020
As a fully integrated and multidisciplinary center, Mayo Clinic provides comprehensive care for people with spinal tumors. All three Mayo Clinic campuses have expertise with the range of treatments for primary and metastatic disease.
"We take a holistic approach to spinal oncology," says Maziyar A. Kalani, M.D., a neurosurgeon at Mayo Clinic in Phoenix/Scottsdale, Arizona. "In addition to surgery, we use decompression, stabilization, various ablation technologies and minimally invasive cement augmentation. We offer the gamut of available treatments to meet whatever needs an individual patient has."
That capability rests upon Mayo's enterprisewide, multidisciplinary expertise. Neurosurgeons collaborate with neuroradiologists, oncologists, radiation oncologists, and specialists in physical medicine and rehabilitation (PM&R).
"We have a high-volume practice in both primary and metastatic tumors, and a number of specialists in each department at each site who are experts in spinal oncology," says Mohamad Bydon, M.D., a neurosurgeon at Mayo Clinic in Rochester, Minnesota.
Coordinating care in these complex cases requires strong communication among medical services. Neurosurgeons, neuroradiologists and radiation oncologists routinely confer on challenging cases.
"Our ability to communicate with providers from different specialties who are all on one campus — as well as to obtain input from colleagues from the other two campuses — allows us to maximize the benefits of team management for our patients," says Kingsley Abode-Iyamah, M.D., a neurosurgeon at Mayo Clinic in Jacksonville, Florida. "That ability is especially important when we deal with rare and technically challenging spinal tumors. Our combined experience helps us to better benefit each patient."
Blending technology and patient-focused care
Mayo Clinic uses the latest technology for the expeditious diagnosis and treatment of spinal tumors. "Our ability to get high-resolution MRI scans and radionucelotide studies, such as positron emission tomography and single-photon emission computerized tomography, helps with both diagnostic quandaries and pre-surgical planning," says Selby G. Chen, M.D., a neurosurgeon at Mayo Clinic's campus in Florida.
Proton beam therapy, which allows radiation delivery to conform more closely to the tumor, is available at Mayo Clinic's campuses in Arizona and Minnesota. The pencil beam technology used at Mayo offers added precision by delivering protons in a raster pattern at different specific depths, to better conform to the volume of the tumor.
Mayo Clinic also uses recently approved carbon fiber implants, which can allow for lower radiation doses than traditional titanium hardware. "Titanium is so dense that the protons can bounce off when it's implanted in patients," Dr. Kalani says. "To compensate, radiation oncologists have to increase the depth of penetration and the proton dosage. Carbon fiber is a composite, not a metal, so it avoids that issue."
Decisions about the use of technology are based on each patient's needs. Mayo Clinic's multidisciplinary approach is aimed at devising the optimal individualized treatment plan — avoiding unnecessary surgery and employing complementary treatment modalities when they can help improve treatment outcome and survival.
"We try to adopt minimally invasive approaches whenever appropriate, to help speed recovery and decrease postoperative pain," Dr. Chen says. "However, when larger surgeries are needed, we don't hesitate to do a more extensive operation that may involve multiple spinal surgeons as well as vascular surgeons, general surgeons or orthopedic surgeons."
Decision-making is enhanced by Mayo Clinic's high-volume practice in spinal oncology. "We have enough patient volume to continuously follow our metrics and improve patient care. We have the numbers to drive change," says Michelle (M.J.) J. Clarke, M.D., a neurosurgeon at Mayo Clinic in Rochester, Minnesota.
Extensive syrinx associated with an intramedullary hemangioblastoma
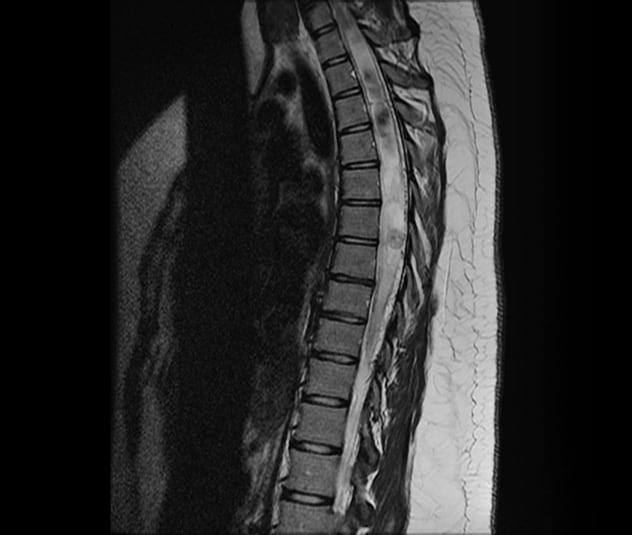
Extensive syrinx associated with an intramedullary hemangioblastoma
T2-weighted MRI shows an extensive syrinx associated with an intramedullary hemangioblastoma in a 19-year-old woman with von Hippel-Lindau disease.
Technology and the commitment to patient-focused care allow Mayo Clinic to manage even the most complex spinal tumors. Dr. Bydon cites the recent case of a 19-year-old woman with von Hippel-Lindau disease who was successfully treated at Mayo Clinic's campus in Minnesota. The patient had an intramedullary hemangioblastoma with extensive syrinx.
"The tumor was large," Dr. Bydon says. "It encompassed the patient's spine and resulted in an accumulation of fluid that was damaging the spinal cord." The patient experienced weakness in her legs and symptoms of myelopathy.
The surgical treatment, which included laminectomy and tumor resection, was complicated by the tumor's size and location in the spinal cord. "We had to navigate around the spinal cord and very carefully dissect the blood vessels, to avoid removing any vessels important to the spinal cord," Dr. Bydon says.
No residual tumor and resolution of the syrinx

No residual tumor and resolution of the syrinx
Postoperative MRI demonstrates no residual tumor and resolution of the syrinx in the patient with von Hippel-Lindau disease.
The patient emerged from tumor resection with improvement in her legs and was able to leave the hospital two days later. "The tumor has been removed in whole, and the syrinx is resolving," Dr. Bydon says.
Surgery is only one aspect of the comprehensive care that patients with spinal tumors need. Mayo Clinic's specialists in PM&R provide extensive rehabilitation after spinal operations. In addition, patients with a genetic condition such as von Hippel-Lindau disease can be followed by medical geneticists and other specialists as needed.
"When patients are referred to Mayo, we look after all their needs," Dr. Kalani says. "If patients are too sick for surgery, we don't have to operate. But we can provide other treatment to ease their symptoms. We can help preserve quality of life."