April 26, 2019
Neuron in the substantia nigra with Lewy bodies
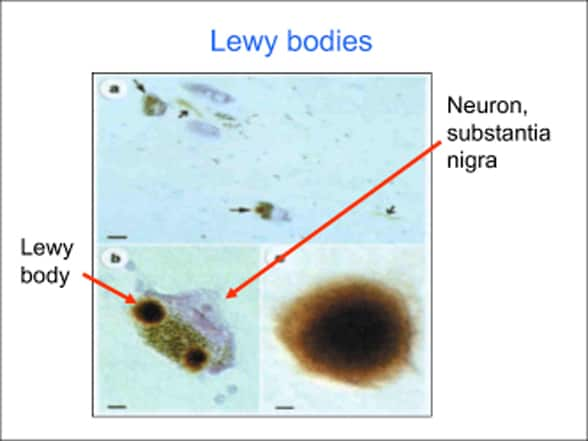
Neuron in the substantia nigra with Lewy bodies
Image of a neuron in the substantia nigra shows Lewy bodies, the pathology hallmark of Parkinson's disease.
Although Parkinson's disease typically affects people over the age of 65, the condition can develop years earlier. Mayo Clinic is launching a young-onset Parkinson's disease clinic to meet the distinct needs of people who have a diagnosis of this neurodegenerative condition at a younger age.
"The implications are very different for patients in the prime of life who are still working, perhaps raising children and have an active lifestyle," says Rodolfo Savica, M.D., Ph.D., a neurologist at Mayo Clinic in Rochester, Minnesota. "There is an entire spectrum of limitations that these patients must deal with, beyond tremor, rigidity or stiffness. It can be devastating."
Timeline of events, signs and symptoms
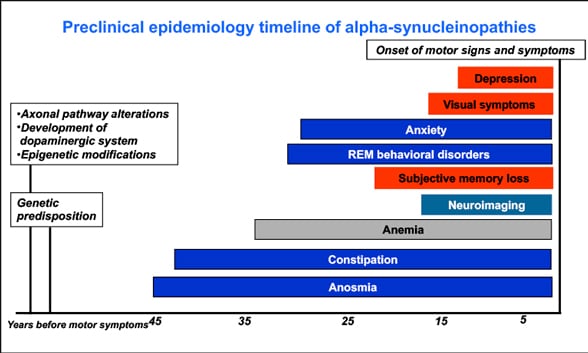
Timeline of events, signs and symptoms
Chart illustrates the timeline of events, signs and symptoms that precede Parkinson's disease.
Sleep disturbances, anxiety and depression are common. "These problems frequently occur prior to the movement troubles that help cinch the diagnosis of Parkinson's disease. They're also often far more disabling in young-onset Parkinson's than are the motor troubles experienced early in the course of the disease," says Ryan J. Uitti, M.D., a neurologist at Mayo Clinic in Jacksonville, Florida. "We should always address quality of life for people with Parkinson's disease, but that's particularly important for younger patients."
Efficient multidisciplinary care
As a tertiary center, Mayo Clinic has experience with the diagnosis and treatment of uncommon conditions such as young-onset Parkinson's disease. No specific age cutoff defines young onset, but most patients are in their 50s.
"A younger patient might not have the classic tremor, but might instead present with a lower extremity dystonia or perhaps upper extremity stiffness or rigidity," says Shyamal H. Mehta, M.D., Ph.D., a neurologist at Mayo Clinic in Phoenix/Scottsdale, Arizona. "The diagnosis can be delayed in these younger patients because the possibility of Parkinson's disease might not be considered."
SPECT brain imaging visualization of the striatal dopamine transporter
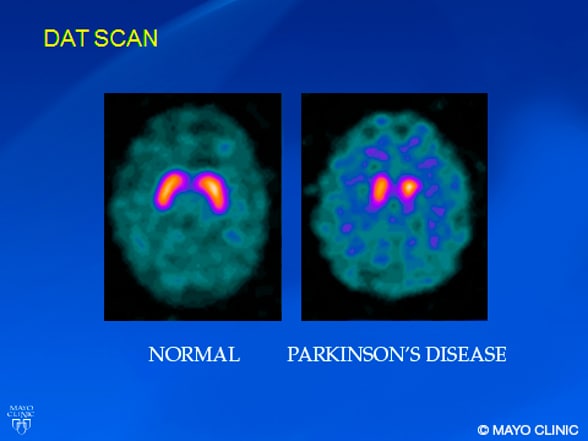
SPECT brain imaging visualization of the striatal dopamine transporter
After injection of the radioligand ioflupane (DaTscan), single-photon emission computerized tomography (SPECT) brain imaging provides visualization of the striatal dopamine transporter. This technique is of diagnostic value in patients with young-onset Parkinson's disease, who may present with atypical signs and symptoms.
At Mayo, the young-onset Parkinson's disease clinic is designed to provide multidisciplinary evaluation and management in a single two-day visit. Laboratory testing is performed, as well as neuroimaging when needed. Mayo Clinic uses state-of-the-art diagnostic tools, including electrophysiological testing, functional imaging and radionuclide injections. Radionuclide testing is often recommended in younger patients to support a clinical diagnosis of Parkinson's disease.
Patients then typically see specialists in:
- Movement disorders
- Sports medicine, who can provide advice geared to individuals' favored exercise, such as cycling or swimming
- Sleep medicine
- Genetics, who can advise on genetic variations that might increase the risk of Parkinson's disease for family members
- Integrative medicine
Before patients arrive at Mayo Clinic, they complete intake questionnaires about their problems and concerns. "This allows us to set up additional specialist appointments as needed — for example, in urology, psychiatry, and men's or women's health," Dr. Savica says. "The entire set of specialists is ready for the patient when he or she arrives."
During their visits, patients might be offered opportunities to participate in research. Before leaving Mayo, patients receive a summary of the information provided to them. Full reports are also sent to patients' local clinicians.
To minimize the need for in-person follow-up, Mayo Clinic is developing methods for ongoing contact via personal electronic media. "Staying in close contact electronically with patients and their local clinicians allows us to suggest changes in therapy that can improve quality of life, without patients' having to make three or four visits to Mayo a year. This is very important for people who are working and have families," Dr. Uitti says.
Individualized treatment and therapeutic trials
Therapy for young-onset Parkinson's disease depends on a patient's needs and level of impairment. "Our recommendations are guided by the differing disease course we typically see in young-onset Parkinson's disease," Dr. Savica says. "Young-onset patients usually, but not always, have more dyskinesias. However, because of the rarity of young-onset Parkinson's disease, there is much about the disease course that is still unclear."
Placement of bipallidal and bithalamic DBS electrodes
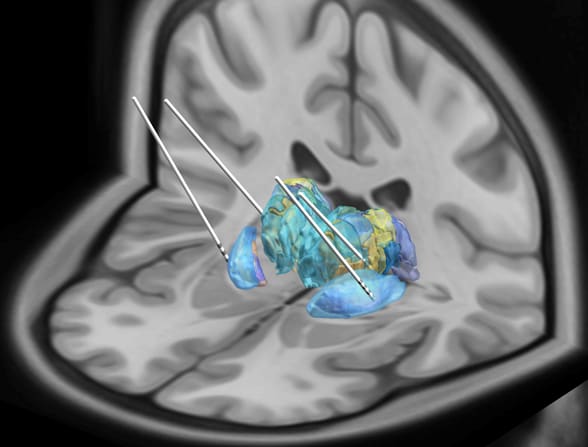
Placement of bipallidal and bithalamic DBS electrodes
Image shows the placement of bipallidal and bithalamic deep brain stimulation (DBS) electrodes for treatment of Parkinson's disease.
In addition to medication, deep brain stimulation (DBS) is a treatment option at all three Mayo Clinic campuses. "If we are unable to ameliorate a patient's symptoms adequately with medication, we may put in as many as four brain electrodes rather than the standard two. We have found that this can significantly improve patients' quality of life," Dr. Uitti says.
"Our preferred DBS system has eight electrodes that can be used individually or in combination with one another, which gives us a lot of flexibility to influence the brain."
As a leader in Parkinson's disease research, Mayo Clinic provides opportunities for patients to participate in therapeutic trials of new medications and surgical techniques. Mayo also offers genetic testing and biobanking of DNA for people with Parkinson's disease so they can be notified of any future treatments that might benefit them. Among the approximately 20 genes associated with Parkinson's disease, Mayo Clinic discovered three, including the most common, LRRK2.
Mayo's physician-researchers also have extensive longitudinal data from patients treated for Parkinson's disease. "Like anyone facing a serious condition, people with young-onset Parkinson's disease want to know what the crystal ball looks like. We have decades of experience making observations on disease course and treatments that might lead to the best results," Dr. Uitti says.
"Many of these younger patients will have Parkinson's disease for 10, 20 or 30 years," he adds. "We are in it for the long run with them."
For more information
Young-Onset Parkinson's Disease Clinic. Mayo Clinic.
Refer a patient to Mayo Clinic.