April 23, 2022
Mayo Clinic routinely uses spinal anesthesia when performing certain minimally invasive spinal surgeries. Compared with surgeries done under general anesthesia, the awake procedures generally result in shorter operating room time and less postoperative pain.
"This is a real paradigm shift in neurosurgery," says Kingsley Abode-Iyamah, M.D., a neurosurgeon at Mayo Clinic in Jacksonville, Florida. "Our studies are showing that spinal anesthesia not only is safe but also offers real benefits for patients."
Innovative technique
Innovative technique
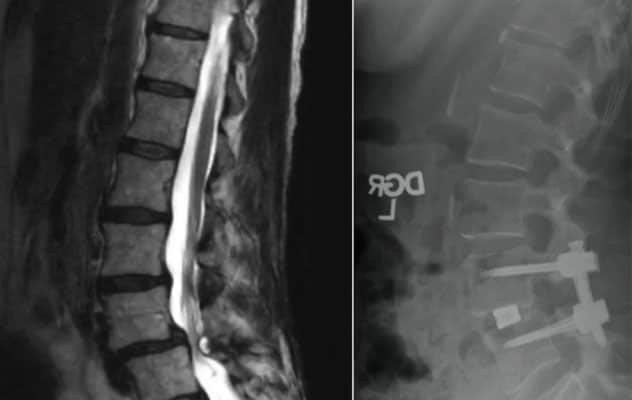
On the left, preoperative MRI shows spinal curvature before awake minimally invasive surgery-transforaminal lumbar interbody fusion (MIS-TLIF) at Mayo Clinic. On the right, postoperative image shows the correction achieved during the awake procedure.
Mayo Clinic's spinal anesthesia protocol is used for selected individuals undergoing laminectomy, diskectomy or minimally invasive surgery-transforaminal lumbar interbody fusion (MIS-TLIF). The procedures are completed within 2 to 3 hours — the typical duration of spinal anesthesia.
A Mayo Clinic study to be published in World Neurosurgery found that 60% of individuals undergoing lumbar spinal surgery were willing to participate in a randomized trial of spinal anesthesia versus general anesthesia.
"There has been a perception that patients would not be willing to undergo this type of surgery awake," Dr. Abode-Iyamah says. "But in our experience, spinal anesthesia improves patients' overall satisfaction."
Documenting the benefits for patients
The adverse effects of general anesthesia for individuals undergoing spinal surgery can include memory loss, nausea, and transient impairment of sensory and motor functions. "In older individuals, general anesthesia might also affect cognition," Dr. Abode-Iyamah says.
The specific advantages of spinal anesthesia — as described in two Mayo Clinic studies published in the December 2021 issue of Neurosurgical Focus — include:
- A 27% reduction in total operating room time
- Lower mean overall and mean maximum pain scores in the first three hours after surgery
- Ambulation on average 7.8 hours earlier than ambulation after general anesthesia
- Shorter hospital stays
Awake spinal surgery is a multidisciplinary effort. "It requires neurosurgeons and anesthesiologists who are not only experts in their fields but also comfortable working together," Dr. Abode-Iyamah says.
The awake procedures are performed with patients in the prone position. Mayo Clinic recommends avoiding spinal anesthesia for patients with obstructive sleep apnea or a body mass index of 35 or above, as those individuals might have an increased risk of carbon dioxide accumulation during the surgery.
Mayo Clinic's techniques for safely performing awake MIS-TLIF are described in a technical note published in the January 2021 issue of the Journal of Clinical Neurology and Neurosurgery. The procedure is used only for one- or two-level fusions due to the time constraint of spinal anesthesia. Mayo Clinic further enhances awake MIS-TLIF by using robotic technology to guide screw placement.
During all awake spinal surgeries, patients wear noise-canceling headphones and listen to music of their choice. "They can communicate with us at any time, and we can communicate with them, making sure they are comfortable and doing well," Dr. Abode-Iyamah says.
Mayo Clinic plans to undertake a randomized prospective clinical trial comparing spinal surgery performed with spinal anesthesia and that performed with general anesthesia.
"The dominance of general anesthesia is probably due to a lack of exposure to spinal anesthesia," Dr. Abode-Iyamah says. "At Mayo Clinic, we are committed to innovating our approaches in ways that help patients."
For more information
De Biase G, et al. Assessment of patients' willingness to participate in a randomized trial of spinal versus general anesthesia for lumbar spine surgery. World Neurosurgery. In press.
De Biase G, et al. Spinal versus general anesthesia for minimally invasive transforaminal lumbar interbody fusion: Implications on operating room time, pain, and ambulation. Neurosurgical Focus. 2021;51:e3.
Abode-Iyamah K, et al. Single-level awake transforaminal lumbar interbody fusion: A Mayo Clinic institutional experience and national analysis. Neurosurgical Focus. 2021;51:e4.
De Biase G, et al. Awake minimally invasive transforaminal lumbar interbody fusion with a pedicle-based retraction system. Clinical Neurology and Neurosurgery. 2021;200:106313.
Refer a patient to Mayo Clinic.