Overview
Peutz-Jeghers syndrome (POOTZ-JAH-erz syndrome) is a rare genetic condition that causes small clumps of tissue called polyps in the digestive tract. It also causes dark spots on the lips, mouth, genitals, hands and feet that may look like freckles. Peutz-Jeghers syndrome (PJS) is linked to occurrence of several cancers.
The most common and easily recognized type of polyp with PJS is called a hamartomatous polyp. These polyps usually appear in the small intestine, stomach and colon. They are made of regular tissue that grows in a way that's not organized. Other types of polyps — including adenomatous polyps, which are precancerous — also can form in people with PJS. The dark spots in the skin usually show up in childhood and may fade in adulthood.
Peutz-Jeghers syndrome is not common. Studies estimate it happens in about 1 in 50,000 to 200,000 births.
The polyps in PJS can cause complications. Most of the polyps usually are not cancerous or precancerous, sometimes called premalignant. And the possibility of any single polyp becoming cancerous is probably low. But people with PJS have a very high risk of several cancers. These include cancers of the stomach, small intestine, colon, pancreas, breast and reproductive organs.
Regular testing is recommended to screen for cancer and other complications.
Symptoms
The symptoms of Peutz-Jeghers syndrome can be caused by polyps in the digestive tract and changes in the skin.
Common symptoms
Peutz-Jeghers syndrome polyps may cause signs and symptoms, such as:
- Blood in the stool, which may look like red streaks or make the stool look black.
- Tiredness or weakness, which can be caused by low level of red blood cells, called iron deficiency anemia.
- Belly pain.
- Vomiting.
- Diarrhea.
These symptoms can happen when polyps bleed, grow large or block part of the intestines.
Peutz-Jeghers syndrome skin signs and symptoms may include:
- Dark spots on the lips and inside or around the mouth.
- Dark spots on the genitals, fingers, palms of the hands or soles of the feet.
These spots, which may look like freckling, often appear before age 5. They may fade over time but remain inside the mouth.
Less common symptoms
Although less common, Peutz-Jeghers syndrome also can cause symptoms involving the reproductive organs.
- Breast growth called gynecomastia in boys. This can happen if the condition causes tumors that make estrogen in the testicles.
- Early puberty in girls. This can happen if the condition causes ovarian tumors.
When to see a doctor
Seek care if new dark spots appear on the lips, around or inside the mouth, on the genitals, or on the hands or feet, especially in a child. These can be early signs of PJS. Also seek care as soon as possible if you have any of the other signs or symptoms of Peutz-Jeghers syndrome. These can happen when polyps bleed, grow or block part of the intestine.
When to seek emergency care
Get emergency care right away for:
- Sudden, severe belly pain or repeated vomiting. This can be a sign of a complication called intussusception, when the bowel slides into itself and causes a blockage. It can be dangerous if it is not treated quickly.
- Heavy rectal bleeding or rectal bleeding along with feeling very weak or dizzy. These can be signs of serious blood loss.
Causes
Autosomal dominant inheritance pattern
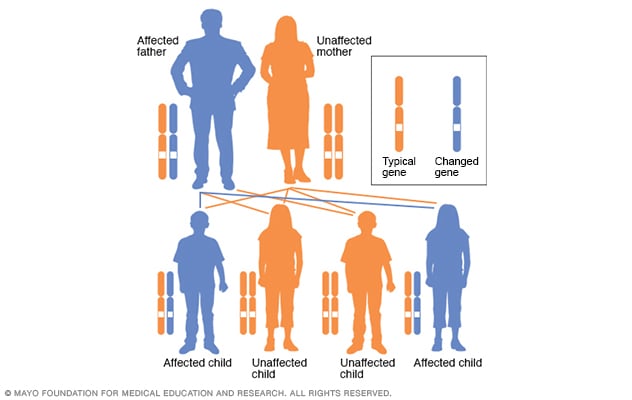
Autosomal dominant inheritance pattern
In an autosomal dominant condition, the changed gene is a dominant gene. It's located on one of the nonsex chromosomes, called autosomes. Only one changed gene is needed to be affected by this type of condition. A person with an autosomal dominant condition — in this example, the father — has a 50% chance of having an affected child with one changed gene. The person has a 50% chance of having an unaffected child.
Peutz-Jeghers syndrome is caused by a change called a mutation in a gene called STK11. This gene helps control how cells grow, repair themselves and die. When the gene does not work as usual, cells may grow in an unorganized way.
Most people with PJS — about 80% to 90% — inherit the gene mutation from a parent. The other 10% to 20% of people with PJS do not inherit it. Instead, they experience a new gene change called a de novo mutation. Why this happens is not known.
When PJS is inherited, a person only needs to inherit one mutated copy of the gene from a parent to have the condition. This is called an autosomal dominant pattern.
The dark spots and color changes that look like freckling on the lips, around the mouth, or on the genitals, hands and feet are caused by pigment building up in the skin. Sometimes this pigment, called melanin, collects in immune cells in the skin. They are called macrophages. Sometimes the skin layers have more melanin and more of the cells that make melanin, called melanocytes.
The hamartomatous polyps that form in the digestive tract happen when tissue in the tract grows in a way that is not organized. Exactly why hamartomatous polyps form is not known. But researchers think it may be that the STK11 gene change affects how cells grow and divide, which can allow the polyps to develop.
Risk factors
Family history is the main risk factor for Peutz-Jeghers syndrome. A person needs only one changed copy of the STK11 gene to have the condition. So if either parent has the condition, their child has a 50% chance of inheriting it.
Both children and adults can have Peutz-Jeghers syndrome. About a third of those with PJS have symptoms during their first 10 years of life. By age 20, about 60% of those with the condition have symptoms. If a person has Peutz-Jeghers syndrome, family members usually should be screened and tested.
Complications
Peutz-Jeghers syndrome can cause a higher risk of certain cancers. Other complications are a result of polyps that bleed or grow in the digestive tract.
Cancers
People with Peutz-Jeghers syndrome have a higher chance of developing cancer both in and outside the digestive tract. For those with PJS, the risk of developing a cancer at some point during life is roughly between about 40% and 93%. The risk goes up with age. The average age of cancer diagnosis in someone with PJS is 42.
Some common types of cancer with PJS — and the percentage of people who get them over a lifetime — include:
Noncancerous tumors
Peutz-Jeghers syndrome also can lead to noncancerous tumors in the reproductive organs.
- A type of testicular tumor can happen in boys. These tumors, called Sertoli cell tumors, make estrogen. They can cause breast growth called gynecomastia and affect height.
- A type of ovarian tumor can form in girls and women. These tumors, called sex cord tumors, usually are not cancerous but can lead to early puberty.
Complications caused by polyps
Polyps can lead to serious symptoms or medical problems, such as:
Prevention
There is no known way to prevent Peutz-Jeghers syndrome. PJS usually is an inherited genetic condition caused by a change in the STK11 gene. However, early testing and regular follow-up care can help manage and prevent some serious complications.
If you or someone else in your family has PJS, other family members can get genetic testing. If a person is found to have the changed gene that causes PJS, regular screening can help find polyps, cancer and other problems early, before they become an emergency. Regular screening also helps find and treat cancer early when treatment might be more successful.
Feb. 21, 2026