Overview
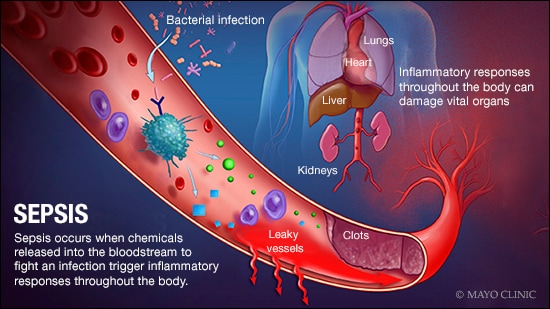
Sepsis is a serious condition in which the body responds improperly to an infection. The infection-fighting processes turn on the body, causing the organs to work poorly.
Sepsis may progress to septic shock. This is a dramatic drop in blood pressure that can damage the lungs, kidneys, liver and other organs. When the damage is severe, it can lead to death.
Early treatment of sepsis improves chances for survival.
Symptoms
Symptoms of sepsis
Symptoms of sepsis may include:
- Change in mental status.
- Fast, shallow breathing.
- Sweating for no clear reason.
- Feeling lightheaded.
- Shivering.
- Symptoms specific to the type of infection, such as painful urination from a urinary tract infection or worsening cough from pneumonia.
Symptoms of sepsis are not specific. They can vary from person to person, and sepsis may appear differently in children than in adults.
Symptoms of septic shock
Sepsis may progress to septic shock. Septic shock is a severe drop in blood pressure. Progression to septic shock raises the risk of death. Symptoms of septic shock include:
- Not being able to stand up.
- Strong sleepiness or hard time staying awake.
- Major change in mental status, such as extreme confusion.
When to see a doctor
Any infection could lead to sepsis. Go to a health care provider if you have symptoms of sepsis or an infection or wound that isn't getting better.
Symptoms such as confusion or fast breathing need emergency care.
From Mayo Clinic to your inbox
Causes
Any type of infection can lead to sepsis. This includes bacterial, viral or fungal infections. Those that more commonly cause sepsis include infections of:
- Lungs, such as pneumonia.
- Kidney, bladder and other parts of the urinary system.
- Digestive system.
- Bloodstream.
- Catheter sites.
- Wounds or burns.
Risk factors
Some factors that increase the risk infection will lead to sepsis include:
- People over age 65.
- Infancy.
- People with lower immune response, such as those being treated for cancer or people with human immunodeficiency virus (HIV).
- People with chronic diseases, such as diabetes, kidney disease or chronic obstructive pulmonary disease (COPD).
- Admission to intensive care unit or longer hospital stays.
- Devices that go in the body, such as catheters in the vein, called intravenous, or breathing tubes.
- Treatment with antibiotics in the last 90 days.
- A condition that requires treatment with corticosteroids, which can lower immune response.
Complications
As sepsis worsens, vital organs, such as the brain, heart and kidneys, don't get as much blood as they should. Sepsis may cause atypical blood clotting. The resulting small clots or burst blood vessels may damage or destroy tissues.
Most people recover from mild sepsis, but the mortality rate for septic shock is about 30% to 40%. Also, an episode of severe sepsis raises the risk for future infections.