Diagnosis
Kidney biopsy
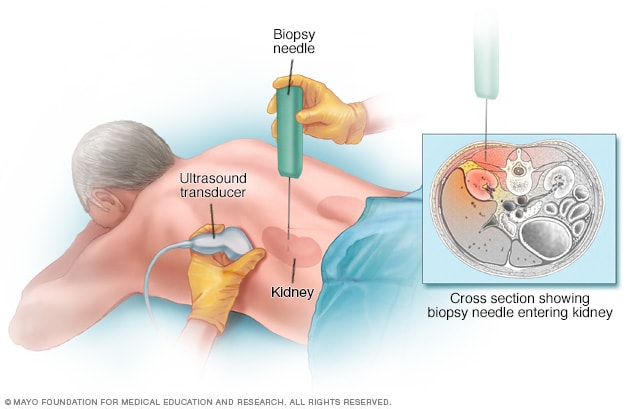
Kidney biopsy
During a kidney biopsy, a healthcare professional uses a needle to remove a small sample of kidney tissue for lab testing. The biopsy needle is inserted through the skin and often is directed using the guidance of an imaging device, such as ultrasound.
To diagnose end-stage kidney disease, your doctor or other healthcare professional may talk with you about your medical history and ask about your family's medical history. You may have a physical exam and neurological exam. Other tests to diagnose kidney disease might include:
- Blood tests. Kidney function tests look for the level of waste products in the blood. Waste products include creatinine and urea.
- Urine tests. Checking a sample of urine can reveal signs of chronic kidney disease. Urine tests also could provide clues about what's causing kidney disease.
- Imaging tests. A healthcare professional might use ultrasound to view the kidneys. Ultrasound can show the structure and size of the kidneys. Other imaging tests might be used in some cases, such as an MRI or CT scan.
- Removing a sample of kidney tissue for testing. A healthcare professional might recommend a kidney biopsy. This procedure removes a sample of kidney tissue for testing in a lab. During a kidney biopsy, a long, thin needle is inserted through the skin and into a kidney. The biopsy sample is sent to a lab for testing. In the lab, tests can help reveal what's causing a kidney problem.
Results from these tests help your healthcare team create a treatment plan for you. Certain tests might be repeated over time to help track changes in your condition.
Stages of kidney disease
There are five stages of kidney disease. To learn what stage you have, a healthcare professional performs a blood test to get an estimate of how well your kidneys are working. The test is called the estimated glomerular filtration rate (eGFR). It measures how much blood the kidneys filter each minute. The results are recorded as milliliters per minute (mL/min). A low eGFR score means reduced kidney function, especially if the value is below 60 mL/min.
When your kidneys fail and no longer work well enough to keep you alive, you have end-stage kidney disease. End-stage kidney disease happens when eGFR is consistently less than 15 mL/min.
As a part of learning your kidney disease stage, a healthcare professional also might test whether you have protein in your urine. Constant loss of protein in the urine is also a sign of kidney damage, even if your kidney function and eGFR are in the healthy to mild range.
| Kidney disease stage |
GFR, mL/min |
Kidney function |
| Source: National Kidney Foundation |
| Stage 1 |
90 or above |
Healthy kidney function |
| Stage 2 |
60 to 89 |
Mild loss of kidney function |
| Stage 3a |
45 to 59 |
Mild to moderate loss of kidney function |
| Stage 3b |
30 to 44 |
Moderate to severe loss of kidney function |
| Stage 4 |
15 to 29 |
Severe loss of kidney function |
| Stage 5 |
Less than 15 |
Kidney failure |
Treatment
Start your donor evaluation
Begin the process of becoming a living kidney or liver donor by clicking here to complete a health history questionnaire.
End-stage kidney disease treatments include:
- Kidney transplant.
- Dialysis.
- Supportive care, also called palliative care.
Kidney transplant
Kidney transplant
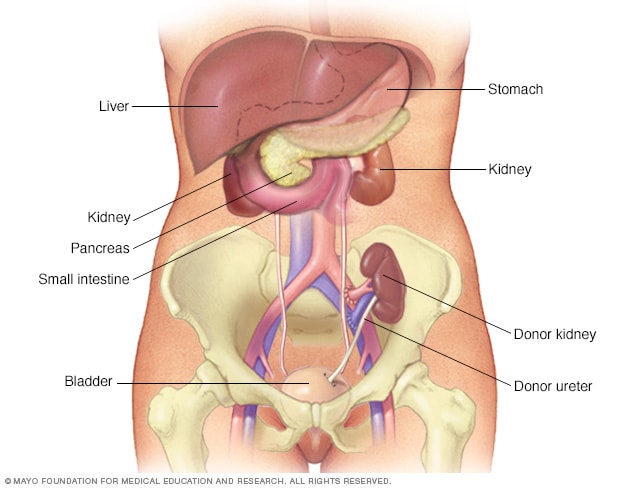
Kidney transplant
During kidney transplant surgery, the donor kidney is placed in your lower belly. Blood vessels of the new kidney are attached to blood vessels in the lower part of your abdomen, just above one of your legs. The new kidney's urine tube, called a ureter, is connected to your bladder. Unless your own kidneys are causing complications, they are left in place.
A kidney transplant is a surgical procedure. A healthy kidney from a donor is placed into a person whose kidneys no longer work well. A kidney transplant often is the treatment of choice for end-stage kidney disease. Without a transplant, lifetime dialysis is needed.
The kidney transplant process takes time. It involves finding a donor, living or deceased, whose kidney best matches your own. You then have surgery. During surgery, the new kidney is placed in your lower belly. To allow the new kidney to function, a surgeon attaches the kidney's blood vessels and the tube that links the kidney to the bladder. This tube is called the ureter.
You may need to spend up to a week in the hospital. After leaving the hospital, you likely will have regular checkups to review your progress as you recover. You may take a number of medicines to help keep your immune system from rejecting the new kidney. These medicines also can lower the risk of complications after surgery, such as infection.
After a successful kidney transplant, the new kidney filters the blood. You no longer need dialysis.
Dialysis
Dialysis does some of the work of your kidneys when your kidneys can't do it themselves. This includes removing extra fluids and waste products from your blood, restoring electrolyte levels, and helping control your blood pressure.
Dialysis options include peritoneal dialysis and hemodialysis.
Peritoneal dialysis
During peritoneal dialysis, blood vessels in the stomach lining fill in for the kidneys. A fluid washes in and out of the peritoneal space and helps the vessels filter extra fluids and waste. Peritoneal dialysis is done at home.
This name refers to the lining that surrounds the organs in your abdomen. That lining is called the peritoneal membrane. It forms a space that can hold fluid. With peritoneal dialysis, a permanent catheter is inserted through the lining into the space around your organs. Dialysis solution is drained through the catheter into that space. The peritoneal lining contains many blood vessels. The solution draws extra fluid, chemicals, and waste out of those blood vessels and through the lining. The lining acts as a filter. The solution is left in place for a number of hours while dialysis occurs. Then it's allowed to drain out through the catheter. New, clean solution is immediately drained in, filling up the space again. This process of exchanging old solution with new is called an exchange.
Hemodialysis
During hemodialysis, a machine does some of the work of the kidneys. It filters extra fluids and wastes from the blood. Hemodialysis may be done at a dialysis center or at home.
Your blood is run through a filter that acts as an artificial kidney. The filter removes the extra fluid, chemicals, and waste from your blood. The cleaned blood is then pumped back into your body. Two needles are inserted for every treatment. The place they are inserted is called the access. A surgeon may connect two of your blood vessels to create an access. This is called a fistula. Connecting the vessels causes the vein to get larger and stronger. The dialysis needles are inserted into that vein.
Another option is to connect a plastic tube between two blood vessels. This is called a graft. The needles are inserted into this artificial vein. In urgent situations, a tube, called a catheter, may be placed temporarily into a large vein in your neck. The tube has two branches, one to carry blood out of the body and the other to return it. Your physician will make a recommendation based on the condition of your veins and other considerations.
For dialysis to be successful, lifestyle changes may be needed. For instance, you need to follow a certain diet.
Palliative care
If you choose not to have a kidney transplant or dialysis, you can choose supportive care, also called palliative care. This can help you manage your symptoms so that you feel better. You also can combine palliative care with kidney transplant or dialysis.
Without either dialysis or a transplant, end-stage kidney disease gets worse. Death could happen quickly or take several months, even years. Palliative care might include treating symptoms, measures to keep you comfortable and end-of-life planning.
More Information
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
Following a special diet is an important part of kidney disease treatment. This includes finding ways to lower how much sodium you take in. Careful choices about what you eat and drink can limit how hard the kidneys have to work. Ask for a referral to a registered dietitian who specializes in working with people who have kidney disease, called a renal dietitian. A renal dietitian can study your diet and suggest food and drink choices you can make to help your kidneys work less hard.
For example, a renal dietitian might work with you to:
- Avoid products with added salt. Lower the amount of sodium you eat by staying away from salty snack foods and other foods with added salt. These include many ready-made foods, such as frozen dinners and canned soups and vegetables. Processed meats and cheeses also tend to be high in salt.
- Choose foods lower in potassium. Your dietitian might suggest that you choose lower potassium foods at each meal. High-potassium foods include bananas, oranges, potatoes, spinach and tomatoes. Examples of low-potassium foods include apples, cabbage, carrots, green beans, grapes and strawberries. Many salt substitutes have potassium, so you may want to avoid them if you have kidney failure.
- Limit protein. Your dietitian can estimate how many grams of protein you need each day. Based on that amount, your dietitian can make suggestions on what to eat. High-protein foods include lean meats, eggs, milk, cheese and beans. Low-protein foods include vegetables, fruits, breads and cereals.
Coping and support
Learning that you have end-stage kidney disease can come as a shock, even if you've been living with chronic kidney disease for some time. It also can be hard to manage the treatment schedule if you're on dialysis.
If you're feeling overwhelmed by your diagnosis, it might help to:
- Connect with other people who have kidney disease. People who are going through the same thing as you can understand what you're feeling. They also can offer unique support. Ask your doctor or other healthcare professional about support groups in your area. Or contact the American Association of Kidney Patients, the National Kidney Foundation or the American Kidney Fund. These organizations can help connect you with groups in your area.
- Stick to your routine as much as possible. Try to keep doing the things you enjoy. Continue working if your condition allows.
- Be active most days of the week. If your healthcare team says it's OK, keep up your activity level. Aim for at least 30 minutes of physical activity most days of the week. This can help with fatigue and stress.
- Talk with someone you trust. You might have a friend or family member who is a good listener. Or you may find it helpful to talk with a faith leader or someone else you trust. Ask your doctor or other healthcare professional for a referral to a social worker or counselor.
Preparing for your appointment
For end-stage kidney disease, you'll likely keep seeing the same healthcare team you've been seeing for treatment of chronic kidney disease. If you're not already being cared for by a nephrologist, you might be referred to one. A nephrologist is a doctor who specializes in kidney conditions.
What you can do
Before your appointment, it's a good idea to:
- Be aware of any restrictions. When you make the appointment, ask if there's anything you need to do in advance, such as change your diet, so that you're ready for any tests you may need.
- Write down any symptoms you have, including any that may seem unrelated to your kidneys or urinary function, and when they started.
- Write down key personal information, including any major stresses or recent life changes.
- Make a list of all medicines, vitamins or supplements you take and how much you take.
- Consider bringing a family member or friend along. It can be hard to remember all the information you get during an appointment. Someone who comes with you may remember things that you missed or forgot.
- Write down questions to ask your healthcare team.
For end-stage kidney disease, some basic questions to ask include:
- What's the level of damage to my kidneys?
- Is my kidney function getting worse?
- Do I need more tests?
- What's causing my condition?
- What are my treatment options?
- What are the possible side effects of each treatment?
- I have these other health conditions. How can I best manage them together?
- Do I need to eat a special diet?
- Can you refer me to a dietitian who can help me plan my meals?
- How often do I need to have my kidney function tested?
- Where can I find more information?
Don't hesitate to ask any other questions you have.
What to expect from your doctor
Your doctor or other healthcare professional may ask you questions, such as:
- How have your symptoms changed over time?
- Have you noticed changes in your urinary habits?
- Have you felt a lot more tired lately?
- Have you been diagnosed or treated for high blood pressure?