Diagnosis
Finding the cause of interstitial lung disease can be challenging, and sometimes the cause can't be found. Many conditions fall into the category of ILD. In addition, the symptoms of a wide range of medical conditions can appear to be ILD. Healthcare professionals must rule out these conditions before making a diagnosis.
Some of the following tests may be necessary.
Lab tests
- Blood tests. Certain bloodwork can detect proteins, antibodies and other markers of autoimmune diseases or inflammatory responses to environmental exposures, such as those caused by molds or bird protein.
Imaging tests
- Computerized tomography, also called a CT scan. This imaging test is key to the diagnosis of interstitial lung disease. It's sometimes the first test in the diagnosis. CT scanners produce 3D images of internal structures. A high-resolution CT scan can be especially helpful in figuring out how much lung damage there is. It can show details of the fibrosis, which can help narrow the diagnosis and guide treatment decisions.
- Echocardiogram. An echocardiogram uses sound waves to visualize the heart. It can create still images of your heart's structures and videos that show how your heart is working. This test can measure the amount of pressure in the right side of your heart.
Pulmonary function tests
Spirometer
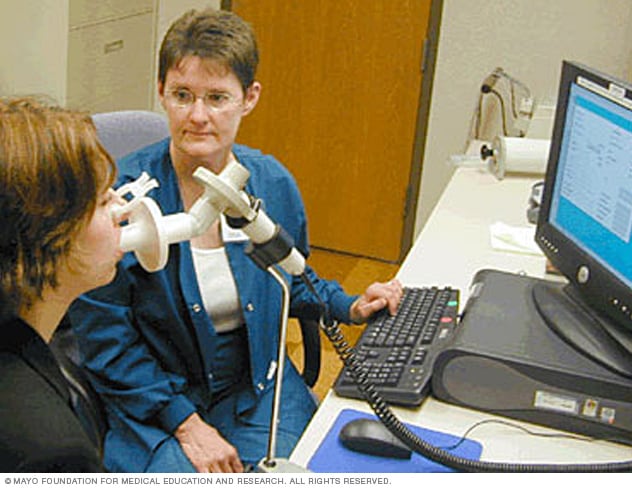
Spirometer
A spirometer is a diagnostic device that measures the amount of air you can breathe in and out and the time it takes you to breathe out completely after you take a deep breath.
- Spirometry and diffusion capacity. This test requires you to breathe out quickly and forcefully through a tube connected to a machine. The machine measures how much air your lungs can hold and how quickly you can move air out of your lungs. It also measures how easily oxygen can move from your lungs into your bloodstream.
- Oximetry. A small device is placed on one of your fingers to measure the oxygen level in your blood. This test may be done at rest or with activity to monitor the course of the lung disease and figure out how serious it is.
Lung tissue analysis
Sometimes interstitial lung diseases can be diagnosed only by looking at a small amount of lung tissue in a lab — what's known as a biopsy.
Your doctor or other healthcare professional may take a tissue sample using one of these methods:
- Bronchoscopy. In this procedure, your healthcare professional removes very small tissue samples — generally no larger than the head of a pin. This is done by using a small, flexible tube, also known as a bronchoscope, that's passed through your mouth or nose into your lungs. The risks of bronchoscopy are generally minor, namely a sore throat for a limited time and hoarseness from the bronchoscope. But the tissue samples are sometimes too small to make a diagnosis.
- Bronchoalveolar lavage. In this procedure, your doctor injects about a tablespoon of sterile salt water through a bronchoscope into a section of your lung and then suctions it out right away. The solution that's removed contains cells from your air sacs. Although bronchoalveolar lavage samples a larger area of the lung than other procedures do, it may not give enough information to find out what's causing pulmonary fibrosis.
- Surgical biopsy. Although this is a more invasive procedure with potential complications, it's often the only way to get a large enough tissue sample to make the correct diagnosis. General anesthesia is used for this test. Surgical instruments and a small camera are inserted through one or more small incisions between the ribs. The camera allows a surgeon to view the lungs on a video monitor while removing tissue samples from the lungs.
More Information
Treatment
Lung scarring that already has occurred in interstitial lung disease can't be reversed, and treatment won't always stop the disease from getting worse. Some treatments may make symptoms better for a short time or slow the disease. Others help maintain quality of life.
Because many of the different types of scarring diseases have no approved or proven therapies, clinical trials may be an option to get an experimental treatment.
Medications
Intense research to find treatment options for specific types of interstitial lung disease is ongoing. Treatment may vary depending on the cause of ILD and what damage has happened in the lungs. Using on the latest scientific evidence, your healthcare professional may recommend:
- Corticosteroid medicines. At first, many people diagnosed with ILD are treated with a corticosteroid, namely prednisone (Prednisone Intensol, Rayos). Sometimes people are treated with other drugs that suppress the immune system. Depending on the cause of ILD, these medicines may slow or even keep the disease from getting worse.
- Medicines that slow the worsening of idiopathic pulmonary fibrosis. Pirfenidone (Esbriet) and nintedanib (Ofev) are medicines that may slow the rate at which IPF worsens. Ofev also has been approved for people with lung fibrosis that's getting worse due to other types of interstitial lung disease. Side effects for both drugs are common. Talk with your healthcare professional about the pros and cons of these medicines.
- Medicines that reduce stomach acid. Gastroesophageal reflux disease, also known as GERD, affects most people with idiopathic pulmonary fibrosis. GERD is linked to worse lung damage. If you have symptoms of acid reflux, your healthcare professional may prescribe ways to treat GERD that reduce stomach acid.
Oxygen therapy
Using oxygen can't stop lung damage, but it can:
- Make it easier to breathe and exercise.
- Prevent or lessen complications from low blood oxygen levels.
- Lower blood pressure in the right side of your heart.
- Make your sleep and sense of well-being better.
You're most likely to get oxygen when you sleep or exercise, although some people may use it around the clock.
Pulmonary rehabilitation
The aim of pulmonary rehabilitation is to make you better able to function and live a full, satisfying life. That's why pulmonary rehabilitation programs focus on:
- Learning more about your lung disease.
- Exercise, so you can become more physically active for longer periods of time.
- Breathing techniques that make your lungs more efficient.
- Emotional support.
- Nutritional counseling.
Surgery
A lung transplant may be an option of last resort for some people with severe interstitial lung disease when other treatment options haven't helped.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
You must be actively involved in your own treatment and stay as healthy as possible when you're living with interstitial lung disease. For that reason, it's important to:
- Learn about your disease. Understanding your condition and how it can be treated can help you decide about your care. Including family members and friends can help them learn your needs.
- Stop smoking. If you have lung disease, the best thing you can do for yourself is to stop smoking. Talk with your healthcare professional about options for quitting, including programs to help you stop smoking. These programs use various proven techniques to help people quit. And because secondhand smoke also can harm your lungs, don't allow people to smoke around you.
- Avoid exposure at work or during hobbies. When possible, stay away from substances that can irritate your lungs. Ask your healthcare professional for more information and advice.
- Eat well. If you have lung disease, you may lose weight because it isn't comfortable to eat and because of the extra energy it takes to breathe. Aim to eat a nutritionally rich diet that contains enough calories. A dietitian can give you more guidelines for healthy eating.
- Get vaccinated. Respiratory infections can make symptoms of ILD worse. Make sure you get the pneumonia vaccine and a flu shot each year.
Coping and support
Living with a chronic lung disease is emotionally and physically challenging. You may need to change your daily routines and activities — sometimes a lot — as breathing problems worsen or health care needs become more important. Feelings of fear, anger and sadness are typical as you grieve for the loss of your old lifestyle and worry about what's next for you and your family.
Share your feelings with your loved ones and your healthcare professional. Talking openly may help you and your loved ones cope with the emotional challenges of your disease. Also, clear communication can help you and your family plan for your needs if your disease gets worse.
Think about joining a support group, where you can talk with people who are facing challenges like yours. Group members may share coping strategies, exchange information about new treatments or simply listen as you express your feelings. If a group isn't for you, you may want to talk with a counselor in a one-on-one setting.
Preparing for your appointment
You'll probably first see your family healthcare professional about your symptoms. Your family healthcare professional may refer you to a pulmonologist, who is a doctor who specializes in lung diseases.
What you can do
Before your appointment, you might want to prepare answers to these questions:
- What are your symptoms and when did they start?
- Are you being treated for other medical conditions?
- What medicines and supplements have you taken in the past five years, including medicines available without a prescription and street drugs?
- What are all the occupations you've had, even if only for a few months?
- Do any members of your family have a lasting lung disease of any kind?
- Have you ever had chemotherapy or radiation treatments for cancer?
Let your pulmonologist know if you've had any chest X-rays, CT scans or other tests so the healthcare professional can request the results before your visit. The images are more important than the report alone. The pulmonologist can make a diagnosis by comparing an old imaging test with those of a current test.
What to expect from your doctor
Your doctor or other healthcare professional may ask some of these questions:
- Do your symptoms occur all of the time or do they seem to go away and then come back?
- Have you recently had contact with air conditioners, humidifiers, pools, hot tubs, or water-damaged walls or carpet?
- Do you own any pet birds or feather-containing items such as down pillows or comforters?
- Are you exposed to mold or construction dust in your home or other places where you spend a lot of time?
- Have any close relatives, friends or co-workers been diagnosed with a lung condition?
- Do you have any family history of lung disease?
- Does your work history include regularly working with or being around toxins and pollutants, such as asbestos, silica dust or grain dust?
- Do you or did you smoke? If so, how much and for how long? If not, have you spent a lot of time around others who smoke?
- Have you been diagnosed or treated for any other medical conditions, particularly arthritis or rheumatic diseases?
- Do you have symptoms of gastroesophageal reflux disease, also known as GERD, such as heartburn?
Nov. 23, 2024