Diagnosis
A healthcare professional might be able to see external hemorrhoids. Diagnosing internal hemorrhoids might include an exam of your anal canal and rectum.
- Digital exam. A healthcare professional places a gloved, lubricated finger into your rectum. This allows your health professional to check for anything that's not usual, such as growths.
- Visual exam. Internal hemorrhoids are often too soft for a healthcare professional to feel during a rectal exam. The health professional might look at the lower part of your colon and rectum with a tool such as an anoscope, a proctoscope or a sigmoidoscope.
A healthcare professional might want to look at your entire colon using colonoscopy if:
- Your symptoms suggest that you might have another digestive system disease.
- You have risk factors for colorectal cancer.
- You are middle-aged and haven't had a recent colonoscopy.
Treatment
Home remedies
You can often lessen the mild pain, swelling and inflammation of hemorrhoids with home treatments.
- Eat high-fiber foods. Eat more foods that are high in fiber. This helps soften the stool and increases its bulk, which can help you avoid straining. Add fiber to your diet slowly to avoid problems with gas.
- Use topical treatments. Apply a hemorrhoid cream or suppository containing hydrocortisone that you can buy without a prescription. You also can use pads containing witch hazel or a numbing medicine.
- Soak regularly in a warm bath or sitz bath. Soak your anal area in plain warm water for 10 to 15 minutes two or three times a day. A sitz bath fits over the toilet.
- Take pain relievers by mouth. You can temporarily use acetaminophen (Tylenol, others), aspirin or ibuprofen (Advil, Motrin IB, others) to help ease your discomfort.
With these treatments, hemorrhoid symptoms often go away within a week. See a healthcare professional if you don't get relief after a week of home care. Contact a health professional sooner if you have severe pain or bleeding.
Medicines
Your hemorrhoids might only produce mild discomfort. In this case, a healthcare professional may suggest creams, ointments, suppositories or pads that you can buy without a prescription. These products contain ingredients such as witch hazel or hydrocortisone and lidocaine, which can temporarily relieve pain and itching.
Hydrocortisone is a steroid that can thin your skin when used for more than a week. Ask your health professional how long you should use it.
External hemorrhoid thrombectomy
If a painful blood clot has formed within an external hemorrhoid, a healthcare professional can remove the hemorrhoid. Removal can provide relief right away. This procedure is done with a medicine that numbs a part of the body, called a local anesthetic. Thrombectomy works best when done within 72 hours of getting a clot.
Minimally invasive procedures
Rubber band ligation of hemorrhoid
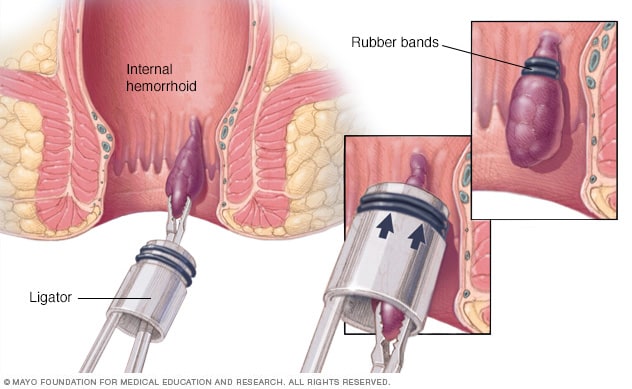
Rubber band ligation of hemorrhoid
To remove a hemorrhoid using rubber band ligation, a healthcare professional uses a small tool called a ligator. The health professional passes the tool through a lighted tube, called a scope, into the anal canal and grasps the hemorrhoid with forceps. Sliding the ligator cylinder upward releases rubber bands around the base of the hemorrhoid. Rubber bands cut off the hemorrhoid's blood supply, causing the hemorrhoid to wither and drop off.
For bleeding that doesn't stop or for painful hemorrhoids, a healthcare professional might recommend a minimally invasive procedure. These treatments can be done in a medical office or another outpatient setting. They don't usually require numbing medicine.
-
Rubber band ligation. A healthcare professional places one or two tiny rubber bands around the base of an internal hemorrhoid to cut off its blood flow. The hemorrhoid withers and falls off within a week.
Hemorrhoid banding can be uncomfortable and cause bleeding. The bleeding might begin 2 to 4 days after the procedure but is rarely severe. Sometimes, more-serious complications can occur.
- Sclerotherapy. With sclerotherapy, a health professional injects a chemical solution into the hemorrhoid tissue to shrink it. While the injection causes little or no pain, it might be less effective than rubber band ligation.
- Coagulation. Coagulation techniques use laser or infrared light or heat. They cause small, bleeding internal hemorrhoids to harden and shrivel. Coagulation has few side effects and usually causes little discomfort.
Surgical procedures
Only a small percentage of people with hemorrhoids need surgery to remove them. However, if other procedures haven't worked or you have large hemorrhoids, a healthcare professional might recommend one of the following:
-
Hemorrhoid removal, also called hemorrhoidectomy. Your surgeon removes extra tissue that causes bleeding by using one of various techniques. The surgery can be done with a local anesthetic combined with a medicine to help you feel calm or less anxious, also called a sedative. Spinal anesthesia or general anesthesia also may be used.
Hemorrhoidectomy is the most effective and complete way to treat severe or recurring hemorrhoids. Complications can include having a hard time urinating, which can lead to urinary tract infections. This complication is short-term and happens mainly after spinal anesthesia.
Most people have some pain after the procedure. Medicines can ease this pain. Soaking in a warm bath also might help.
-
Hemorrhoid stapling. This procedure, called stapled hemorrhoidopexy, blocks blood flow to hemorrhoidal tissue. It is typically used only for internal hemorrhoids.
Stapling generally involves less pain than hemorrhoidectomy and lets you get back to regular activities sooner. Compared with hemorrhoidectomy, however, stapling has been linked to a greater risk of hemorrhoids coming back and rectal prolapse. Rectal prolapse happens when part of the rectum pushes through the anus.
Complications also can include pain, bleeding and trouble emptying the bladder. A rare complication is a life-threatening blood infection called sepsis.
Talk with a healthcare professional about the best option for you.
Preparing for your appointment
If you have symptoms of hemorrhoids, make an appointment with someone on your primary healthcare team. If needed, this person might refer you to one or more specialists for evaluation and treatment. These specialists may include a doctor with expertise in the digestive system, called a gastroenterologist, and a colon and rectal surgeon.
Here are some suggestions to help you get ready for your appointment.
What you can do
Be aware of any restrictions before your appointment. When you make the appointment, ask if there's anything you need to do in advance.
Make a list of:
- Your symptoms and how long you've noticed them.
- Key personal information, including typical bowel habits and diet, especially your fiber intake.
- All medicines, vitamins and supplements you take, including doses.
- Questions to ask during your appointment.
For hemorrhoids, some questions to ask include:
- What's the likely cause of my symptoms?
- Is my condition likely to be short term or lasting?
- Am I at risk of complications related to this condition?
- What treatment approach do you recommend?
- If treatments we try first don't work, what will you recommend next?
- Am I a candidate for surgery? Why or why not?
- Are there more self-care steps that might help?
- I have other medical conditions. How can I manage these along with hemorrhoids?
Don't hesitate to ask other questions.
What to expect from your doctor
Your health professional is likely to ask a few questions, including:
- How uncomfortable are your symptoms?
- What are your typical bowel habits?
- How much fiber does your diet contain?
- What, if anything, seems to make your symptoms better?
- What, if anything, appears to worsen your symptoms?
- Has anyone in your family had hemorrhoids or cancer of the colon, rectum or anus?
- Have you had a change in your bowel habits?
- When passing stool, have you noticed blood on your toilet paper, dripping into the toilet or mixed into your stools?
What you can do in the meantime
Before your appointment, take steps to soften your stools. Eat more high-fiber foods, such as fruits, vegetables and whole grains. Consider a nonprescription fiber supplement, such as psyllium or methylcellulose. Drinking 6 to 8 glasses of water a day also might help ease your symptoms.
Aug. 23, 2025