Overview
Celiac disease
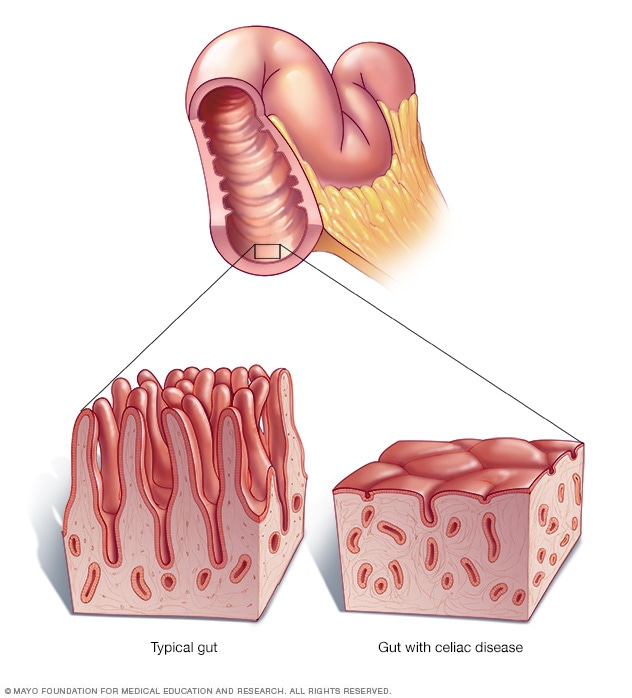
Celiac disease
Your small intestine is lined with tiny hairlike projections called villi, which absorb sugars, fats, proteins, vitamins, minerals and other nutrients from the food you eat. Gluten exposure in people with celiac disease damages the villi, making it hard for the body to absorb nutrients necessary for health and growth.
Celiac disease is an autoimmune condition where the immune system reacts to gluten, sometimes causing damage to the small intestine. Gluten is a protein found in foods containing wheat, barley or rye.
If you have celiac disease, eating gluten triggers an immune response to the gluten protein in your small intestine. Over time, this reaction can damage your small intestine's lining and prevent it from absorbing nutrients. This condition is called malabsorption.
The intestinal damage often causes symptoms such as diarrhea, fatigue, weight loss, bloating or anemia. It also can lead to serious complications if it is not managed or treated. In children, malabsorption can affect growth and development in addition to gastrointestinal symptoms.
There's no definite cure for celiac disease. But for most people, following a strict gluten-free diet can help manage symptoms and help the intestines heal.
Symptoms
The symptoms of celiac disease can vary greatly. They also may be different in children and adults. Digestive symptoms for adults include:
- Diarrhea.
- Fatigue.
- Weight loss.
- Bloating and gas.
- Belly pain.
- Nausea and vomiting.
- Constipation.
However, more than half the adults with celiac disease have symptoms that are not related to the digestive system, including:
- Anemia, usually from iron deficiency due to decreased iron absorption.
- Loss of bone density, called osteoporosis, or softening of bones, called osteomalacia.
- Itchy, blistery skin rash, called dermatitis herpetiformis.
- Mouth ulcers.
- Headaches and fatigue.
- Nervous system injury, including numbness and tingling in the feet and hands, possible problems with balance, and cognitive impairment.
- Joint pain.
- Reduced functioning of the spleen, known as hyposplenism.
- Elevated liver enzymes.
Children
Children with celiac disease are more likely than adults to have digestive problems, including:
- Nausea and vomiting.
- Chronic diarrhea.
- Swollen belly.
- Constipation.
- Gas.
- Pale, foul-smelling stools.
Not being able to absorb nutrients may cause:
- Failure to thrive for infants.
- Damage to tooth enamel.
- Weight loss.
- Anemia.
- Irritability.
- Short stature.
- Delayed puberty.
- Neurological symptoms, including attention-deficit/hyperactivity disorder (ADHD), learning disabilities, headaches, lack of muscle coordination and seizures.
Dermatitis herpetiformis
Gluten intolerance can cause this blistery skin disease. The rash usually happens on the elbows, knees, torso, scalp or buttocks. Like celiac disease, this condition is often associated with changes to the lining of the small intestine. However, dermatitis herpetiformis might not cause digestive symptoms.
Healthcare professionals treat dermatitis herpetiformis with a gluten-free diet or medicine, or both, to control the rash.
When to see a doctor
Consult your healthcare team if you have diarrhea or digestive discomfort that lasts for more than two weeks. Consult your child's healthcare team if your child:
- Is pale.
- Is irritable.
- Is failing to grow.
- Has a potbelly.
- Has foul-smelling, bulky stools.
Be sure to consult your healthcare team before trying a gluten-free diet. If you stop or even reduce the amount of gluten you eat before you're tested for celiac disease, you can change the test results.
Celiac disease tends to run in families. If someone in your family has the condition, ask a member of your healthcare team if you should be tested. Also ask about testing if you or someone in your family has a risk factor for celiac disease, such as type 1 diabetes.
Causes
A person's genes, combined with eating foods with gluten and other factors, can contribute to celiac disease. However, the precise cause isn't known. Infant-feeding practices, gastrointestinal infections and gut bacteria may contribute, but these causes have not been proved. Sometimes celiac disease becomes active after surgery, pregnancy, childbirth, viral infection or severe emotional stress.
When the body's immune system overreacts to gluten in food, the reaction damages the tiny, hairlike projections, called villi, that line the small intestine. Villi absorb vitamins, minerals and other nutrients from the food you eat. If your villi are damaged, you can't get enough nutrients, no matter how much you eat.
Risk factors
Celiac disease tends to be more common in people who have:
- A family member with celiac disease or dermatitis herpetiformis.
- Type 1 diabetes.
- Down syndrome, Williams syndrome or Turner syndrome.
- Autoimmune thyroid disease.
- Microscopic colitis.
- Addison's disease.
Complications
Celiac disease that is not treated can lead to:
- Malnutrition. This happens if your small intestine can't absorb enough nutrients. Malnutrition can lead to anemia and weight loss. In children, malnutrition can cause slow growth and short stature.
- Bone weakening. In children, malabsorption of calcium and vitamin D can lead to a softening of the bone, called osteomalacia or rickets. In adults, it can lead to a loss of bone density, called osteopenia or osteoporosis.
- Infertility and miscarriage. Not being able to absorb calcium and vitamin D properly can contribute to reproductive issues.
- Lactose intolerance. Damage to your small intestine might cause you belly pain and diarrhea after eating or drinking dairy products that contain lactose. Once your intestine has healed, you might be able to tolerate dairy products again.
- Cancer. People with celiac disease who don't maintain a gluten-free diet have a greater risk of developing several forms of cancer, including intestinal lymphoma and small bowel cancer.
- Nervous system conditions. Some people with celiac disease can develop conditions such as seizures or a disease of the nerves to the hands and feet, called peripheral neuropathy.
Nonresponsive celiac disease
Some people with celiac disease don't respond to what they consider to be a gluten-free diet. Nonresponsive celiac disease is often due to contamination of the diet with gluten. Working with a dietitian can help you learn how to avoid all gluten.
People with nonresponsive celiac disease might have:
- Bacterial overgrowth in the small intestine.
- Microscopic colitis.
- Poor pancreas function, known as pancreatic insufficiency.
- Irritable bowel syndrome.
- Difficulty digesting sugar found in dairy products (lactose), table sugar (sucrose), or a type of sugar found in honey and fruits (fructose).
- Truly refractory celiac disease that is not responding to a gluten-free diet.
Refractory celiac disease
In rare instances, the intestinal injury of celiac disease doesn't respond to a strict gluten-free diet. This is known as refractory celiac disease. If you still have symptoms after following a gluten-free diet for 6 months to 1 year, you should talk to your healthcare team to see if you need further testing to look for explanations for your symptoms.