Diagnosis
To diagnose carpal tunnel syndrome, your healthcare professional may ask you questions about your symptoms. You also may need one or more tests to find out whether you have carpal tunnel syndrome:
-
History of symptoms. The pattern of your symptoms is important in making a diagnosis. Carpal tunnel syndrome symptoms usually occur while holding a phone or a newspaper or gripping a steering wheel. They also tend to occur at night and may wake you from sleep. Or you may notice the numbness when you wake up in the morning.
But the median nerve doesn't provide sensation to the little finger. If you have symptoms in that finger, you may have a condition other than carpal tunnel syndrome.
-
Physical exam. Your healthcare professional tests the feeling in the fingers and the strength of the muscles in the hand.
Bending the wrist, tapping on the nerve or simply pressing on the nerve can trigger symptoms in many people.
- X-ray. You may need an X-ray of the affected wrist to exclude other causes of wrist pain, such as arthritis or fracture. However, X-rays are not helpful in making a diagnosis of carpal tunnel syndrome.
- Ultrasound. An ultrasound of the wrist provides a picture of the tendons and nerves. This can help show whether the nerve is being compressed.
- Electromyography. This test measures the tiny electrical discharges produced in muscles. During this test, a thin-needle electrode is inserted into specific muscles to evaluate the electrical activity when muscles contract and rest. This test can identify damage to the muscles controlled by the median nerve. The test also may rule out other conditions.
- Nerve conduction study. In a variation of electromyography, two electrodes are taped to the skin. A small shock is passed through the median nerve to see if electrical impulses are slowed in the carpal tunnel. This test may be used to diagnose the condition and rule out other conditions.
Treatment
Treat carpal tunnel syndrome as early as possible after symptoms start. In the early stages, simple things that you can do for yourself may make the symptoms go away. For example:
- Take more-frequent breaks to rest the hands.
- Don't do activities that make symptoms worse.
- Use cold packs to reduce swelling.
Other treatment options include wrist splinting, medicines and surgery. Splinting and other conservative treatments are more likely to help if you've had only mild to moderate symptoms that come and go for less than 10 months.
If you have numbness in your hands, get treatment from a healthcare professional.
Nonsurgical therapy
If the condition is diagnosed early, nonsurgical methods may help improve carpal tunnel syndrome, including:
- Wrist splinting. A splint that holds the wrist still while you sleep can help relieve nighttime symptoms of tingling and numbness. Even though you only wear the splint at night, it also can help prevent daytime symptoms. Nighttime splinting may be a good option if you're pregnant because it does not involve the use of any medicines to be effective.
-
Nonsteroidal anti-inflammatory drugs (NSAIDs). NSAIDs, such as ibuprofen (Advil, Motrin IB, others), may help relieve pain from carpal tunnel syndrome in the short term.
There isn't evidence, however, that these medicines improve carpal tunnel syndrome.
-
Corticosteroids. Your healthcare professional may inject the carpal tunnel with a corticosteroid medicine such as cortisone to relieve pain. Sometimes an ultrasound is used to guide these injections.
Corticosteroids decrease inflammation and swelling, which relieves pressure on the median nerve. Oral corticosteroids aren't considered as effective as corticosteroid injections for treating carpal tunnel syndrome.
If carpal tunnel syndrome is caused by rheumatoid arthritis or another inflammatory arthritis, then treating the arthritis may reduce symptoms of carpal tunnel syndrome. However, this has not been proved by research.
Surgery
Carpal tunnel release
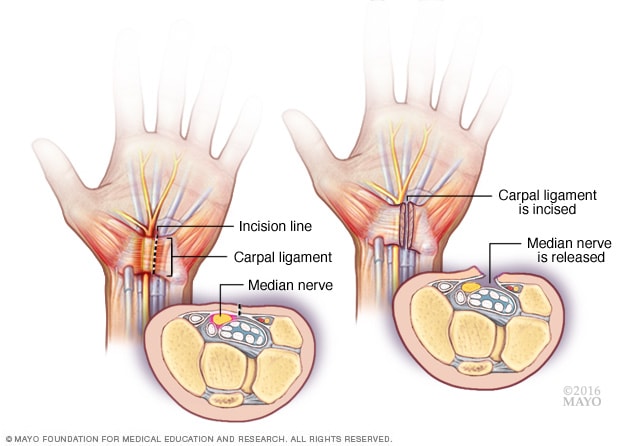
Carpal tunnel release
During carpal tunnel release, a surgeon makes an incision in the palm of the hand over the carpal tunnel ligament and cuts through the ligament to relieve pressure on the median nerve. The surgery may be done by making one incision on the palm side of the wrist or by making several small incisions.
Surgery may be appropriate if symptoms are severe or don't respond to other treatments.
The goal of carpal tunnel surgery is to relieve pressure by cutting the ligament pressing on the median nerve.
Three different techniques are used in carpal tunnel surgery:
-
Endoscopic surgery. A surgeon uses a telescope-like device with a tiny camera called an endoscope. This allows the surgeon to see inside the carpal tunnel. The surgeon cuts the ligament through one or two small incisions in the hand or wrist.
Endoscopic surgery may result in less pain than does open surgery in the first few days or weeks after surgery.
- Open surgery. A surgeon makes a cut, also called an incision, in the palm of the hand over the carpal tunnel and cuts through the ligament to free the nerve.
- Ultrasound-guided surgery. This surgery is similar to endoscopic surgery, but the surgeon uses ultrasound to see the nerve, tendons, arteries and ligament. Then the surgeon cuts the ligament either with a small knife or with a braided wire put into the wrist through a needle.
Discuss the risks and benefits of each technique with your surgeon before surgery. Surgery risks may include:
- Incomplete release of the ligament.
- Wound infections.
- Scar formation.
- Injuries to nerves or blood vessels.
During the healing process after the surgery, the ligament tissues gradually grow back together while allowing more room for the nerve. This internal healing process typically takes several months, but the skin heals in a few weeks.
Your surgeon likely will recommend that you use the hand after the ligament has healed. Slowly work back to full use of the hand and do not use forceful hand motions or extreme wrist positions.
Soreness or weakness may take from several weeks to a few months to resolve after surgery. If your symptoms were very severe, they may not completely go away after surgery.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
These steps may provide temporary symptom relief:
- Take short, frequent breaks from repetitive activities involving the use of the hands.
- Lose weight if you are overweight or obese.
- Rotate the wrists and stretch the palms and fingers.
- Take a pain reliever, such as acetaminophen (Tylenol, others), aspirin, ibuprofen (Advil, Motrin IB, others) or naproxen sodium (Aleve).
- Wear a snug, not tight, wrist splint at night. You can buy these without a prescription at most drugstores or pharmacies.
- Do not sleep on the hands.
If pain, numbness or weakness persists, see your healthcare professional.
Alternative medicine
Alternative therapies in your treatment plan may help you manage carpal tunnel syndrome. You may have to experiment to find a treatment that works for you. Always check with your healthcare professional before trying any complementary or alternative treatment.
- Yoga. Yoga postures designed for strengthening, stretching and balancing the upper body and joints may help reduce pain and improve grip strength.
- Hand therapy. Early research suggests that certain physical and occupational hand therapy techniques may reduce symptoms of carpal tunnel syndrome.
Preparing for your appointment
Here's some information to help you get ready for your appointment and what to expect from your healthcare professional.
What you can do
- Take note of when your symptoms are at their worst. Does any activity seem to make them worse, or do you notice them at a certain time of day?
- Keep track of the things you've tried to do to make the symptoms better.
- Write down the medicines you've taken to manage your symptoms.
What to expect from your doctor
Your healthcare professional may ask:
- How long have you had the problem?
- Did it come on suddenly or develop over time?
- Is it getting better, getting worse or staying the same?
- Are there certain activities that seem to cause it, make it worse or make it better?
What you can do in the meantime
There are some simple things you can do before you see a healthcare professional for the first time.
First, try to learn whether any activities seem to make your symptoms worse. Change how you do those activities or don't do them, if possible. For example, if driving seems to cause symptoms, try changing the position of your hands on the steering wheel.
You also might try using a wrist splint at night to see if that helps the symptoms.
Feb. 06, 2024