Overview
Bronchioles and alveoli in the lungs
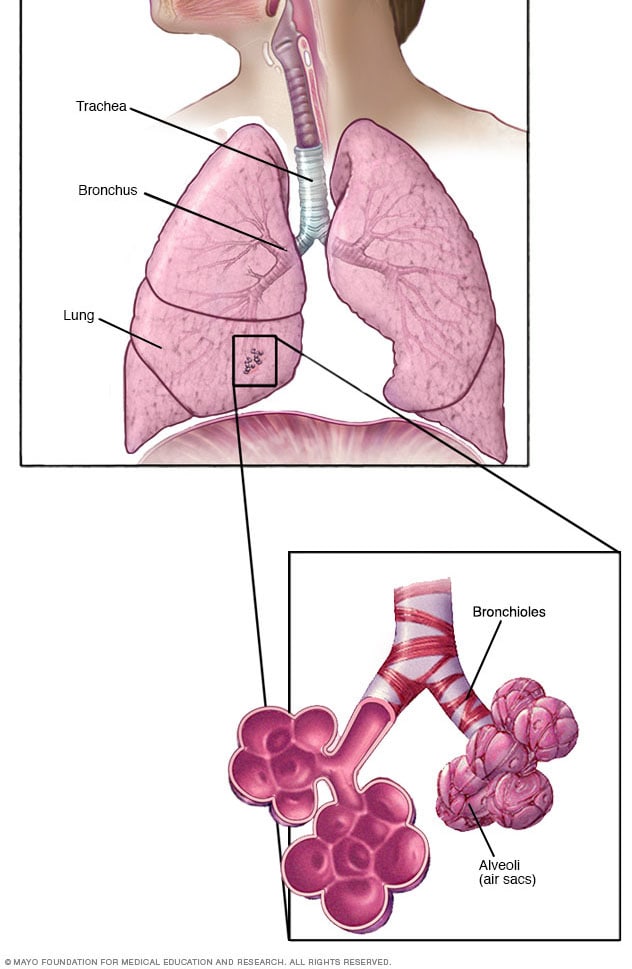
Bronchioles and alveoli in the lungs
In your lungs, the main airways, called bronchi, branch off into smaller and smaller passageways. The smallest airways, called bronchioles, lead to tiny air sacs called alveoli.
Bronchiolitis is a common lung infection in young children and infants. It causes swelling and irritation and a buildup of mucus in the small airways of the lung. These small airways are called bronchioles. Bronchiolitis is almost always caused by a virus.
Bronchiolitis starts out with symptoms much like a common cold. But then it gets worse, causing coughing and a high-pitched whistling sound when breathing out called wheezing. Sometimes children have trouble breathing. Symptoms of bronchiolitis can last for 1 to 2 weeks but occasionally can last longer.
Most children get better with care at home. A small number of children need a stay in the hospital.
Products & Services
Symptoms
For the first few days, the symptoms of bronchiolitis are much like a cold:
- Runny nose.
- Stuffy nose.
- Cough.
- Sometimes a slight fever.
Later, your child may have a week or more of working harder than usual to breathe, which may include wheezing.
Many infants with bronchiolitis also have an ear infection called otitis media.
When to see a doctor
If symptoms become serious, call your child's health care provider. This is especially important if your child is younger than 12 weeks old or has other risk factors for bronchiolitis — for example, being born too early, also called premature, or having a heart condition.
Get medical attention right away if your child has any of these symptoms:
- Has blue or gray skin, lips and fingernails due to low oxygen levels.
- Struggles to breathe and can't speak or cry.
- Refuses to drink enough, or breathes too fast to eat or drink.
- Breathes very fast — in infants this can be more than 60 breaths a minute — with short, shallow breaths.
- Can't breathe easily and the ribs seem to suck inward when breathing in.
- Makes wheezing sounds when breathing.
- Makes grunting noises with each breath.
- Appears slow moving, weak or very tired.
Causes
Bronchiolitis happens when a virus infects the bronchioles, which are the smallest airways in the lungs. The infection makes the bronchioles swollen and irritated. Mucus collects in these airways, which makes it difficult for air to flow freely in and out of the lungs.
Bronchiolitis is usually caused by the respiratory syncytial virus (RSV). RSV is a common virus that infects just about every child by 2 years of age. Outbreaks of RSV infection often happen during the colder months of the year in some locations or the rainy season in others. A person can get it more than once. Bronchiolitis also can be caused by other viruses, including those that cause the flu or the common cold.
The viruses that cause bronchiolitis are easily spread. You can get them through droplets in the air when someone who is sick coughs, sneezes or talks. You also can get them by touching shared items — such as dishes, doorknobs, towels or toys — and then touching your eyes, nose or mouth.
Risk factors
Bronchiolitis usually affects children under the age of 2 years. Infants younger than 3 months have the highest risk of getting bronchiolitis because their lungs and their ability to fight infections aren't yet fully developed. Rarely, adults can get bronchiolitis.
Other factors that increase the risk of bronchiolitis in infants and young children include:
- Being born too early.
- Having a heart or lung condition.
- Having a weakened immune system. This makes it hard to fight infections.
- Being around tobacco smoke.
- Contact with lots of other children, such as in a child care setting.
- Spending time in crowded places.
- Having siblings who go to school or get child care services and bring home the infection.
Complications
Complications of severe bronchiolitis may include:
- Low oxygen in the body.
- Pauses in breathing, which is most likely to happen in babies born too early and in babies under 2 months old.
- Not being able to drink enough liquids. This can cause dehydration, when too much body fluid is lost.
- Not being able to get the amount of oxygen needed. This is called respiratory failure.
If any of these happen, your child may need to be in the hospital. Severe respiratory failure may require that a tube be guided into the windpipe. This helps your child breathe until the infection improves.
Prevention
Because the viruses that cause bronchiolitis spread from person to person, one of the best ways to prevent infection is to wash your hands often. This is especially important before touching your baby when you have a cold, flu or other illness that can be spread. If you have any of these illnesses, wear a face mask.
If your child has bronchiolitis, keep your child at home until the illness is past to avoid spreading it to others.
To help prevent infection:
- Limit contact with people who have a fever or cold. If your child is a newborn, especially a premature newborn, avoid being around people with colds. This is especially important in the first two months of life.
- Clean and disinfect surfaces. Clean and disinfect surfaces and items that people often touch, such as toys and doorknobs. This is especially important if a family member is sick.
- Wash hands often. Frequently wash your own hands and those of your child. Wash with soap and water for at least 20 seconds. Keep an alcohol-based hand sanitizer handy to use when you're away from home. Make sure it contains at least 60% alcohol.
- Cover coughs and sneezes. Cover your mouth and nose with a tissue. Throw away the tissue. Then wash your hands. If soap and water aren't available, use a hand sanitizer. If you don't have a tissue, cough or sneeze into your elbow, not your hands.
- Use your own drinking glass. Don't share glasses with others, especially if someone in your family is ill.
- Breastfeed, when possible. Respiratory infections are less common in breastfed babies.
Immunizations and medicines
In the U.S., respiratory syncytial virus (RSV) is the most common cause of bronchiolitis and pneumonia in children who are less than a year old. Two options for immunization can help prevent young infants from getting severe RSV. Both are recommended by the American Academy of Pediatrics, the American Academy of Family Physicians, the American College of Obstetricians and Gynecologists, and others.
You and your healthcare professional should discuss which option is best to protect your child:
- Antibody product called nirsevimab (Beyfortus). This antibody product is a single-dose shot given in the month before or during RSV season. It's for newborn babies and those younger than 8 months born during or entering their first RSV season. In the U.S., the RSV season typically is November through March, but it varies in Florida, Alaska, Hawaii, Puerto Rico, Guam and other U.S. Pacific Island territories.
- Nirsevimab also should be given to children 8 months through 19 months old who are at higher risk of severe RSV disease through their second RSV season. Higher risk conditions include:
- Children with active chronic lung disease from being born too soon (prematurely).
- Children with a severely weakened immune system.
- Children with severe cystic fibrosis.
- American Indian or Alaska Native children.
In rare situations, when nirsevimab is not available or a child is not eligible for it, another antibody product called palivizumab may be given. But palivizumab requires monthly shots given during the RSV season, while nirsevimab is only one shot. Palivizumab is not recommended for healthy children or adults.
- Vaccine for pregnant people. The FDA approved an RSV vaccine called Abrysvo for pregnant people to prevent RSV in infants from birth through 6 months of age. A single-dose shot of Abrysvo can be given sometime from 32 weeks through 36 weeks of pregnancy during September through January in the U.S. Abrysvo is not recommended for infants or children.
Other viruses can cause bronchiolitis too. These include COVID-19 and influenza or flu. Getting seasonal COVID-19 and flu shots every year is recommended for everyone older than 6 months.