Overview
Athlete's foot, also called tinea pedis, is a skin infection caused by fungi. It usually starts between the toes. The condition can occur when feet get hot and sweaty inside closed shoes.
Signs and symptoms of athlete's foot include an itchy, scaly rash. The fungus can live on floors, bedding, towels and shoes, spreading easily to others.
Athlete's foot is closely related to other fungal infections such as ringworm and jock itch. It can be treated with antifungal medicines. But it often comes back.
Products & Services
Symptoms
Athlete's foot
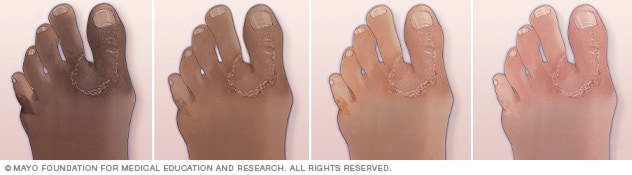
Athlete's foot
Illustration of athlete’s foot on different skin colors. The fungal infection causes scaly rash that may itch, sting or burn.
Athlete's foot can affect one or both feet. Common symptoms are:
- Scaly, peeling or cracked skin between the toes.
- Itchy skin, especially right after taking off socks and shoes.
- Swollen skin that may look red, purple or gray, depending on your skin color.
- Burning or stinging.
- Blisters.
- Dry, scaly skin on the bottom and sides of the foot.
When to see a doctor
Athlete's foot on side of foot
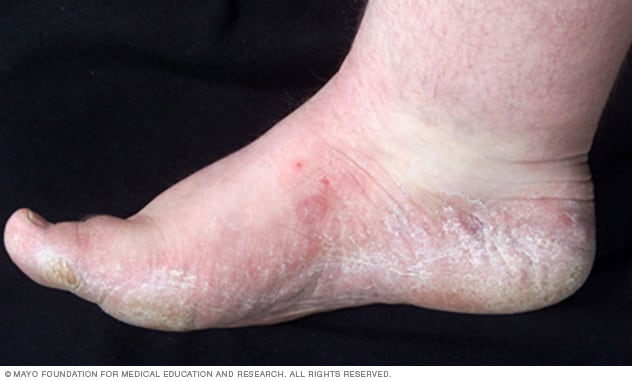
Athlete's foot on side of foot
Athlete's foot can cause dry, scaly skin on the bottom and sides of the foot.
If you have a rash on your foot that doesn't improve after two weeks of using an antifungal cream that you can buy over the counter, see your healthcare professional.
If you have diabetes, see your healthcare professional if you think you have athlete's foot. Also see your healthcare professional if you have symptoms of an infection, such as swelling of the affected area, pus and fever.
Causes
Athlete's foot is caused by the same type of fungi, called dermatophytes, that cause jock itch and ringworm. They thrive in warm, damp places such as sweaty socks and shoes and wet towels.
The fungi that cause athlete's foot spread easily to other people because they can travel on hands, towels and other surfaces. You can get athlete's foot through contact with someone who has it and by touching surfaces that have the fungus on them. The fungi also can spread from the feet to other parts of the body. This may happen if you use a towel to dry your feet and then use the same towel to dry the rest of your body.
Risk factors
You have a higher risk of athlete's foot if you:
- Often wear enclosed footwear.
- Sweat a lot.
- Share towels, shoes, rugs or bed linens with someone who has athlete's foot.
- Walk barefoot in public showers, pools or locker rooms.
Complications
A complication of athlete's foot is the spread of fungi to other parts of the body. For example, if the fungi that cause athlete's foot spread to the groin, they can cause jock itch.
Athlete's foot sometimes can lead to a bacterial infection. People with weakened immune systems, such as those with diabetes, may develop a serious skin infection called cellulitis.
Prevention
These tips can help you prevent athlete's foot or lower your risk of getting or spreading the fungus:
- Let your feet breathe. Wear sandals or open-toe shoes when possible.
- Wash your feet every day. Use warm, soapy water. Dry your feet well, especially between the toes.
- Use an antifungal powder, spray or ointment. After washing your feet, apply an antifungal medicine that you can buy over the counter.
- Change your socks regularly. Change them at least once a day or more often if your feet get very sweaty. Choose socks made from fabrics that absorb moisture, such as cotton. They help keep your feet drier than those made from artificial fabric, such as nylon.
- Rotate pairs of shoes. Wear different shoes from day to day. This gives your shoes time to dry after each use.
- Protect your feet in public places. Wear waterproof sandals or shoes around public pools, showers and locker rooms.
- Don't share shoes, towels or unwashed bedding with others. The fungi can live on these items.
Jan. 06, 2026