Ventricular tachycardia ablation
Ventricular tachycardia ablation, also called VT ablation, uses cold or heat energy to create tiny scars in the heart. The scars block faulty signals that cause a rapid, erratic heartbeat.
VT ablation is a treatment for a type of irregular heartbeat called ventricular tachycardia. Ventricular tachycardia occurs when the heart's signals make the lower heart chambers beat too quickly. The lower heart chambers are called the ventricles. The goal of VT ablation is to restore a regular heart rhythm.
Why it's done
Related information
Ventricular tachycardia
This type of cardiac ablation may be done if you have a type of fast, erratic heartbeat called ventricular tachycardia. If you have an implantable cardioverter-defibrillator (ICD), VT ablation may reduce the number of shocks you receive from the device.
VT ablation isn't recommended for all types of ventricular tachycardia. Your care team may suggest medicines and other procedures first.
Discuss your treatment options with a healthcare professional. Together you can talk about the pros and cons of VT ablation.
What you can expect
Epicardial ablation
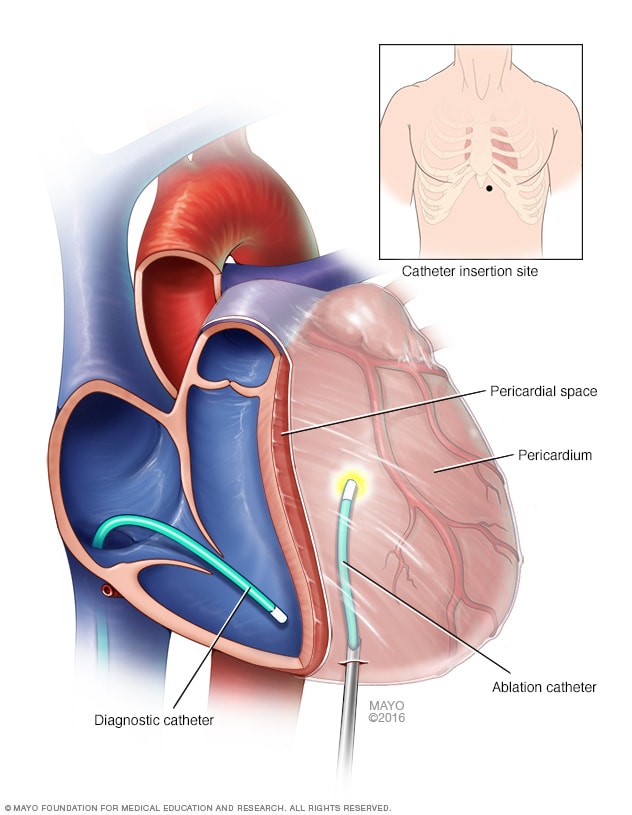
Epicardial ablation
Epicardial ablation is a treatment for irregular heartbeats. During epicardial ablation, heat or cold energy is used to create tiny scars on the outside of the heart. The scars block faulty electrical signals that cause the heart to beat too fast. During the treatment, tubes called catheters are used. The tubes go through the skin on the chest and into the space around the heart, called the pericardial space.
Ventricular tachycardia ablation is done in the hospital. Before the procedure, you usually get a medicine called a sedative that helps you relax.
The amount of sedation needed for the procedure depends on the specific type of irregular heartbeat and your overall health. You may be fully awake or lightly sedated. Some people get a combination of medicines, called general anesthesia, to put them in a sleep-like state.
The doctor inserts a long flexible tube called a catheter into a blood vessel, usually in the groin area. The catheter is gently guided to the heart.
Sensors on the tip of the catheter send electrical signals and record the heart's electricity. Your care team uses this information to determine the best place to apply the VT ablation treatment.
One of the following ablation techniques is used to create small scars in the heart and block irregular heart rhythms.
- Heat, known as radiofrequency energy.
- Extreme cold, known as cryoablation.
VT ablation may be done from inside or outside the heart. Sometimes, treatment is done at both locations.
- Inside the heart. If the irregular heartbeat is coming from inside the heart, the doctor guides the catheter to this area. Heat or cold energy is applied to the target area. The energy damages the tissue and causes scarring. This helps block the electrical signals that cause ventricular tachycardia.
- Outside the heart, also called epicardial ablation. If the irregular heartbeat starts in tissue outside the heart, the doctor places a needle through the skin on the chest and into the lining of the fluid-filled sack around the heart. A hollow tube called a sheath is then inserted. Flexible tubes called catheters go through the sheath to access the outside surface of the heart. Heat or cold energy can be used during epicardial ablation.
VT ablation takes about 3 to 6 hours. Afterward, you go to a recovery area where a care team closely watches you. You may stay overnight in the hospital.
Results
Most people see improvements in their quality of life after VT ablation. You may feel less tired or experience fewer ICD shocks. However, sometimes the irregular heart rhythm returns. You may need a repeat procedure, or you and your care team might discuss other treatments.
Feb. 02, 2024