Overview
Vagus nerve stimulation involves using a device to send electrical impulses to the vagus nerve. The vagus nerve is the main nerve of the system that controls digestion, heart rate and other vital functions. When the device fires, it sends electrical impulses to areas of the brain. This changes brain activity to treat certain conditions.
Devices for vagus nerve stimulation include one the Food and Drug Administration (FDA) approved that goes into the body, to treat epilepsy and depression. It works by sending impulses to areas of the brain that cause seizures and affect mood.
The FDA has approved another vagus nerve stimulation device for use after a stroke. For people who have trouble using their hand or arm after a stroke, the device helps make new pathways in the brain during exercise. This can help people regain the use of the affected hand or arm.
Surgeons put these devices under the skin in the chest. A wire threaded under the skin connects the device to the left vagus nerve. The device sends electrical signals along the left vagus nerve to the brainstem to affect the brain.
There's also a vagus nerve on the right side of the body. Surgeons don't often use the right vagus nerve because it's more likely to affect how the heart works.
There are newer vagus nerve stimulation devices that don't need surgery to implant the device. The FDA has approved one such device in the United States to treat cluster headaches and migraine. This device works by holding it against the skin of the neck. The device blocks pain signals to prevent or relieve head pain.
Researchers study ways to use vagus nerve stimulation to treat other conditions, as well. Research is looking at using the therapy for rheumatoid arthritis, inflammatory bowel disease, bipolar disorder, obesity and Alzheimer's disease.
Products & Services
Why it's done
Implanted vagus nerve stimulation
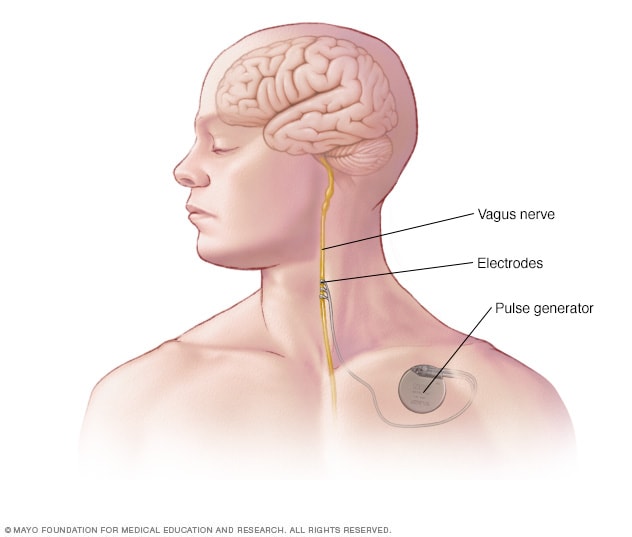
Implanted vagus nerve stimulation
In vagus nerve stimulation, a device placed under the skin of the chest stimulates the vagus nerve in the neck. This sends signals to the brain that lessen seizures.
Implantable vagus nerve stimulation devices can treat a number of conditions.
Epilepsy
Anti-seizure medicines don't fully manage seizures for about one-third of people with epilepsy. For some of them, vagus nerve stimulation may help manage their seizures.
The FDA has approved vagus nerve stimulation for people with epilepsy who:
- Are 4 years old and older.
- Have focal epilepsy. In focal epilepsy, one area of the brain causes the seizures.
- Can't fully manage their seizures with medicines.
Healthcare professionals also may use vagus nerve stimulation for people with generalized epilepsy.
Depression
Vagus nerve stimulation may help people with depression. It may be used when medicines, psychological counseling and electroconvulsive therapy haven't worked well.
The FDA has approved vagus nerve stimulation for the treatment of depression in adults who:
- Have long-lasting, hard-to-treat depression, known as treatment-resistant depression.
- Haven't improved after trying four or more medicines, electroconvulsive therapy or both.
- Keep using their other depression treatments with vagus nerve stimulation.
Stroke recovery
For people who are recovering from a stroke, the FDA has approved vagus nerve stimulation for use in rehabilitation. Vagus nerve stimulation with rehabilitation may help people recover the use of their hands and arms after an ischemic stroke.
Risks
Having a vagus nerve stimulator put into the body is safe for most people. But it does have some risks. These come both from the surgery to implant the device and from the brain stimulation.
Surgery risks
Surgical complications with implanted vagus nerve stimulation are rare. They're like the risks of having other types of surgery. They include:
- Pain where the cut is made to put the device in.
- Infection.
- Trouble swallowing.
- Vocal cords that can't move, called paralysis. This usually doesn't last long, but not always.
Side effects after surgery
Some of the side effects linked with implanted vagus nerve stimulation can include:
- Voice changes.
- A hoarse voice.
- Throat pain.
- Cough.
- Headaches.
- Shortness of breath.
- Trouble swallowing.
- Tingling or prickling of the skin.
- Trouble sleeping.
- Worse sleep apnea.
For most people, side effects ease over time. Most people can tolerate them. But some side effects may remain for as long as you use implanted vagus nerve stimulation.
Changing the electrical impulses may help ease these effects. If you can't stand the side effects, a healthcare professional can shut off the device.
How you prepare
Think about the benefits and risks of implanted vagus nerve stimulation before having the procedure. Make sure you know all your treatment choices. Be sure that you and your healthcare professional feel that implanted vagus nerve stimulation is the best treatment for you. Ask your healthcare team what to expect during surgery and after the device is in place.
Food and medicines
You may need to stop taking certain medicines ahead of surgery. Your surgeon may ask you not to eat or drink for a certain number of hours before the procedure.
What you can expect
Before the procedure
Before surgery, you have a physical exam. Your surgeon may have you start taking antibiotics before surgery to prevent infection.
During the procedure
Surgery to implant the vagus nerve stimulation device often is done on an outpatient basis. You go home that day. During surgery, you'll likely get medicine, called general anesthesia, to put you into a sleeplike state.
The surgery itself doesn't involve the brain. The surgeon makes two cuts, called incisions. One is on the chest or in the armpit area. The other is on the left side of the neck.
The surgeon puts the pulse generator in the upper left side of the chest. The pulse generator is about the size of a stopwatch. It runs on battery power.
A lead wire connects to the pulse generator. The surgeon guides the lead wire under the skin from the chest up to the neck. Then the surgeon connects the wire to the left vagus nerve through the second cut.
The device and its battery last for years before it needs to be replaced. A surgeon also can remove it, if needed.
Video: Vagus nerve stimulation
It’s called vagus nerve stimulation. Surgeons implant a device near the collarbone and run a wire to the vagus nerve. When the device fires it stimulates that nerve to send signals to the brain. This increases activity in areas that control mood.
After the procedure
If you had the device implanted to treat epilepsy or depression, your healthcare team turns on the pulse generator during a medical visit a few weeks after surgery. Then the team programs how long and how often the device sends electrical impulses to the vagus nerve.
Vagus nerve stimulation most often starts at a low level. Your healthcare team can raise it depending on your symptoms and side effects.
The device turns on and off in cycles, such as 30 seconds on, five minutes off. You may feel some tingling or slight pain in your neck. Your voice may be hoarse when the device is on.
Newer models that treat epilepsy can sense a sudden increase in your heart rate and react by sending a signal to the nerve. A sudden increase in heart rate may mean you're about to have a seizure. You can use a hand-held magnet to start the impulse at other times. For instance, you can turn it on if you feel you're about to have a seizure.
For a device that's put in after a stroke, a specialist most often turns it on during rehabilitation. You also can turn it on at home using a magnet. You might turn it on to help with certain tasks such as cooking.
You need to make follow-up visits to your healthcare professional to make sure that the pulse generator is working and hasn't moved out of place. Check with your healthcare team before having medical tests, such as an MRI. The test might affect the device.
Results
Vagus nerve stimulation isn't a cure for epilepsy. Most people with epilepsy won't stop having seizures. Most keep taking epilepsy medicine after the procedure. But some people have up to 50% fewer seizures. The seizures also may be less intense.
It can take months or even more than a year with the device before you have fewer seizures. Vagus nerve stimulation also may shorten the recovery time after a seizure. People who have vagus nerve stimulation to treat epilepsy also may see their moods and quality of life get better.
Research on how well implanted vagus nerve stimulation works for depression is ongoing. Some studies suggest the effects of vagus nerve stimulation for depression build over time. It may take at least several months of treatment before your depression symptoms start to ease.
Implanted vagus nerve stimulation doesn't work for everybody with depression. And it isn't meant to replace other treatments.
Studies have found that vagus nerve stimulation paired with rehabilitation helped improve function in people who had a stroke. It also may help people who have problems with thinking and swallowing after a stroke. Research is ongoing.
Some health insurance carriers may not pay for this procedure.
Studies of implanted vagus nerve stimulation as a treatment for other conditions have been too small to know whether the treatment works. Other conditions include Alzheimer's disease, rheumatoid arthritis, inflammatory bowel conditions and heart failure. More research is needed.
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.
Dec. 20, 2024