Risks
A breast self-exam for breast awareness is a safe way to become familiar with the typical look and feel of your breasts.
However, there are some limitations and risks, including:
Worry caused by finding a lump
Most of the changes or lumps people find in their breasts aren't cancerous. Still, finding something suspicious in your breast can make you worry about what it may mean. You may endure several days of worry until you can see your healthcare professional.
Other tests may be needed
If you discover a suspicious lump, you may need other tests and procedures to check it out. This might include imaging tests such as a diagnostic mammogram or a breast ultrasound. You also may have a procedure to remove breast tissue for testing, called a biopsy. If it turns out the lump isn't cancer, you might feel that you've had an invasive procedure without needing one.
Overestimating the benefits
A breast self-exam doesn't replace a breast exam by your healthcare professional, called a clinical breast exam. It also doesn't replace a screening mammogram. Becoming familiar with the typical look and feel of your breasts can be used with breast cancer screening but can't replace it.
How you prepare
To prepare for your breast self-exam for breast awareness:
Ask a healthcare professional to show you how to do the exam
Before you begin breast self-exams for breast awareness, you may find it helpful to discuss the instructions and technique with your healthcare professional.
If you menstruate, do the exam after your period
Hormone levels fluctuate each month during the menstrual cycle. This causes changes in breast tissue, such as swelling, and may cause breast tenderness. Breast swelling begins to decrease at the start of a period. The best time to perform a self-exam for breast awareness is usually the week after your period ends.
What you can expect
Begin by looking at your breasts
Sit or stand shirtless and braless in front of a mirror with your arms at your sides. To inspect your breasts visually, do the following:
- Face forward and look for puckering, dimpling, or changes in size, shape or symmetry.
- Check to see if your nipples are turned in.
- Inspect your breasts with your hands pressed down on your hips.
- Inspect your breasts with your arms raised overhead and the palms of your hands pressed together.
- Lift your breasts to see if ridges along the bottom are symmetrical.
If you have a vision condition that makes it difficult for you to visually inspect your breasts, ask a trusted friend or a family member to help you.
Next, use your hands to examine your breasts
Breast self-exam
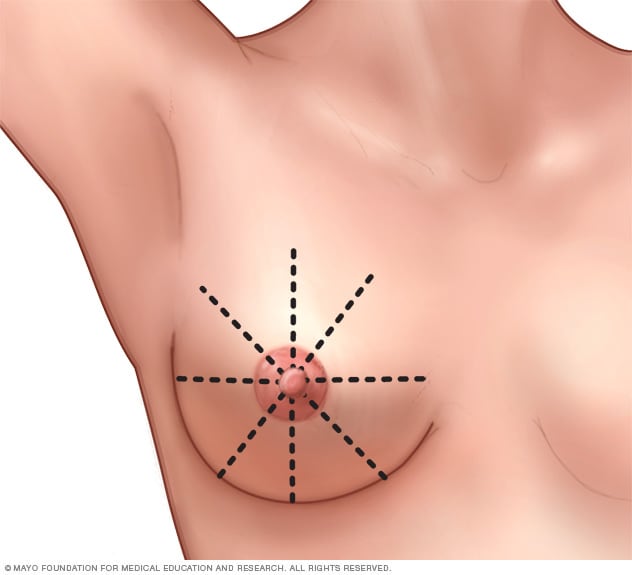
Breast self-exam
To perform a breast self-exam for breast awareness, follow a pattern that ensures you cover your entire breast. For instance, imagine that your breasts are divided into equal wedges, like pieces of a pie. Move your fingers along each piece in toward your nipple.
Common ways to perform the manual part of the breast exam include:
- Lying down. Choose a bed or other flat surface to lie down on your back. When you're lying down, breast tissue spreads out. This makes the tissue thinner and easier to feel.
- In the shower. Lather your fingers and breasts with soap to help your fingers glide more smoothly over your skin.
When examining your breasts, some general tips to keep in mind include:
- Use the pads of your fingers. Use the pads, not the very tips, of your three middle fingers for the exam. If you have difficulty feeling with your finger pads, use another part of your hand that is more sensitive. This may include your palm or the backs of your fingers.
- Use different pressure levels. Your goal is to feel different depths of the breast by using different levels of pressure to feel all the breast tissue. Use light pressure to feel the tissue closest to the skin, medium pressure to feel a little deeper, and firm pressure to feel the tissue closest to the chest and ribs. Be sure to use each pressure level before moving on to the next spot. If you're not sure how hard to press, talk with your healthcare professional.
- Take your time. Don't rush. It may take several minutes to carefully examine your breasts.
- Follow a pattern. Use a methodical technique to ensure you examine your entire breast. For instance, imagine the face of a clock or the slices of a pie over your breast. Begin near your collarbone and examine that section, moving your fingers from the outside edge of the breast toward your nipple. Then move your fingers to the next section.
If you have a condition that makes it difficult for you to examine your breasts using this technique, you likely can still do a breast self-exam. Ask your healthcare professional to show you ways you can examine your breasts.
Results
What's typical
Finding a change in your breast isn't a reason to panic. Some breast changes are typical. For instance, if you have periods, you might notice that your breasts change at certain times in the menstrual cycle. It's common for the breasts to feel different in different places. A firm ridge along the bottom of each breast is typical, for instance. The look and feel of your breasts will likely change as you age.
When to contact a healthcare professional
Make an appointment with a doctor or other healthcare professional if you notice:
- A hard lump or knot near your underarm.
- A recent change in a nipple to being pushed in instead of sticking out.
- Bloody nipple discharge.
- Changes in skin color, warmth, swelling or pain.
- Changes in the way your breasts look or feel, including thickening or noticeable fullness that is different from the surrounding tissue.
- Dimples, puckers, bulges or ridges on the skin of your breast.
- Itching, scales, sores or rashes.
Your healthcare professional may suggest more tests and procedures to investigate breast changes. Tests and procedures may include a clinical breast exam, a mammogram and an ultrasound.