May 21, 2022
Nonobstructive azoospermia (NOA) is the absence of sperm in the ejaculate due to a failure in spermatogenesis. It is the most severe form of male infertility caused by intrinsic testicular failure or inadequate gonadotropin production. However, microsurgical testicular sperm extraction (microTESE) may offer men with a diagnosis of NOA a pathway to biological parenthood.
Seminiferous tubules within the testicle
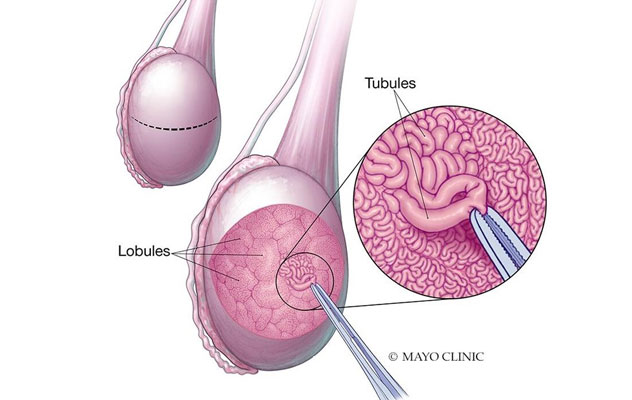
Seminiferous tubules within the testicle
During microTESE, a surgeon retrieves sperm from the seminiferous tubules of the testis.
According to the most recent American Urological Association and American Society for Reproductive Medicine male infertility guidelines, men with NOA should be offered microTESE. MicroTESE is a surgical procedure where sperm is retrieved from the seminiferous tubules of the testis.
How is microTESE performed?
Operating microscope magnification
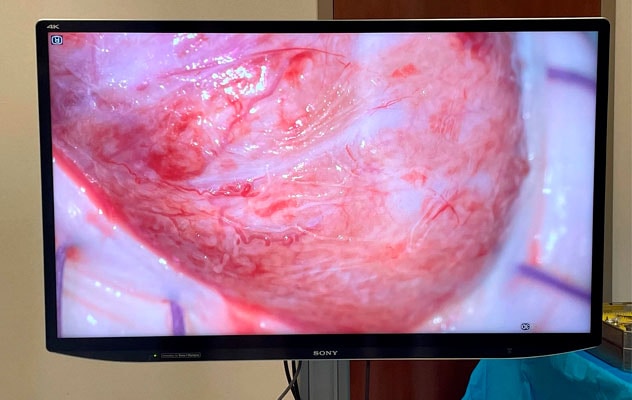
Operating microscope magnification
The seminiferous tubules of the testis are magnified 10 to 15 times.
While patients with NOA may not have sperm detectable on a semen analysis, they may have focal areas of sperm production within the testis. During a typical microTESE procedure, a surgeon spends hours searching for sperm using an operating microscope. And a reproductive endocrinology lab technologist can spend up to 14 hours searching under a bench-top microscope. Here is what the surgical field looks like during the procedure at 10 to 15 times magnification.
Sperm retrieval rates are 40% to 60% for microTESE, and any sperm found needs to be used for in vitro fertilization (IVF) and intracytoplasmic sperm injection (ICSI). Due to the specialized nature of this procedure, it is typically done at a facility in conjunction with reproductive endocrinologists. MicroTESE has traditionally been performed in the operating room under general anesthesia, posing a financial barrier for couples who do not have insurance coverage for fertility care.
How is Mayo Clinic making microTESE more accessible for patients?
At Mayo Clinic in Rochester, Minnesota, Sevann Helo, M.D., performs microTESE in the office setting using oral sedation and the 3D surgical microscope. Dr. Helo says, "It's a game-changer for patients who are paying out of pocket for a procedure that can cost upward of $10,000 when done in the operating room, with no guarantee that we will be able to find sperm. We've been able to bring that cost down substantially to make the dream of microTESE and IVF-ICSI attainable for more couples."
When asked about the difficulty of introducing this procedure into the office setting, Dr. Helo states: "It was a natural extension of the other microsurgical procedures that I offer in the office, including vasectomy reversal and varicocelectomy. While there are some nuances to managing patient comfort for microTESE, the feedback we have received thus far is that patients are appreciative that they could receive world-class care at an affordable price."
For more information
Schlegel PN, et al. Diagnosis and treatment of infertility in men: AUA/ASRM guideline part II. Journal of Urology. 2021;205:44.
Schlegel PN. Testicular sperm extraction: Microdissection improves sperm yield with minimal tissue excision. Human Reproduction (Oxford, England). 1999;14:131.
Refer a patient to Mayo Clinic.