Aug. 21, 2018
In the warmer Minnesota months, families dust off their child-sized ATVs, lawn mowers and trampolines. Children in every neighborhood are playing on monkey bars and riding bicycles. Unfortunately, relearning some of these skills or ignoring rules for proper usage can lead to pediatric orthopedic injuries. Though more rare, motor vehicle collisions with children involved also occur during the warm season.
Recognizing the differences in caring for children
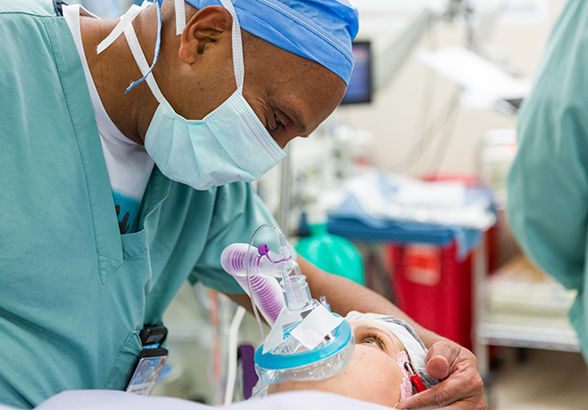 A physician reassures a pediatric patient before surgery
A physician reassures a pediatric patient before surgery
Orthopedic injuries in children are different from those in adults in several ways:
Anesthesiology
Orthopedic injuries in children require a pediatric anesthesiologist who's completed a one-year subspecialty fellowship in caring for infants and children.
Growth plate issues
If a child's growth plate is injured, the child must be followed for many years by a pediatric subspecialist to ensure growth is not arrested, which dictates treating the child differently from an adult with the same injury. For example, in an adult with a femoral shaft fracture, the physician places a rod along the length of the bone. In a child, however, the same injury requires use of skinny rods tailored to circumvent the growth plate to avoid stunting growth.
Casts
Many pediatric injuries can be treated with a cast, which requires personnel comfortable with applying up to full-body casts in children.
"Children are not small adults," says Todd A. Milbrandt, M.D., a pediatric orthopedic surgeon at Mayo Clinic in Rochester, Minnesota. "There are different treatment principles for them that make them a unique patient population for management."
Considering transfer of children with fractures
In an article published in Orthopedics in 2015, the authors reported that orthopedics has become increasingly subspecialized — 99 percent of orthopedic residency graduates complete a fellowship. Sometimes even orthopedic surgeons in the community not subspecializing in pediatrics may feel ill-equipped to take on operative pediatric cases, though many adult orthopedic injuries may be addressed in their facilities. In locations where there are no practicing pediatric orthopedic surgeons for miles in any direction, however, an orthopedic surgeon who likes to care for children may fill the niche.
To avoid double transfers of children with orthopedic injuries, it's important to identify the closest appropriate orthopedist. A number of factors may prompt transferring a child more than once, such as transfer to a hospital where providers gain a better picture of the injury and then decide an additional transfer is warranted. Double transfers also may be due to sending a child to a facility that appears well-suited to the injury's requirements, but not for pediatric patients.
"It would be easy to hit the transfer button and have a child end up in a place appropriate for adults who have the same injuries, but not appropriate for a pediatric injury," says Dr. Milbrandt.
If children are transferred more than once, they may face a number of risks, including:
- Missing the eight-hour deadline for surgery on open fractures, increasing the potential for deep infection
- Delay in treating a growth plate injury, which endangers future growth of the affected bone
- Inability to quickly relieve pressure surrounding a fracture or crushed limb, leading to ischemia, then damage to muscle and nerve, which may be permanent or, at worst, lead to loss of a limb or death
- Not being able to eat for up to 24 hours due to spending all day in transfer and then taken immediately to surgery
To prepare a child with an orthopedic injury for transfer, Dr. Milbrandt suggests antibiotics for open fractures, splint immobilization with plaster plus an elastic bandage, and X-ray if there is time while awaiting transfer to provide the receiving hospital more information for treatment planning. He does not recommend delaying transfer for imaging, however.
Reaching out to the community
As many pediatric orthopedic injuries may be preventable, Dr. Milbrandt strongly encourages trauma staff to be active in community outreach. For the warm weather months, he suggests addressing ATV and lawn mower risks to children, in particular. He recommends children be at least age 14 to operate ATVs, which can travel as fast as motor vehicles, with severe consequences. For lawn mower safety, Dr. Milbrandt feels strongly that children should not ride on the lap of an adult operating a riding mower or be the sole mower operator until age 13, when a child is old enough to adequately push the machine.
"Adults, and sometimes grandparents in particular, think they are doing a good thing riding on a lawn mower with a child," he says. "The safest thing, however, is having the child stay inside while an adult is mowing or remain in the front yard if an adult is mowing in the backyard."
For those interested in community outreach, Dr. Milbrandt is available to provide resources or consult, and can be reached at 507-284-3660.
For more information
Niesen MC, et al. Orthopedic surgery fellowships: The effects of interviewing and how residents establish a rank list. Orthopedics. 2015;38:175.