Oct. 27, 2023
Mayo Clinic offers the latest technology to maximize the safety and outcomes of neuro-oncological treatment. Technical advances are thoughtfully integrated into all aspects of patient care.
"Mayo Clinic is never satisfied with the status quo. We use the latest technology to improve patient outcomes and quality of life," says Alfredo Quinones-Hinojosa, M.D., chair of Neurosurgery at Mayo Clinic in Jacksonville, Florida.
Technical advances at Mayo Clinic include:
- Molecular prognostication for brain tumor treatment.
- Immunofluorescence for intraoperative imaging of meningiomas and other brain tumors.
- Artificial intelligence models for imaging brain tumors.
- MRI-guided focused ultrasound for the treatment of brain tumors.
- Proton therapy and future carbon ion treatment for brain tumors.
- Restorative and exoscopic neurosurgeries.
Before adopting new technologies, Mayo Clinic assesses the impact on patient care. "It's important to embrace new technology. But it's equally important to avoid investing in technologies that don't improve patient care in a meaningful way," says Bernard R. Bendok, M.D., chair of Neurosurgery at Mayo Clinic in Phoenix/Scottsdale, Arizona.
Precise laboratory testing and imaging
Critical tumor information
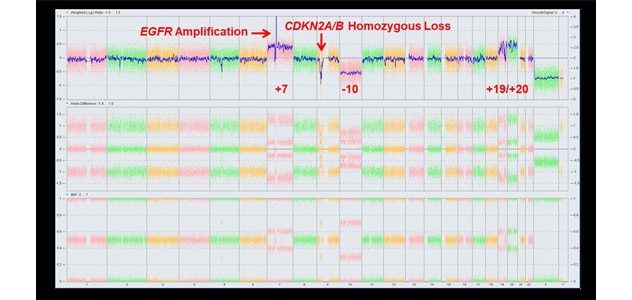
Critical tumor information
Genetic brain tumor test panel results show a typical chromosomal microarray pattern for telomerase reverse transcriptase-mutant isocitrate dehydrogenase wild-type glioblastoma.
Molecular diagnostics plays an increasingly important role in managing brain tumors. Testing panels available through Mayo Clinic Laboratories use targeted next-generation sequencing and chromosomal microarray to evaluate genetic mutations and rearrangements.
Subspecialized pathologists evaluate test results and report on individuals' diagnoses and prognoses. With the rapid pace of discovery of genes with clinical significance, Mayo Clinic researchers work constantly to update the panels.
"We always think about how we can improve our service to provide the best information for patients with brain tumors," says Robert B. Jenkins, M.D., Ph.D., a medical geneticist and pathologist in Mayo Clinic Comprehensive Cancer Center at Mayo Clinic in Rochester, Minnesota.
Innovative imaging provides additional precision for the diagnosis and treatment of neurological tumors.
"Mayo Clinic is never satisfied with the status quo. We use the latest technology to improve patient outcomes and quality of life."
Immunofluorescence is used for intraoperative visualization of meningiomas. That imaging modality typically has been used only during glioma resections. But Mayo Clinic participated in a multicenter, international clinical trial investigating immunofluorescence's impact on outcomes of meningioma resections.
"Immunofluorescence may show us more accurately where the tumor is," says Jamie J. Van Gompel, M.D., a neurosurgeon at Mayo Clinic's campus in Minnesota. "In the future, immunofluorescence might be helpful for all benign tumors."
Applying artificial intelligence to imaging is another important tool. Mayo Clinic researchers have developed a deep learning model that can distinguish MRI indications of tumor progression from pseudoprogression in individuals with glioma. As described in the September 2022 issue of the Journal of Neuro-Oncology, the model has 88.72% sensitivity and 76.4% accuracy in cases where neuroradiologists' interpretations indicated a high level of uncertainty.
"In an era of increasing personalization of therapy, the accurate stratification of tumor progression and pseudoprogression can facilitate decision-making for patients," Dr. Quinones-Hinojosa says.
Another deep learning model provides real-time, intraoperative delineation of cancer and noncancer brain tissues. Described in the January 2023 issue of Biomedical Optics Express, the ensemble model synergizes attenuation characteristics and texture features as shown on optical coherence tomography.
"This deep network cancer detector is capable of producing accurate segmentation maps in real time," Dr. Quinones-Hinojosa says. "The model has been designed and validated to be sensitive, specific, fast, stable, interpretable and superior to its individual components alone."
Ultrasound and precision radiation therapies
Mayo Clinic pursues innovative approaches — surgical and nonsurgical — for the treatment of neurological tumors.
MRI-guided focused ultrasound can be used to open the blood-brain barrier to deliver therapeutic agents into brain tumors. "This is a promising technology for understanding and treating brain tumors in new ways," says Timothy J. Kaufmann, M.D., M.S., a neuroradiologist at Mayo Clinic's campus in Minnesota. The approach is being evaluated in clinical trials.
Proton beam therapy precisely targets brain tumors, allowing for the delivery of higher doses of radiation. The treatment is especially useful for tumors in children and tumors near eloquent brain tissue.
"Proton therapy in the hippocampus reduces the likelihood of cognitive and memory deficits," Dr. Quinones-Hinojosa says. "For tumors near the temporal lobe, such as a vestibular schwannoma, there are fewer issues with hearing loss after radiation. There is also a potential reduction of effects on the pituitary gland. That is especially important when treating children because hormonal dysfunction can have devastating effects on growth and development."
 New construction
New construction
Artist's rendering of the integrated oncology facility under construction at Mayo Clinic in Jacksonville, Florida.
Mayo Clinic is currently the largest provider of proton beam therapy in the United States. Construction is underway on an expanded proton beam facility at Mayo Clinic's campus in Minnesota. Proton beam therapy also will be offered at the new integrated oncology facility under construction at Mayo Clinic's campus in Florida.
"Having proton therapy at all three of Mayo Clinic's main campuses is an exciting development that will greatly benefit our patients," Dr. Quinones-Hinojosa says.
The new oncology center also will include a carbon ion treatment facility. Carbon ion therapy — currently available at only a handful of centers in Asia and Europe — has the capability of killing cancer cells that are resistant to traditional radiation therapy.
"Like proton beam therapy, carbon ion therapy minimizes the radiation dose delivered to adjacent normal tissue. We are entering a new era with great potential for treating brain tumors," Dr. Quinones-Hinojosa says.
Surgical innovations
Mayo Clinic has demonstrated success with restorative surgery for individuals with vestibular schwannomas. Working with ENT surgeons, neurosurgeons perform stereotactic radiosurgery for tumor removal, followed by cochlear implantation.
"Focused ultrasound for blood-brain barrier opening is a promising technology for understanding and treating brain tumors in new ways."
In a study published in the July 2021 issue of the Journal of Neurosurgery, Mayo Clinic researchers found that most patients who had cochlear implantation after stereotactic radiosurgery for vestibular schwannoma enjoyed access to sound at near-normal levels.
"Stereotactic radiosurgery plus either immediate or delayed cochlear implantation may become the treatment of choice at Mayo Clinic for patients with tumors that are smaller than 25 millimeters but growing," Dr. Van Gompel says.
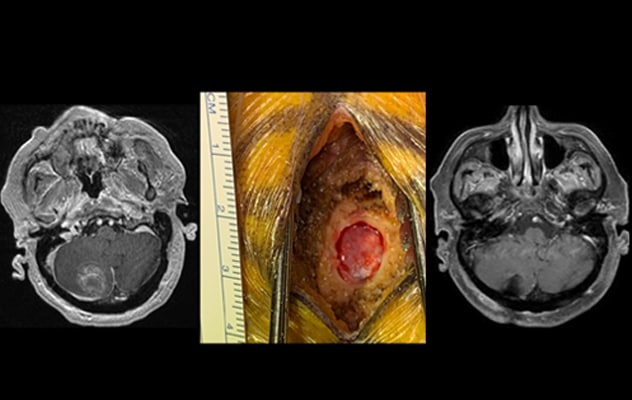 Minimally invasive tumor resection
Minimally invasive tumor resection
On the left, preoperative MRI shows a large cerebellar metastatic tumor. In the center, photograph shows the burr hole, measuring less than 14 millimeters, through which the tumor was resected. On the right, postoperative MRI shows complete resection. The patient went home on the day following the procedure.
Mayo Clinic's use of exoscopic visualization facilitates minimally invasive neurosurgery for selected patients. Compared with the endoscope, the exoscope provides a wider focus of view, greater magnification and oblique visualization angles.
"The exoscope is very ergonomic for the surgeon and allows us to get light down into areas where we couldn't before," says Kaisorn L. Chaichana, M.D., a neurosurgeon at Mayo Clinic's campus in Florida.
"Mayo Clinic's focus is always on doing what is best for patients," Dr. Bendok says. "Our hope is that increasingly effective neurosurgical technology and interventions will help alleviate suffering and improve quality of life."
For more information
Mayo Clinic Laboratories. Mayo Clinic.
Mayo Clinic Comprehensive Cancer Center. Mayo Clinic.
Clinical Trials: A Study to Evaluate Gleolan to Enhance Tumor Visualization in Patients with Newly-diagnosed or Recurrent Meningioma. Mayo Clinic.
Moassefi M, et al. A deep learning model for discriminating true progression from pseudoprogression in glioblastoma patients. Journal of Neuro-Oncology. 2022;159:447.
Wang N, et al. Deep learning-based optical coherence tomography image analysis of human brain cancer. Biomedical Optics Express. 2023;14:81.
Patel NS, et al. Cochlear implantation after radiosurgery for vestibular schwannoma. Journal of Neurosurgery. 2021;135:126.
Refer a patient to Mayo Clinic.