April 13, 2018
Magnetic resonance elastography (MRE) has revolutionized clinicians' ability to detect liver fibrosis by noninvasively measuring liver stiffness. Pathological changes occurring in the liver before cirrhosis that are also clinically important to identify include steatosis associated with nonalcoholic steatohepatitis (NASH), inflammation associated with viral hepatitis and congestion associated with cardiac hepatopathy. Detection of these changes provides essential diagnostic, prognostic and treatment information. In NASH, for example, early detection of liver inflammation would allow timely interventions to prevent progression to liver fibrosis and development of cirrhosis.
A research team of Mayo Clinic radiologists (Meng Yin, Ph.D., Richard L. Ehman, M.D.) and hepatologists (Alina M. Allen, M.D., Vijay Shah, M.D.) recently conducted a study to determine whether MRE technology can be adapted to use for the detection of NASH. "Development of a reliable, noninvasive method for diagnosing NASH is a major unmet need," explains Dr. Allen, a specialist in gastroenterology and hepatology at Mayo Clinic's campus in Minnesota and the study's primary investigator.
In advanced stages of NASH, conventional MRE's ability to measure liver stiffness provides an accurate measure of fibrosis. Conventional MRE, however, cannot differentiate mild fibrosis from inflammation, making it a less useful tool for assessing progression of NASH in its earlier stages.
"Our research was designed to examine the role of a multiparametric magnetic resonance elastography (MRE) protocol for the detection of NASH before onset of fibrosis," says Dr. Allen. The research team hypothesized that by generating the mechanical waves at different frequencies, early histologic changes of NASH (lobular inflammation, cellular ballooning) that affect viscoelastic properties, such as interstitial fluid pressure and viscosity, can be detected.
Study design
The Mayo research team prospectively enrolled a total of 88 participants who were scheduled to undergo bariatric surgery. Before surgery, study subjects underwent multifrequency 3-D MRE (at 30, 40 and 60 Hz) to assess which viscoelastic imaging parameters correlated with early histologic changes in NASH. MRI proton density fat fraction (MRI-PDFF) helped researchers quantify the degree of steatosis present.
Researchers used liver biopsy obtained during surgery to diagnose NASH, and they calculated histologic nonalcoholic fatty liver disease activity score (NAS) using the NASH Clinical Research Network criteria. The imaging parameters that correlated with steatosis, lobular inflammation and ballooning were selected using logistic regression. These imaging parameters were included in a predictive regression model of NASH diagnosis.
Results
Of the 88 subjects enrolled, 37 (42 percent) had biopsy-proven NASH. Most subjects had early-stage liver disease, while only three subjects had advanced fibrosis (stages F3-4 on a scale from 0 to 4). From the complex shear modulus output generated by MRE at multiple mechanical frequencies, the damping ratio and shear stiffness correlated with lobular inflammation and hepatocellular ballooning, respectively. The fat fraction obtained from MRI-PDFF correlated with steatosis (p < 0.05).
MRI-based predictive NAS and histologic NAS
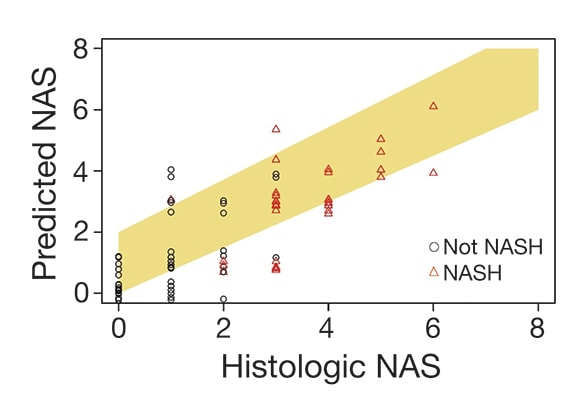
MRI-based predictive NAS and histologic NAS
Area under the receiver operating characteristic (AUROC) = 0.86. This yielded the following performance parameters: sensitivity = 0.68, specificity = 0.82, positive predictive value (PPV) = 0.74, negative predictive value (NPV) = 0.78. The relative agreement between the MRI-based predictive NAS and histologic NAS is illustrated in Figure (Spearman rho=0.78).
These three parameters (damping ratio, shear stiffness and fat fraction) were fit into a generalized linear model that had high predictive performance of biopsy-proven NASH.
Conclusions
"Our study determined that multifrequency 3-D MRE facilitates early detection of inflammation and ballooning in early NASH, and it predicts disease activity with a high degree of accuracy," explains Dr. Allen. "Based on these results, we have concluded that this imaging biomarker represents a promising alternative to liver biopsy for NASH diagnosis and monitoring.
"Obviating the impractical need for liver biopsy to diagnose NASH before fibrosis ensues would positively impact the care of NAFLD patients by enabling screening, monitoring serial changes or response to therapy," says Dr. Allen. "Expanding the use of MRI to an all-in-one diagnostic test for inflammation, steatosis, fibrosis and liver cancer has high potential to transform the clinical practice."
Dr. Allen notes that the research team is planning further testing on a larger sample size and validation in independent patient cohorts.
For more information
Allen AM, et al. SAT-464-Novel multiparametric magnetic resonance elastography (MRE) protocol accurately predicts NAS score for NASH diagnosis. Journal of Hepatology. 2017;66:S659.
Clinical trials: Transforming non-invasive liver disease detection by MRE: The Hepatogram. Mayo Clinic.