Diagnosis
To diagnose a spinal cord tumor, a healthcare professional might start by asking about your symptoms. The health professional might do an exam to see how your nerves are working. Other tests that can help diagnose a spinal cord tumor are imaging tests and biopsy.
Physical exam
A health professional may examine your body. This might involve checking your back for painful spots and other symptoms that might be concerning. This assessment also might include a neurological exam. This kind of exam tests different parts of your body to understand how your nerves are working. The health professional may check your balance, coordination, strength and reflexes.
Spinal magnetic resonance imaging
MRI scan of spinal cord tumor
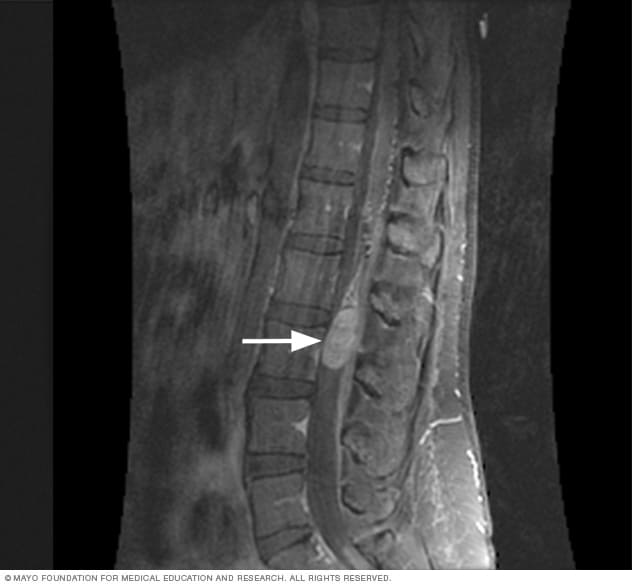
MRI scan of spinal cord tumor
Magnetic resonance imaging, also called MRI, is often used to detect a spinal cord tumor. The white arrow in this MRI scan image points to a spinal cord tumor.
Magnetic resonance imaging uses a powerful magnetic field and radio waves to make pictures of the inside of the body. This test also is called an MRI. A spinal MRI can make detailed pictures of your spinal cord. MRI is usually the preferred test to detect spinal cord tumors.
A member of your healthcare team might put a dye into a vein in your hand or arm during the MRI. This dye, called a contrast agent, helps make clearer pictures.
Spinal computerized tomography scan
A computerized tomography scan uses X-ray techniques to create detailed images of the body. It then uses a computer to create cross-sectional images, also called slices, of the inside of the body. This test also is called a CT scan.
A spinal CT scan can make detailed pictures of the spine. Sometimes a healthcare professional puts a dye into your vein for this test. The dye helps make clearer pictures. Spinal CT isn't typically used to diagnose a spinal cord tumor. But it might give your healthcare team more information to help understand your condition.
Spinal cord tumor biopsy
A biopsy is a procedure to remove a sample of tissue for testing in a lab. In the lab, tests can show the type of spinal cord tumor that you have.
To get the tissue sample, a healthcare professional might put a needle through the skin and into the spine. The health professional uses the needle to draw out some tissue from the spinal cord tumor. The sample goes to a lab for testing. Results help the healthcare team make a treatment plan.
Often a surgeon removes a sample of tissue from the spinal cord tumor during surgery. The sample might be tested right away. The results tell the surgeon what type of cells are involved in the tumor. The type might help the surgeon decide whether to continue with surgery to remove the spinal cord tumor.
More Information
Treatment
The main treatment for spinal cord tumor is surgery. Sometimes treatment involves radiation therapy and chemotherapy.
The goal of treatment is to remove the spinal cord tumor completely. But this might not be possible. Surgery carries a risk of hurting the spinal cord and the nerves around it. So healthcare teams must carefully plan the surgery to lower the risk.
When creating your spinal cord tumor treatment plan, your healthcare team considers many factors. These factors include the type of tumor you have, where it is in your spine, and whether the tumor affects the spinal cord or the tissue around it. Your healthcare team also considers your overall health and what you prefer.
Monitoring
Some spinal cord tumors don't cause symptoms. If a small tumor is growing slowly and not causing symptoms, treatment might not be needed right away.
Instead, your healthcare team might watch the tumor closely to see if it shows signs of growing. This might include imaging tests every so often.
Surgery for spinal cord tumors
Spinal tumor neck surgery
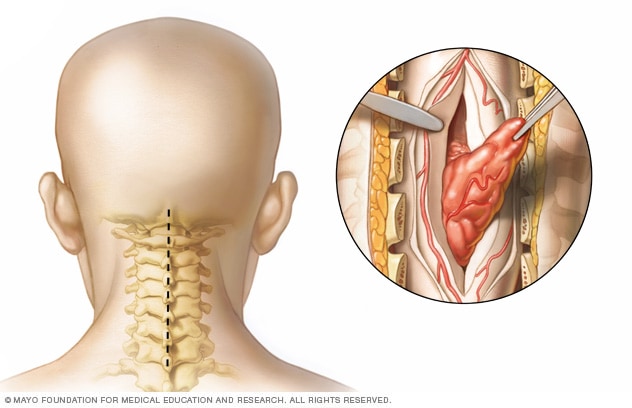
Spinal tumor neck surgery
This image shows a spinal cord tumor being removed from the neck. To access the spinal cord, a surgeon makes a cut along the spine.
The goal of surgery is to remove all of the spinal cord tumor. Your healthcare team will carefully consider whether surgery might hurt your spinal cord. If there's a good chance that surgery won't cause long lasting damage, surgery might be an option for you.
For most spinal cord tumors, the surgeon makes a cut in the back or neck to access the spine. The surgeon removes parts of some spine bones to get to the spinal cord. The surgeon uses a high-powered microscope and surgical tools to carefully remove the spinal cord tumor.
Surgeons can monitor the function of the affected nerves during surgery. This may lower the risk of hurting the nerves. Some procedures involve very high-energy sound waves to break up a tumor and make it easier to remove. These and other techniques are making spinal surgery safer for more people with spinal cord tumors.
But even with the latest advances in surgery, not all spinal cord tumors can be removed completely. If that happens, the surgeon might remove as much of the tumor as is possible. Then other treatments might be used after surgery.
Recovery from spinal surgery may take weeks or months, depending on the procedure. It's common to have changes in feeling or loss of function right after surgery. Often these changes may start to get better slowly. Whether changes in function are long lasting will depend on your situation. Talk with your healthcare team about what you can expect.
Radiation therapy for spinal cord tumors
Radiation therapy treats tumors with powerful energy beams. The energy can come from X-rays, protons or other sources. During radiation therapy, you lie on a table while a machine moves around you. The machine directs radiation to precise points on your body.
Radiation might be used after surgery. It can help kill tumor cells that remain after surgery. Radiation might help slow a tumor's growth if surgery isn't possible.
Chemotherapy for spinal cord tumors
Chemotherapy treats cancer with strong medicines. Many chemotherapy medicines exist. Most chemotherapy medicines are given through a vein. Some come in pill form.
Chemotherapy doesn't work for all spinal cord tumors. It tends to work better in spinal cord tumors that are growing quickly, such as some spinal cord cancers.
Chemotherapy might be used after surgery. It can help kill tumor cells that remain.
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Alternative medicine
No alternative medicines have been proved to cure spinal cord tumors. But some complementary and alternative treatments may help with symptoms.
People with spinal cord tumors sometimes have pain. Your healthcare team may offer treatments that help. Sometimes complementary treatments also can give some relief from pain. Treatments that might help include:
- Acupuncture.
- Hypnosis.
- Massage.
- Mindfulness practices, such as meditation and guided imagery.
- Relaxation exercises.
- Spiritual practices, such as prayer.
Talk about the risks and benefits of complementary treatments with your healthcare team. Some treatments, such as herbal remedies, could interfere with medicines you're taking.
Coping and support
Learning that you have a spinal cord tumor can feel overwhelming. But you can take steps to cope after your diagnosis. Consider trying to:
Find out all you can about your spinal cord tumor
Write down your questions, bring them to your appointments, and ask your healthcare professional your questions. Take notes, or ask a friend or family member to come along to take notes.
The more you and your family know and understand about your care, the more confident you'll feel when it is time to make treatment decisions.
Get support
Find someone you can share your feelings and concerns with. You may have a close friend or family member who is a good listener. Or speak with a clergy member or counselor.
Other people with spinal tumors may be able to offer unique insights. Ask your healthcare team about support groups in your area and online.
Take care of yourself
Choose a healthy diet rich in fruits, vegetables and whole grains whenever possible. Check with your healthcare professional to see when you can start exercising again. Get enough sleep so that you feel rested.
Reduce stress in your life by taking time for relaxing activities, such as listening to music or writing in a journal.
Preparing for your appointment
Make an appointment with a doctor or other healthcare professional if you have any symptoms that worry you. If your health professional thinks you might have a condition affecting the spinal cord, that person may refer you to a neurologist. A neurologist is a doctor who specializes in conditions that affect the brain, spinal cord and nerves.
If you learn that you have a spinal cord tumor, you might meet with surgeons. These may be surgeons who operate on the brain and spinal cord, called neurosurgeons, and surgeons who operate on the spine, called spinal surgeons.
Other specialists who care for people with spinal cord tumors include doctors who use medicine to treat cancer, called medical oncologists, and doctors who use radiation to treat cancer, called radiation oncologists.
Here's some information to help you get ready for your appointment.
What you can do
- Write down any symptoms you have and for how long.
- List your key health information, including all conditions you have and the names of any medicines you're taking.
- Note any family history of brain or spinal tumors, especially in a first-degree relative, such as a parent or sibling.
- Take a family member or friend along. Sometimes it can be difficult to remember all of the information you receive during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Write down questions to ask your healthcare professional.
Questions to ask at your initial appointment include:
- What may be causing my symptoms?
- Are there any other possible causes?
- What kinds of tests do I need? Do these tests require any special preparation?
- What do you recommend for next steps in determining my diagnosis and treatment?
- Should I see a specialist?
Questions to ask a specialist include:
- Do I have a spinal tumor?
- What type of tumor do I have?
- How will the tumor grow over time?
- What might be the consequences?
- What are the goals of my treatment?
- Am I a candidate for surgery? What are the risks?
- Am I a candidate for radiation? What are the risks?
- Will I need chemotherapy? What are the risks?
- What treatment approach do you recommend?
- If the first treatment isn't successful, what will we try next?
- What is the long-term outlook for my condition?
- Do I need a second opinion?
In addition to the questions that you've prepared, ask any additional questions that come up during your appointment.
What to expect from your doctor
Be prepared to answer some questions about your symptoms and your health history, such as:
- What are your symptoms?
- When did you first notice these symptoms?
- Have your symptoms gotten worse over time?
- If you have pain, where does the pain seem to start?
- Does the pain spread to other parts of your body?
- Have you experienced any weakness or numbness in your legs?
- Have you had any difficulty walking?
- Have you had any problems with your bladder or bowel function?
- Have you been diagnosed with any other medical conditions?
- Are you currently taking any medicines?
- Do you have any family history of spinal tumors?