Overview
Thyroid gland
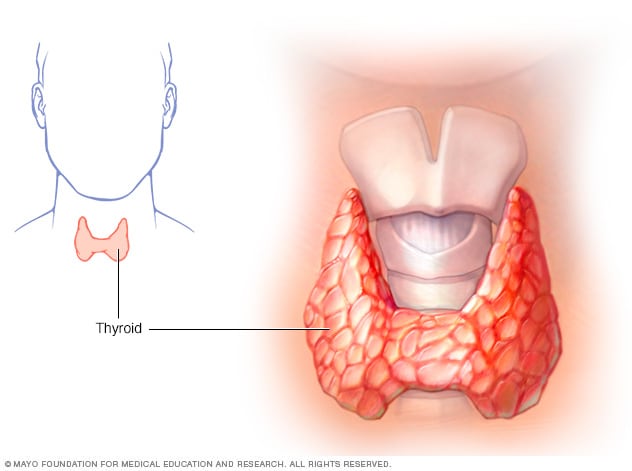
Thyroid gland
The thyroid gland sits at the base of your neck.
Thyroidectomy is surgery to remove all or part of the thyroid gland. The thyroid is a butterfly-shaped gland located in the front of the neck. It makes hormones that control every part of the metabolism, from the heart rate to how fast you burn calories.
Healthcare professionals perform thyroidectomy to treat thyroid conditions. These include:
- Cancer.
- Noncancerous enlargement of the thyroid, called a goiter.
- Overactive thyroid, called hyperthyroidism.
How much of the thyroid gland is removed during thyroidectomy depends on the reason for the surgery. If only part of your thyroid is removed, called a partial thyroidectomy, your thyroid may work as usual after surgery. If your entire thyroid is removed, called a total thyroidectomy, you'll need to take thyroid hormone medicine every day to replace your thyroid's natural function.
Why it's done
Your healthcare professional may recommend thyroidectomy if you have conditions such as:
- Thyroid cancer. Cancer is the most common reason for thyroidectomy. If you have thyroid cancer, most or all of the thyroid will likely be removed.
- Noncancerous enlargement of the thyroid, called a goiter. Removing all or part of your thyroid gland may be an option for a large goiter. A large goiter may be uncomfortable or make it hard to breathe or swallow. A goiter also may be removed if it's causing your thyroid to be overactive.
- Overactive thyroid. In an overactive thyroid, called hyperthyroidism, your thyroid gland makes too much of the hormone thyroxine. Thyroidectomy may be an option if antithyroid medicine or radioactive iodine doesn't work or isn't right for you. These are two other common treatments for hyperthyroidism.
- Suspicious thyroid nodules. A needle biopsy can provide more information about thyroid nodules. But sometimes it's not clear from the biopsy whether the nodules are cancer or not. If this happens, you may need surgery to find out. If your nodules are at higher risk of being cancer, you may be a candidate for thyroidectomy.
Risks
Thyroidectomy is generally safe. But as with any surgery, thyroidectomy has the risk of complications.
Potential complications include:
- Bleeding. Sometimes bleeding can block the airway, making it hard to breathe.
- Infection.
- Low parathyroid hormone levels, called hypoparathyroidism. Sometimes surgery damages the parathyroid glands behind the thyroid. The parathyroid glands control calcium levels in the blood. If blood calcium levels are too low, you may feel numbness, tingling or cramping.
- Permanent hoarse or weak voice due to nerve damage to the vocal cords.
How you prepare
Medicines and food
If you have hyperthyroidism, your healthcare professional may prescribe medicine such as iodine and potassium solution. Medicine can help control your thyroid function and lower the risk of bleeding after surgery.
To avoid anesthesia complications, you may need to avoid eating and drinking for a certain amount of time before surgery. Your healthcare professional will give you specific instructions.
Other precautions
Before the day of your surgery, ask a friend or loved one to help you get home after the procedure. Be sure to leave jewelry and valuables at home.
What you can expect
Before the surgery
Surgeons typically perform thyroidectomy using general anesthesia, so you won't be awake during the procedure. The anesthesiologist or anesthetist gives you an anesthetic as a gas to breathe through a mask or injects a liquid medicine into a vein. After you're in a sleeplike state, a breathing tube will be placed in your windpipe, called the trachea, to help you breathe throughout the procedure.
The surgical team places several monitors on your body to check your heart rate, blood pressure and blood oxygen level throughout the surgery. These monitors include a blood pressure cuff on your arm and heart-monitor leads attached to your chest.
During the surgery
Once you're unconscious, the surgeon makes a cut, called an incision, low in the center of your neck. It can often be placed in a skin crease where it will be hard to see after the incision heals. All or part of the thyroid gland is then removed, depending on the reason for the surgery.
If you're having thyroidectomy because of thyroid cancer, the surgeon also may examine and remove lymph nodes around your thyroid. In some people, the surgeon uses special equipment to monitor irritation of vocal cords during the surgery to prevent permanent damage. Thyroidectomy usually takes 1 to 2 hours. It may take more or less time, depending on the extent of the surgery.
There are several approaches to thyroidectomy, including:
- Conventional thyroidectomy. This approach involves making a cut, called an incision, in the center of the neck to directly access the thyroid gland. The majority of people will likely be candidates for this procedure.
- Transoral thyroidectomy. This approach accesses the thyroid through a cut inside the mouth.
- Endoscopic thyroidectomy. This approach uses smaller cuts in the neck. Your surgeon inserts surgical instruments and a small video camera through the cuts. The camera guides your surgeon during the procedure.
After the surgery
After surgery, you're moved to a recovery room where healthcare professionals monitor your recovery from the surgery and anesthesia.
Some people may need to have a drain placed under the cut in the neck. This drain is usually removed the day after surgery.
After thyroidectomy, some people may have neck pain and a hoarse or weak voice. These symptoms typically last for only a short time. They may be due to irritation from the breathing tube inserted into the windpipe during surgery or from nerve irritation caused by the procedure. Sometimes the hoarseness or weakness is caused by permanent damage to the vocal cords.
You'll be able to eat and drink as usual after surgery. Depending on the type of surgery you had, you may be able to go home the day of your surgery or stay overnight in the hospital.
When you go home, you can usually return to your regular activities. Wait at least 10 to 14 days before doing anything strenuous, such as heavy lifting or high-impact sports.
It takes up to a year for the surgical scar to fade. Your healthcare professional may recommend using sunscreen to make the scar less visible.
Results
The long-term effects of thyroidectomy depend on how much of the thyroid is removed.
Partial thyroidectomy
If only part of the thyroid is removed, the remaining portion typically takes over the function of the entire thyroid gland. So you might not need thyroid hormone therapy.
Complete thyroidectomy
If your entire thyroid is removed, your body can no longer make thyroid hormone. Without medicine, you'll develop symptoms of underactive thyroid, called hypothyroidism. These symptoms may include dry skin, tiredness and weight gain. You'll need to take a daily pill with the synthetic thyroid hormone levothyroxine (Synthroid, Unithroid, others).
This hormone replacement is the same as the hormone usually made by the thyroid gland and performs all of the same functions. Your healthcare professional will test your blood to know how much thyroid hormone replacement you need.
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.