Overview
Healthy shoulder joint
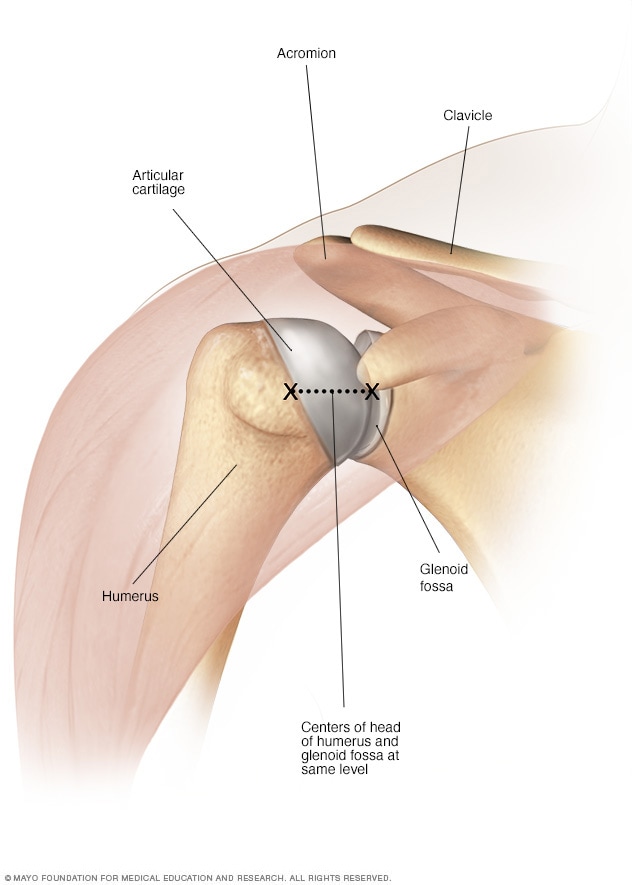
Healthy shoulder joint
In a healthy shoulder joint, the round head of the upper arm bone fits into a shallow socket in the shoulder.
Anatomic total shoulder replacement
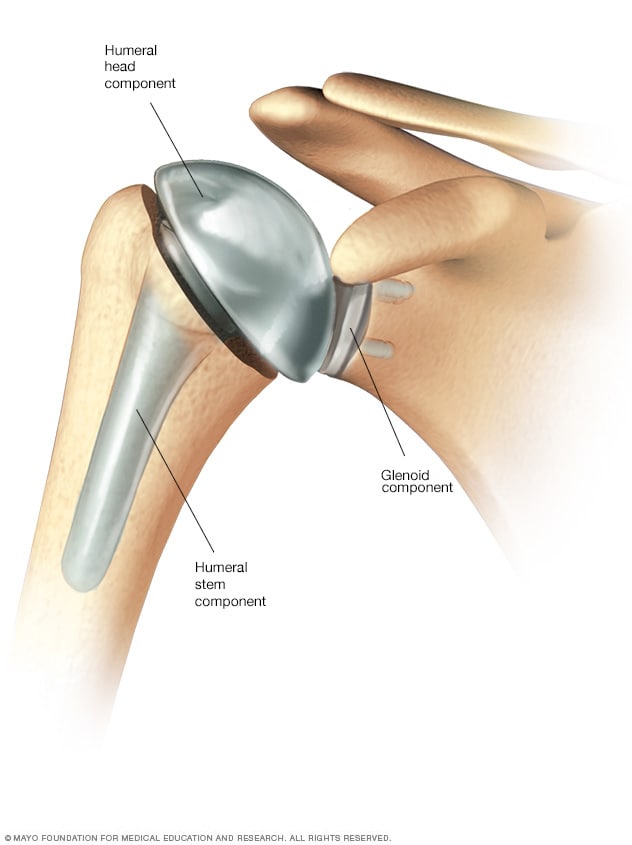
Anatomic total shoulder replacement
In an anatomic total shoulder replacement, the ball and the socket are replaced with implants that resemble the natural shape of the bones.
Reverse total shoulder replacement
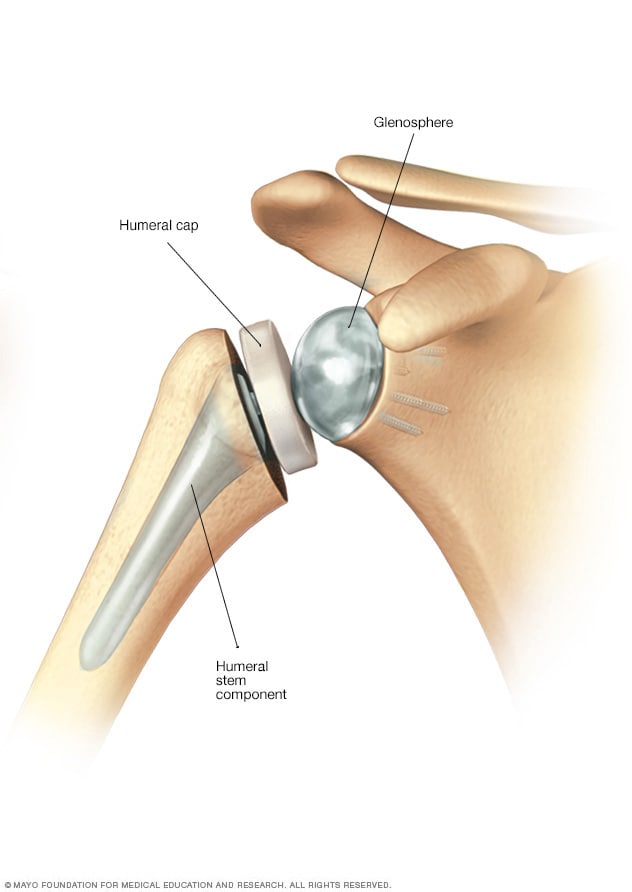
Reverse total shoulder replacement
In a reverse total shoulder replacement, the ball implant is attached to the shoulder blade and the socket is attached to the upper arm bone.
Shoulder replacement surgery also is called shoulder arthroplasty (ARTH-row-plas-tee). In this surgery, the damaged parts of the shoulder are removed and replaced with new parts. These new parts, called implants, typically are made of metal and plastic.
The shoulder is a ball-and-socket joint. The top of the upper arm bone is shaped like a ball. It fits into a shallow socket in the shoulder. Damage to this joint can cause pain, weakness and stiffness.
There are different types of shoulder implants. Some people need only part of the joint replaced, while others need the whole joint replaced. Some implants are shaped like the human shoulder. These are called anatomic replacements. Other implants may reverse the positions of the ball and socket. These are called reverse replacements.
Why it's done
Shoulder replacement surgery is done to relieve pain, stiffness and other symptoms caused by damage to the shoulder joint.
Conditions that can damage the joint include:
- Osteoarthritis. Also called wear-and-tear arthritis, this condition damages the cartilage that covers the ends of bones and helps joints move smoothly. Without this cushion of cartilage, the joint becomes stiff and painful.
- Rotator cuff injuries. The rotator cuff is a group of muscles and tendons that help move and support the shoulder. Serious injuries to the rotator cuff also can lead to damage to the cartilage and bone in the shoulder joint.
- Fractures. A broken upper arm bone may need to be replaced if it is seriously damaged in an accident. It also may need to be replaced if an earlier injury didn't heal properly or if earlier surgery to fix a break didn't work.
- Rheumatoid arthritis and other inflammatory conditions. These conditions are caused by an overactive immune system. Inflammation from rheumatoid arthritis and other inflammatory conditions can damage the cartilage. Sometimes these conditions also can damage the underlying bone in the joint and the surrounding rotator cuff muscles.
- Osteonecrosis. This condition happens when a bone doesn't get enough blood. Some shoulder conditions reduce blood flow to the upper arm bone, called the humerus. Without enough blood, the bone may weaken and collapse.
Shoulder replacement procedures
There are different types of shoulder replacement surgeries. The right option for you depends on which parts of the joint are damaged and how well your muscles and tendons are working.
- Anatomic total shoulder replacement. Both the ball and the socket are replaced. The implants resemble the natural shape of the bones.
- Reverse total shoulder replacement. Both the ball and the socket are replaced, but the positions are switched. The ball is attached to the shoulder blade, and the socket is attached to the upper arm bone. This typically is done when the rotator cuff is seriously damaged.
- Partial shoulder replacement. Hemiarthroplasty is the medical term for partial shoulder replacement. Only the ball of the shoulder joint is replaced. This may be a good option if the socket is still healthy and only the ball is damaged.
Reverse total shoulder replacement
Reverse shoulder replacement may be a better way to improve the joints function and reduce pain, especially if the joint is affected by arthritis. This operation is also called reverse arthroplasty. Artho means joint. Plasty means to mold surgically.
The top of the arm bone fits into a socket on the shoulder blade. In a typical shoulder replacement, a plastic lining is attached to the socket to allow smooth movement. The surgeon removes the top of the arm bone and inserts a metal stem with a ball on the end. However, if the rotator cuff is severely damaged, the joint may not be stable or work properly.
In a reverse shoulder replacement, the normal ball and socket structure is reversed. An artificial ball is attached to the shoulder blade. An artificial socket is attached to the top of the arm bone. The large deltoid muscle that covers the shoulder is typically able to move the arm.
Partial shoulder replacement
In some people, the top of the arm bone needs to be replaced, but the socket is still in good shape. In others, the bone in the socket is too worn out and not strong enough to hold a new lining. In these cases an operation called a hemiarthroplasty may be the best option. Hemi means partial.
As seen before, the surgeon exposes the joint, prepares the top of the arm bone and inserts a metal stem with a ball on the end. If the socket is worn out, the surgeon smooths and reshapes it. The arm bone is then put back in place.
Risks
In most cases, shoulder replacement surgery helps lessen pain and improve movement. But sometimes it may not fully relieve pain or restore the shoulder's strength and motion. Rarely, additional surgery may be needed.
Although complications are rare, it's important to understand the risks. These may include:
- Dislocation. The new ball can slip out of the socket.
- Fracture. Bones in the shoulder can break during or after surgery. This includes the upper arm bone, called the humerus bone. It also includes the shoulder blade, called the scapula, and the socket bone, called the glenoid.
- Implant loosening or wear. Over time, the artificial parts may loosen or wear out. If that happens, another surgery may be needed to replace them.
- Rotator cuff failure. The muscles and tendons that support the shoulder joint are called the rotator cuff. The rotator cuff can sometimes tear or wear out after a partial or total anatomic shoulder replacement.
- Nerve damage. Nearby nerves can be injured during surgery. This may cause numbness, weakness and pain in the arm or shoulder.
- Blood clots. Clots may form in the veins of the leg or arm after surgery. If a piece of the clot travels to the lungs, the heart or, rarely, the brain, it can lead to serious health issues.
- Infection. Infections can occur at the incision site or deeper in the shoulder. Sometimes another surgery is needed to treat the infection.
How you prepare
Before surgery is scheduled, you'll meet with your surgeon for an evaluation. This visit typically includes:
- A review of your symptoms.
- A physical exam.
- Imaging tests such as X-rays or a CT scan of your shoulder.
Some questions you may want to ask include:
- What type of shoulder replacement surgery do you recommend?
- How will I manage my pain after surgery?
- How long will I need to wear a sling?
- What kind of physical therapy will I need?
- What activities should I avoid after surgery?
- Will I need help at home while I recover?
Other members of the healthcare team also talk with you to make sure you are ready for surgery. They ask about your medical history, any medicines you take, and whether you use tobacco or are regularly exposed to secondhand smoke. Tobacco slows healing.
You may meet with a physical therapist who teaches you exercises to help with your recovery. The physical therapist also may show you how to use a sling, called an immobilizer, that keeps your shoulder from moving after surgery.
Many people go home the same day as their shoulder replacement surgery.
More information
Outpatient joint replacement: Is it a safe option?
What you can expect
Before the procedure
Your surgeon will give you instructions about how to prepare for surgery. This may include when to stop eating and drinking, how to bathe or clean the surgical area, and which medicines to take or avoid the day before and the day of surgery. Follow these directions carefully.
During the procedure
Before surgery, a member of your care team will explain how you'll be sedated. Most people get general anesthesia and a nerve block. General anesthesia puts you into a deep sleep during surgery. The nerve block numbs your shoulder and helps manage pain even after you wake up. The surgery usually takes 1 to 2 hours.
After the procedure
After surgery, you'll rest in a recovery area for a short time. You will have X-rays taken of your shoulder. Your shoulder will be in a type of sling called an immobilizer. Don't try to move your shoulder unless your care team says it's OK.
How long you stay in the hospital after surgery depends on your specific situation. Most people go home the same day.
Your shoulder replacement surgery at Mayo Clinic
If you're planning to have shoulder replacement surgery at Mayo Clinic, the following resources will explain what to expect and how to prepare.
Results
After shoulder replacement, most people feel less pain than they did before surgery. Many have no pain at all. And most people have improved shoulder movement and strength, making it easier to do everyday activities.
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.