Overview
Laminectomy
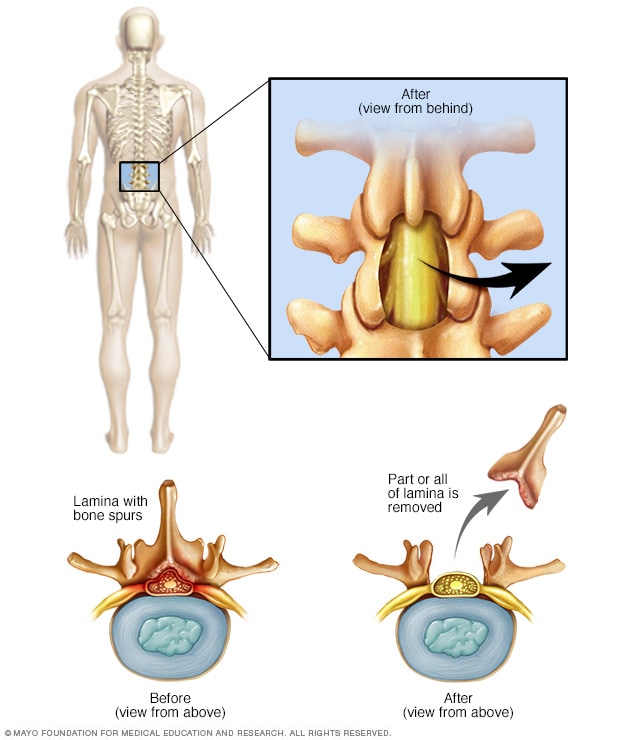
Laminectomy
A lumbar laminectomy involves the removal of the back part of a vertebra in your lower back to make more room within the spinal canal.
Cervical laminectomy
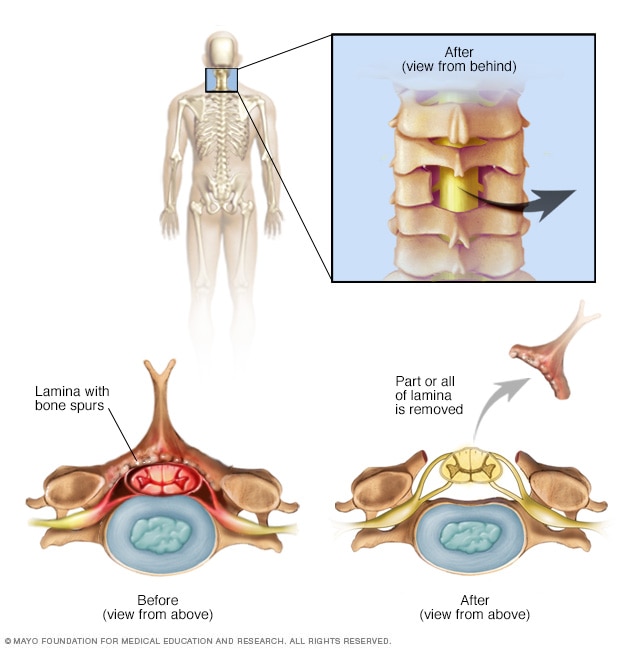
Cervical laminectomy
A cervical laminectomy involves the removal of the back part of a vertebra in your neck to make more room within the spinal canal.
Laminectomy is surgery to remove the back arch or part of a spinal bone. This part of the bone, called the lamina, covers the spinal canal. Laminectomy enlarges the spinal canal to ease pressure on the spinal cord or nerves. Laminectomy is often done as part of a decompression surgery to relieve pressure.
Pressure in the spinal canal is most commonly caused by bony overgrowths within the spinal canal. These overgrowths are sometimes called bone spurs. These overgrowths are a side effect of aging and can happen in people who have arthritis in their spines. Some people are more likely to have bone spurs because of genetic traits passed down in their families.
Laminectomy is generally used only when more-conservative treatments, such as medicines, physical therapy or injections, have failed to relieve symptoms. Laminectomy also might be recommended if symptoms are severe or getting much worse.
Why it's done
Bony overgrowths of the joints in the spine can build up within the spinal canal. They can narrow the space for the spinal cord and nerves. This pressure can cause pain, weakness or numbness that can radiate down arms or legs.
Because laminectomy restores spinal canal space, it's likely to relieve the pressure that causes the radiating pain. But the procedure doesn't cure the arthritis that caused the narrowing. So, it's not likely to relieve back pain.
A healthcare professional might recommend laminectomy if:
- Conservative treatment, such as medicines or physical therapy, fails to improve symptoms.
- Muscle weakness or numbness makes it hard to stand or walk.
- Symptoms include loss of bowel or bladder control.
In some situations, laminectomy may be a part of surgery to treat a herniated spinal disk. A surgeon may need to remove part of the lamina to get to the damaged disk.
Risks
Laminectomy is generally safe. But as with any surgery, complications can occur. Potential complications include:
- Bleeding.
- Infection.
- Blood clots.
- Nerve injury.
- Spinal fluid leak.
How you prepare
You'll need to avoid eating and drinking for a certain amount of time before surgery. Your healthcare team can give you instructions about the types of medicines you should and shouldn't take before your surgery.
What you can expect
During laminectomy
Surgeons usually perform laminectomy using general anesthesia, so you're not awake during the surgery.
The surgical team monitors heart rate, blood pressure and blood oxygen levels throughout the procedure. After you are in a sleep-like state and can't feel pain:
- The surgeon makes an incision in your back over the affected vertebrae and moves the muscles away from your spine as needed. The surgeon uses small instruments to remove the bone spurs and the smallest amount of lamina possible. The size of the incision may vary depending on your condition and body size. Minimally invasive surgeries often use smaller incisions than those used for open procedures.
- If laminectomy is being performed as part of surgery for a herniated disk, the surgeon also removes the herniated portion of the disk and any pieces that have broken loose. This is called a diskectomy.
- For a vertebra that has slipped over another or for curvature of the spine, spinal fusion might be needed to stabilize the spine. During spinal fusion, the surgeon permanently joins two or more of the vertebrae after removing the arthritic joints. The surgery might involve the use of bone grafts and, if needed, metal rods and screws.
- Depending on your condition and your needs, the surgeon may do minimally invasive surgery. For this procedure, the surgeon makes a smaller incision and uses a special surgical microscope.
After laminectomy
After surgery, you're moved to a recovery room where the healthcare team watches for complications from the surgery and anesthesia. You may be asked to move your arms and legs. Your healthcare professional may prescribe medicine to relieve pain at the incision site.
You're likely to spend a night or two in the hospital. Your care team might recommend physical therapy after a laminectomy to improve your strength and flexibility.
Depending on the amount of lifting, walking and sitting your job involves, you may be able to return to work within a few weeks. If you also have spinal fusion, your recovery time will be longer.
Results
Most people report improvement in their symptoms after laminectomy, especially a decrease in pain that radiates down the leg or arm. But this benefit may lessen over time with some forms of arthritis. Laminectomy is less likely to improve pain in the back itself.
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.