Overview
Adrenal glands
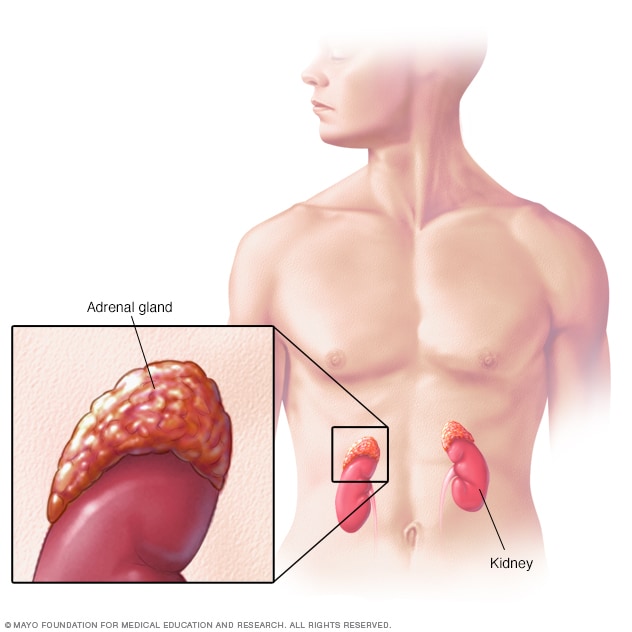
Adrenal glands
Located on top of the kidneys, the adrenal glands make hormones that help regulate metabolism, the immune system, blood pressure and other important functions. Although small, these glands control much of what happens in the body.
An adrenalectomy (uh-dree-nul-EK-tuh-me) is surgery to remove one or both of the adrenal glands.
The body's two adrenal glands are located at the top of each kidney. The adrenal glands are part of the system that makes hormones, called the endocrine system. Although adrenal glands are small, they make hormones that affect almost every part of the body. These hormones control metabolism, the immune system, blood pressure, blood sugar and other important body functions.
An adrenalectomy often is done to remove a tumor. Most of these tumors are benign. That means they are not cancer. Cancer that begins in the adrenal glands is not common. The surgery also may be done because an adrenal gland makes too much of certain hormones. Or an adrenalectomy may be needed if cancer has spread to an adrenal gland from another part of the body.
If only one gland is removed, and it was not making too many hormones, the other takes over the work of both adrenal glands after surgery. In that situation, hormone replacement medicine is not needed. If an adrenal gland is removed because it is making too many hormones, you may need to take hormone replacement medicine until the other adrenal gland starts working correctly again. If both adrenal glands are removed, you need to take medicine for the rest of your life to replace the hormones that the glands make.
Products & Services
Why it's done
You may need an adrenalectomy if one or both of your adrenal glands:
- Contain a tumor. Adrenal gland tumors that are cancer are called malignant tumors. Tumors that are not cancer are called benign tumors. Most adrenal gland tumors are not cancer.
- Make too many hormones. If an adrenal gland makes too many hormones, it can cause a wide range of symptoms that may lead to serious health problems. In some cases, certain types of tumors can trigger the glands to make extra hormones. They include tumors called pheochromocytomas and aldosteronomas. Some tumors cause the gland to make too much of the hormone cortisol. That leads to a condition called Cushing syndrome. A tumor in the pituitary gland also can trigger the adrenal glands to make too much cortisol. If the pituitary tumor cannot be completely removed, an adrenalectomy may be necessary.
In some cases, an adrenalectomy also may be advised if an imaging exam of the adrenal glands, such as a CT scan or an MRI scan, show suspicious or unclear findings.
Risks
Adrenalectomy has the same risks as other major surgeries — bleeding, infection and a bad reaction to the anesthesia. Other possible risks include:
- Injury to organs close to the adrenal gland.
- Blood clots.
- Pneumonia.
- Blood pressure changes.
- Not enough hormones in the body after surgery.
For some people, the health problem that led to an adrenalectomy may return after surgery, or the surgery may not resolve it completely.
How you prepare
For a period of time before surgery, you may need to have your blood pressure checked often. You may need to follow a special diet and take medicine. You also may need imaging tests to help your care team prepare for the surgery. If your body is making too many hormones, you may need to follow specific preparations before surgery to make sure the procedure can be done safely.
Just before the surgery, you may need to avoid eating and drinking for a certain period of time. Your health care provider will give you specific instructions. Before your surgery, ask a friend or family member to help you get home after the procedure.
What you can expect
During the procedure
Adrenalectomy is done using general anesthesia. This means you are in a sleep-like state during surgery.
Surgeons may perform an adrenalectomy using a minimally invasive approach, or they may use open surgery.
Minimally invasive surgery
This surgical approach has many benefits, including smaller scars, less pain and less recovery time than open surgery. It often can be used for an adrenalectomy because the adrenal glands are small. Minimally invasive surgery also is called laparoscopic surgery, posterior retroperitoneoscopic surgery (PRA) or robotic surgery. During minimally invasive surgery, the surgeon makes 1 to 4 small cuts, called incisions, in the abdomen or back.
- Laparoscopic surgery. In laparoscopic surgery, the surgeon places a small camera, called a laparoscope, through one of the incisions in the abdomen. It's used to view the internal organs and guide the surgery. Through the other incisions, the surgeon inserts instruments that are used to remove the adrenal gland.
- Posterior retroperitoneoscopic surgery (PRA). With this approach, the surgeon also uses a small camera and small incisions. But the incisions are made on the back. The adrenal gland is removed through them.
- Robotic surgery. Robot-assisted procedures can be used to perform laparoscopic adrenalectomies. This approach is similar to other laparoscopic surgeries, except it may need only one or two incisions. Instead of the surgeon moving the surgical instruments by hand, the instruments are attached to mechanical arms. The surgeon controls the arms while seated at a computer console near the operating table.
Open surgery
During an open adrenalectomy, the adrenal gland is removed through one cut in the front of the abdomen. The location of the cut depends on tumor size, tumor type and a person's body type. Open surgery typically is used for large tumors and tumors that have spread to other tissues. It also may be used if there is scar tissue near the adrenal gland from other surgeries, or if obesity is a concern.
The surgery used for adrenalectomy depends on the condition that's affecting your adrenal gland as well as your health and medical history. If there's a tumor in your adrenal gland, the size and type of tumor will make a difference too. Talk to your health care team about the approach that's right for you.
After the procedure
The length of the hospital stay after adrenalectomy depends on the type of surgery. Most people who have minimally invasive surgery either go home the same day as the surgery or spend one night in the hospital. If open surgery is used, the hospital stay may be 3 to 5 days.
Results
The adrenal gland removed during surgery is sent to a laboratory to be examined. Specialists called pathologists study the gland and tissue. They report what they learn to your health care provider. After surgery, you talk with your provider about the pathologist's report and any follow-up care you may need.
Most people have only one adrenal gland removed. In that case, the remaining adrenal gland takes over the work of both adrenal glands. If one adrenal gland is removed because it's making too much of certain hormones, you may need to take hormone replacement medicine until the other adrenal gland starts working correctly again. If both adrenal glands are removed, you need to take medicine for the rest of your life to replace the hormones that the glands make.
Dec. 23, 2025