Feb. 09, 2019
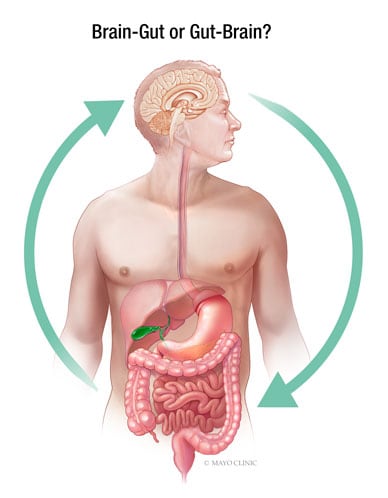
Adult functional gastrointestinal disorders (FGIDs) are brain-gut interaction disorders that affect about 1 out of every 4 adults and have a significant negative impact on quality of life, work productivity and health care costs.
Irritable bowel syndrome (IBS) is one of the most common forms of FGIDs and is estimated to affect 1 out of 7 adults in the United States. This disorder is characterized by continuous or recurrent abdominal pain or discomfort associated with altered bowel habits, with no evidence of an organic disorder (such as an ulcer or a blockage), a structural abnormality or another cause for chronic GI symptoms when testing (such as bloodwork, X-rays or endoscopy) is performed. There are three distinct subtypes of IBS, which are categorized based on bowel habits:
- Constipation predominant (IBS-C)
- Diarrhea predominant (IBS-D)
- Mixed type (IBS-M)
In this article, Mayo gastroenterologists discuss the Mayo Clinic experience and recent research findings related to the use of dietary interventions and other nonpharmacological measures in managing IBS and other types of FGIDs.
Dietary measures
The majority of individuals with IBS note that symptoms begin or worsen after eating a meal. Individuals with diarrhea-predominant IBS experience an exaggerated gastrocolonic motor response to ingestion of food that causes postprandial pain and rectal urgency. Although individuals with IBS do not commonly have true food allergies, sensitivities to foods are reported by nearly half of patients. A growing number of studies have examined the role of dietary factors in IBS and suggest that dietary modifications might help prevent or reduce symptoms.
Fiber supplementation
Supplementation with a soluble fiber preparation, such as psyllium, is still regarded as an effective initial approach to the management of constipation-predominant IBS. Providers should have patients increase the dose gradually, while reminding them that it may take up to 12 weeks for evidence of results.
Brian E. Lacy, M.D., Ph.D., and co-authors affirmed the efficacy of dietary fiber in managing IBS in an American College of Gastroenterology monograph on IBS management published in The American Journal of Gastroenterology in 2018. Dr. Lacy is a gastroenterologist at Mayo Clinic's campus in Florida. "The low cost and lack of significant side effects make soluble fiber a reasonable first line therapy for IBS patients," says Dr. Lacy.
Probiotics
Multiple randomized controlled trials have established that probiotics have beneficial effects on global symptoms and on bloating and flatulence in individuals with IBS. Adil E. Bharucha, M.B.B.S., M.D., a gastroenterologist at Mayo Clinic's campus in Rochester, Minnesota, co-authored a comprehensive review article about FGIDs associated with abdominal pain published in Mayo Clinic Proceedings in 2016. In a discussion about the role of dietary measures, Dr. Bharucha and co-authors note that although Bifidobacterium infantis improves abdominal pain and reduces defecation difficulty significantly, it does not affect stool frequency or consistency.
Gluten and FODMAPs
Gluten and fermentable oligosaccharides, disaccharides, monosaccharides and polyols (FODMAPs) have recently gained attention as a possible dietary trigger for IBS symptoms. FODMAPs are short-chain carbohydrates present in stone fruits, legumes, lactose-containing foods and artificial sweeteners.
In an article published in The American Journal of Gastroenterology in 2018, Dr. Lacy and co-authors share the results of a systematic review and meta-analysis of randomized controlled trials (RCTs) examining the efficacy of gluten-free diets (GFDs) and low-FODMAP diets as a treatment for IBS. These diets are among the most common diets recommended by health care professionals to improve IBS symptoms.
The researchers analyzed two RCTs of a GFD in 111 participants, and seven RCTs that compared a low-FODMAP diet with various control interventions in 397 participants. This review concluded that these trials provided insufficient evidence that a GFD or low-FODMAP diet was effective in reducing IBS symptoms.
According to Dr. Lacy, the evidence supporting the use of a GFD was not statistically significant. "Our analysis noted that these trials were relatively small, subject to a high risk of bias and that, overall, the evidence was low in quality according to GRADE criteria. The three RCTs that compared a low-FODMAP diet with rigorous control diets had the least heterogeneity between studies, but also the least magnitude of effect," says Dr. Lacy.
Some researchers have expressed concern that restricted diets could cause problems with prolonged use. These problems might involve nutritional deficiencies or unforeseen changes in the colonic microbiome. While more data is needed on this topic, Dr. Lacy notes that one study presented at the ACG 2017 Annual Scientific Meeting produced some interesting results. The study compared the impact of low-FODMAP diets and modified National Institute for Health and Care Excellence (mNICE) diets on IBS symptoms over a four-week period and concluded that the low-FODMAP diet may be associated with major micronutrient inadequacies.
Despite the limitations of the available study data about the efficacy and safety of specific dietary modifications, many experts believe that working with patients to monitor their diets and make dietary modifications still has value. But Dr. Lacy cautions that dietary modifications should be undertaken with care. "Given the limited studies and lack of long-term data, we need to provide careful advice and, ideally, use a multidisciplinary team approach that includes a dietitian," says Dr. Lacy.
Mayo FGIDs specialists recommend having patients keep a detailed log of daily dietary intake to aid in identifying particular foods that aggravate symptoms. Clinicians can consider an initial trial of an individual dietary intervention if certain foods (such as fructans or gluten) appear to be triggers. Patients who continue to have persistent symptoms while a trial is underway or patients who can't identify any possible triggers can try a four-week trial low-FODMAP diet with the consultation of a dietitian. The dietitian can help tailor the specific therapy to each individual and create menus that comply with any dietary restrictions.
In partnership with investigators at Arizona State University, Mayo Clinic gastrointestinal motility thought leaders are conducting research on the physical role of the gut microbiome and the gut-brain axis in FGIDs. Ongoing research efforts are addressing the interplay of nutrients and the gut microbiome, and assessing the impact of treating gut dysbiosis to search for ideal dietary and supplemental recommendations for patients on their journey to wellness.
Psychological and behavioral approaches
Effective patient-physician relationship
Dr. Bharucha notes that establishing an effective patient-physician relationship is important, because many individuals with functional GI disorders feel abandoned and undertreated and seek care from multiple doctors with limited success. "We need to approach these patients with empathy and provide reassurance through appropriate testing that their condition is not life-threatening. We also need to educate them about the disease, set reasonable expectations for treatment and engage them in managing their condition."
Assess coexisting psychological factors
Assess coexisting psychological factors
During evaluation it is important to assess coexisting psychological factors, including anxiety, depression, somatization and catastrophization.
Dr. Bharucha and co-authors note that life experiences during childhood and adulthood, lack of social support, and other social factors can lead to maladaptive earned-illness behaviors and predispose some individuals to functional GI and psychiatric disorders. This means that a history of verbal, sexual or physical abuse or major life stressors such as bereavement or divorce may factor into the management of FGIDs in some patients.
Psychological and physical interventions
Individuals with a history of life stressors may benefit from psychological and behavioral interventions, tailored to the symptoms, functional impairment, psychological distress and symptom expression. The goals of these interventions include pain management, improvement in daily function and relief from psychological distress. Dr. Bharucha and co-authors noted that a meta-analysis of 41 trials involving 2,290 patients observed that psychological therapy is moderately effective for improving IBS symptoms for up to one year after therapy.
"Cognitive behavioral therapy can help patients relax, provide a sense of control over symptoms and induce more parasympathetic activity," explains Dr. Bharucha. "Diaphragmatic breathing exercises can help patients reduce belching, regurgitation and vomiting."
According to Tisha N. Lunsford, M.D., a gastroenterologist at Mayo Clinic's campus in Arizona, a variety of personality traits, including neuroticism, emotional hypersensitivity, maladaptive stress, coping and aggression, have been shown to be associated with poorer health care quality of life and therapeutic outcomes following both psychological and pharmacological treatments. Dr. Lunsford co-authored a 2010 article in Clinical Gastroenterology and Hepatology that explores this dynamic in patients with FGIDs.
"Our results confirmed our primary hypothesis that a clinically meaningful subset of patients with FGIDs test positive for the Type D personality trait," explains Dr. Lunsford. "Consideration of personality traits may allow for improved risk stratification in research and in planning treatment for these individuals."
Various psychological and physical therapies appear to be safe and effective in FGIDs but may not be widely available. Led by integrative medicine practitioners at Mayo Clinic's campus in Arizona, physicians, nurses, dietitians, psychologists, physical therapists, acupuncturists and massage therapists, as well as instructors in movement classes such as yoga and tai chi, are committed to providing therapies that have been researched and have scientific evidence to support them.
"For more than a decade, Mayo Clinic physicians have been integrating complementary and alternative therapies with conventional care to meet the emotional, spiritual and psychological needs of the patient and to complement addressing physical symptoms," explains Dr. Lunsford. "Integrative medicine reaffirms the importance of the relationship between practitioner and patient, focuses on the whole person, is informed by evidence, and makes use of all appropriate therapeutic approaches, health care professionals and disciplines to achieve optimal health and healing."
For more information
Ford AC, et al. American College of Gastroenterology monograph on management of irritable bowel syndrome. The American Journal of Gastroenterology. 2018;113(suppl 2):1.
Bharucha AE, et al. Common functional gastroenterological disorders associated with abdominal pain. Mayo Clinic Proceedings. 2016;91:1118.
Dionne J, et al. A systematic review and meta-analysis evaluating the efficacy of a gluten-free diet and a low FODMAPs diet in treating symptoms of irritable bowel syndrome. The American Journal of Gastroenterology. 2018;113:1290.
Farida JP, et al. P2011 — Micronutrient intake changes with the low FODMAP and mNICE diets. Presentation at: ACG 2017 Annual Scientific Meeting; 2017; Orlando, Fla.
Hansel SL, et al. Personality traits and impaired health-related quality of life in patients with functional gastrointestinal disorders. Clinical Gastroenterology and Hepatology. 2010;8:220.