April 01, 2016
Cardiovascular disease (CVD) is the leading cause of death in the United States, where up to 60 percent of adults will have a myocardial infarction, stroke or incident of heart failure in their lifetimes. Despite these striking numbers, research data suggest that CVD is largely preventable. Individuals with an optimal risk profile — collectively named "Life's Simple 7" by the American Heart Association — have as much as an 80 percent reduction in risk of CVD.
Cholesterol and CVD risk
Six of Life's Simple 7 (healthy diet, physical activity, no smoking, and well-controlled blood pressure, blood glucose and body weight) can be universally recommended by clinicians. However, the seventh item (cholesterol level) is a challenge because the optimal level is primarily determined by an individual's risk of CVD.
National guidelines recommend the use of population-based risk algorithms, such as the Pooled Cohort Risk Assessment Equations, to determine atherosclerotic cardiovascular risk (ASCVD). "These risk algorithms are remarkably effective in predicting risk in populations, but have limitations in predicting individual risk," says R Todd Hurst, M.D., director of the Heart Health and Performance Program at Mayo Clinic's campus in Phoenix/Scottsdale, Arizona. "The best illustration of these limitations is that the majority of CVD events (up to 75 percent) occur in low- and intermediate-risk populations."
Because more-accurate means of determining individual CVD risk are needed, a search is ongoing for better tools to identify high-risk individuals before clinical events occur. One such tool is imaging for subclinical atherosclerosis, most commonly accomplished by quantifying the amount of calcium in the coronary arteries by computerized tomography.
Subclinical atherosclerosis and CVD risk prediction
The coronary artery calcium score (CACS) is strongly correlated with future risk of myocardial infarction and stroke, making it a potentially attractive tool to further clarify individual risk of CVD. Several large studies with long-term follow-up have shown that CACS adds incremental information in CVD risk identification and provides more-accurate CVD risk prediction compared with traditional risk factors in about 25 percent of individuals.
Despite the potential utility of these data, it is not known if identifying individuals who are at higher risk by CACS — and intensifying the prevention regimen — lowers the risk of CVD events. That question has not been adequately studied.
A case: Statin or no statin?
A 50-year-old African-American man, known in this case study as Smith, presents with concerns regarding cardiovascular risk. He has no personal history of CVD. He is active and asymptomatic and takes no medication. He is not a current smoker. His blood pressure is 134/82 mm Hg, and he has a total cholesterol level of 212 mg/dL, a high-density lipoprotein cholesterol level of 54 mg/dL, triglycerides of 92 mg/dL, and a calculated low-density lipoprotein cholesterol level of 140 mg/dL. His 10-year risk, as determined by the ASCVD Pooled Cohort Risk Assessment Equations, is 5.7 percent.
Smith notes that his 52-year-old brother recently had coronary artery bypass graft surgery and his father died of a myocardial infarction at 55 years of age but feels their health problems were primarily due to long-term tobacco abuse.
Smith leads a healthy lifestyle but is wondering if he should consider taking a statin medication to further lower his risk of CVD.
The "2013 American College of Cardiology/American Heart Association Guideline on the Treatment of Blood Cholesterol to Reduce Atherosclerotic Cardiovascular Risk in Adults" recommends shared decision-making about the benefits and risks of a statin medication for primary prevention when the 10-year risk is 7.5 percent or higher in an adult who does not have diabetes.
In addition, the guidelines state that CACS, as well as ankle-brachial index (ABI), high-sensitivity C-reactive protein (hs-CRP), and family history of premature CVD may be considered (Class IIb) to inform treatment decision-making.
However, the guidelines do not make specific recommendations on how these tools should be used. Thus, according to the guidelines, in the case of Smith, it would be reasonable for a clinician to take one of the following actions:
- Not recommend a statin because the patient's 10-year ASCVD risk is less than 7.5 percent
- Recommend a statin on the basis of the patient's family history of premature CVD and his moderately elevated 10-year risk score
- Seek further information such as CACS, ABI or hs-CRP to help guide the decision
Clinicians who seek additional information want to know whether Smith is at higher risk than would be predicted by risk factors due to genetic disposition for atherosclerosis. Following this line of thought, a high-risk CACS result indicates that a statin medication should be considered. If a low-risk result is obtained, reassurance and continued emphasis on lifestyle measures should be recommended.
What patient should not have a CACS?
The appropriate patient for CACS is still debated, and the answer to this question will likely continue to evolve as data accumulate. However, there is more agreement among experts in CVD prevention concerning patients for whom CACS is rarely indicated:
- Patients with clinical CVD or those already taking a statin medication
- Patient scenarios where both the clinician and the patient agree that a statin is indicated
- Patient scenarios where both the clinician and the patient agree that a statin is not indicated
- Patients who have had previous CACS to assess the response to treatment
What patient should have a CACS?
While there is not enough evidence to make a recommendation without reservation to perform CACS in any patient, many clinicians who specialize in CVD prevention (including those at Mayo Clinic) believe that CACS can add valuable clinical information in selected patients.
At Mayo Clinic's campus in Arizona, the most common indication for CACS is lack of a decision by the patient, the clinician or both about whether to start a statin for CVD risk reduction. In such a situation, the imaging study can further clarify the patient's risk and, by extension, whether a statin medication should be considered.
There are several common clinical scenarios where the individual's risk of future CVD is uncertain:
Family history of CVD
Family history is often the most difficult CVD risk factor to assess. Although it is clear that family history is an important determinant of risk, the complex interplay between genetic factors, environmental exposure and lifestyle choices often makes confident assessment of an individual's risk impossible. In this situation, CACS may help determine if the patient has a genetic disposition to atherosclerosis.
Striking risk factor in a young patient
Because age is the most heavily weighted factor in population-based risk algorithms, younger patients (younger than 60 years) are less likely to be high risk, even if they have significant risk factors. The guidelines recommend considering a lifetime risk score in such patients. However, many clinicians use CACS to guide prevention recommendations.
'Gray zone' (5 to 7.5 percent) ASCVD 10-year risk score
An imaging study may place the patient in either a lower or a higher risk category that would then impact clinical recommendations.
What is a high-risk imaging result?
CT of patient with CACS of 4,410 Agatston units
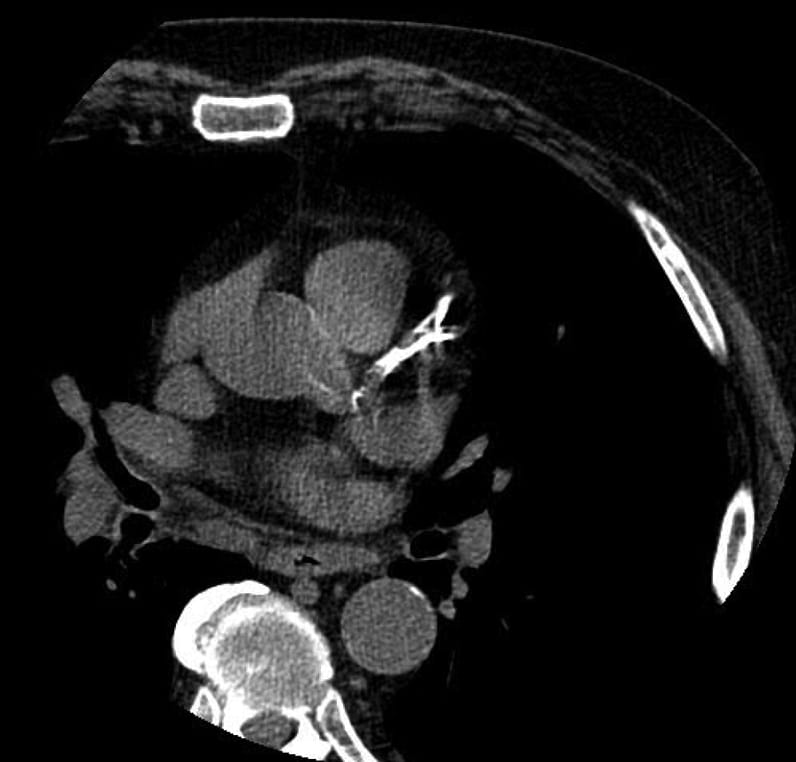
CT of patient with CACS of 4,410 Agatston units
This coronary artery calcium score (CACS) noncontrasted electrocardiographically gated computerized tomographic (CT) single-plane view was obtained in a 52-year-old man with a family history of premature coronary artery disease. This view demonstrates extensive calcification in the left main coronary artery, the proximal left anterior descending coronary artery and the proximal circumflex coronary artery. The total CACS was 4,410 Agatston units.
The generally accepted definition of high risk with CACS is a reading higher than 300 Agatston units or a CACS at or above the 75th percentile when adjusted for age, sex and race.
Too much or too little?
The answer to the question "Are we doing too many CACS studies or too few?" is primarily dependent on the clinical judgment of each clinician. "It is clear that there is great need to more accurately identify individuals who are at high risk of CVD prior to clinical events, yet the role of CACS in CVD risk prediction, if any, is not clearly defined from the current data," says Dr. Hurst.
Until more-definitive data become available, most experts in prevention of CVD favor a strategy that limits use of CACS to those patients for whom the result would have the most impact on treatment recommendations.
For more information
My Life Check — Life's Simple 7. American Heart Association.
Pooled Cohort Risk Assessment Equations: Predicts 10-year risk for a first atherosclerotic cardiovascular disease (ASCVD) event. ClinCalc.com.