Overview
Pelvic inflammatory disease, also called PID, is an infection of the reproductive organs of people assigned female at birth. It most often happens when sexually transmitted germs spread from the vagina to the uterus, fallopian tubes or ovaries.
The symptoms of pelvic inflammatory disease may be mild. Some people have no symptoms. If you don't have symptoms, you might not realize you have pelvic inflammatory disease until you have trouble getting pregnant or you get ongoing, called chronic, pelvic pain.
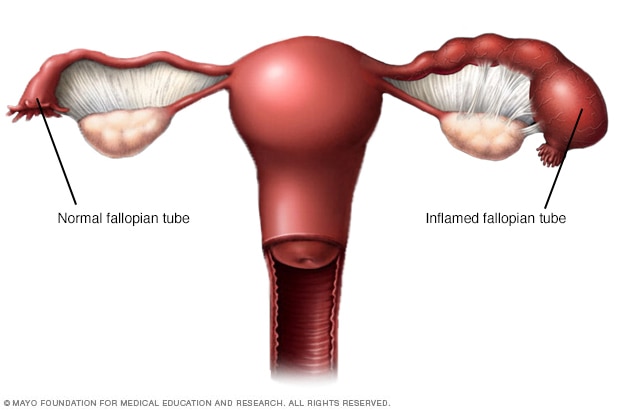
Pelvic inflammatory disease
Pelvic inflammatory disease, also called PID, is an infection of one or more of the upper reproductive organs in people assigned female at birth. These include the uterus, fallopian tubes and ovaries. If not treated, PID can cause scar tissue and pockets of infected fluid, called abscesses, in the reproductive tract. These can cause long-term damage.
Symptoms
The symptoms of pelvic inflammatory disease might be mild. Some people don't have symptoms. Symptoms may include:
- Pain in the lower belly and pelvis.
- Fluid that comes out of the vagina, called discharge, that's heavy or not usual. It may smell bad.
- Bleeding from the vagina between periods.
- Pain during sex.
- Fever, sometimes with chills.
- Urinating often. It may cause a burning feeling.
When to see a doctor
See your healthcare professional right away or seek emergency care if you have:
- Strong pain.
- Upset stomach and vomiting.
- A temperature higher than 101 degrees Fahrenheit (38.3 degrees Celsius).
Even if your PID symptoms don't bother you much, see your healthcare professional as soon as you can. Vaginal discharge with an odor, painful urination or bleeding between periods can be symptoms of a sexually transmitted infection, also called an STI.
If you have these symptoms, don't have sex. And make an appointment with your healthcare professional. Fast treatment of an STI can help prevent PID.
Women’s health topics – straight to your inbox
Causes
Many types of germs can cause PID. But gonorrhea and chlamydia are the most common. You may get these germs during sex if you don't use protection, such as a condom.
Other germs also can cause pelvic inflammatory disease. These include bacteria in the vagina that are typical but out of balance. This is called bacterial vaginosis.
Rarely, germs may enter the reproductive tract when a healthcare professional puts in an intrauterine device, also called an IUD, for long-term birth control. Any medical procedure that involves putting instruments into the uterus also can cause PID.
Risk factors
Factors that might increase your risk of pelvic inflammatory disease include:
- Being sexually active and younger than 25 years old.
- Having more than one sex partner.
- Having sex with someone who has more than one sex partner.
- Having sex without using a condom the right way.
- Douching. This upsets the balance between good germs and harmful ones in the vagina. Douching might mask symptoms of PID.
- Having had pelvic inflammatory disease or a sexually transmitted infection.
Complications
Pelvic inflammatory disease may cause scar tissue and pockets of infected fluid, called abscesses, in the reproductive tract. These can cause lasting damage to the reproductive organs.
Complications from this damage might include:
- Ectopic pregnancy. PID is a major cause of ectopic pregnancy, also called tubal pregnancy. An ectopic pregnancy can happen when PID causes scar tissue in one of the tubes that links the uterus to the ovaries, called the fallopian tubes. The scar tissue keeps the fertilized egg from making it through the fallopian tube to the uterus.
The fertilized egg then grows in the fallopian tube. Ectopic pregnancies can cause life-threatening bleeding and need emergency medical attention.
- Trouble getting pregnant. Damage to your reproductive organs can keep you from getting pregnant, called infertility. The more times you've had PID, the greater your risk of infertility. Delaying treatment for PID also greatly raises your risk of infertility.
- Ongoing, called chronic, pelvic pain. Pelvic inflammatory disease can cause pelvic pain that might last for months or years. Scarring in the fallopian tubes and other pelvic organs can cause pain during sex and when the body releases an egg, called ovulation.
- Tubo-ovarian abscess. PID might cause pus to form in the reproductive tract. This is called an abscess. Most often, abscesses affect the fallopian tubes and ovaries. But they can form in the uterus or in other pelvic organs. An abscess may turn into a life-threatening infection.
Prevention
To lower your risk of pelvic inflammatory disease:
- Practice safer sex. Use condoms every time you have sex, limit your number of partners and ask about a partner's sexual history before you have sex.
- Talk with your healthcare professional about birth control. Many forms of birth control don't protect against getting PID. Using barrier methods, such as a condom, helps lower the risk. Even if you take birth control pills, use a condom every time you have sex with a new partner to protect against STIs.
- Get tested. If you're at risk of an STI, make an appointment with your healthcare professional for testing. Set up a regular screening schedule with your healthcare professional if needed. Early treatment of an STI gives you the best chance of not getting PID.
- Ask your partner to be tested. If you have pelvic inflammatory disease or an STI, ask your partner to be tested and treated. This can prevent the spread of STIs and keep PID from coming back.
- Don't douche. Douching upsets the balance of germs in the vagina.