Overview
Open-angle glaucoma
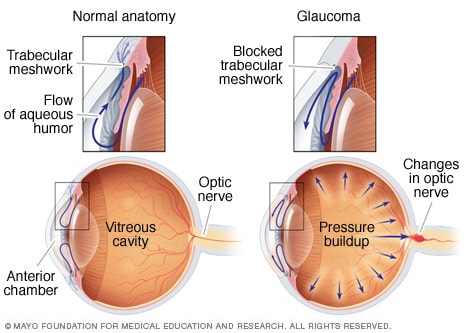
Open-angle glaucoma
Usually, fluid called aqueous humor flows freely through the anterior chamber in the eye and exits through the drainage system, known as the trabecular meshwork. If that system is blocked or isn't functioning well, the pressure inside the eye builds. This pressure can damage the optic nerve. With the most common type of glaucoma, this results in gradual vision loss.
Glaucoma is an eye condition that damages the optic nerve. This damage can lead to vision loss or blindness. The optic nerve sends visual information from your eye to the brain and is vital for good vision. Damage to the optic nerve is often related to high pressure in the eye. But glaucoma can happen even with typical eye pressure.
Glaucoma can happen at any age but is more common in older adults. It is one of the leading causes of blindness for people over the age of 60.
Many forms of glaucoma have no warning signs. The effect is so gradual that you may not notice a change in vision until the condition is in its later stages.
It's important to have regular eye exams that include measurements of your eye pressure. If glaucoma is found early, vision loss can be slowed or prevented. If you have glaucoma, you'll need treatment or monitoring for the rest of your life.
Symptoms
The symptoms of glaucoma depend on the type and stage of the condition.
Open-angle glaucoma
- No symptoms in early stages.
- Gradually, patchy blind spots in your side vision. Side vision also is called peripheral vision.
- In later stages, difficulty seeing things in your central vision.
Acute angle-closure glaucoma
- Bad headache.
- Severe eye pain.
- Nausea or vomiting.
- Blurred vision.
- Halos or colored rings around lights.
- Eye redness.
Normal-tension glaucoma
- No symptoms in early stages.
- Gradually, blurred vision.
- In later stages, loss of side vision.
Glaucoma in children
- A dull or cloudy eye (infants).
- Increased blinking (infants).
- Tears without crying (infants).
- Blurred vision.
- Nearsightedness that gets worse.
- Headache.
Pigmentary glaucoma
- Halos around lights.
- Blurred vision with exercise.
- Gradual loss of side vision.
When to see a doctor
If you have symptoms that come on suddenly, you may have acute angle-closure glaucoma. Symptoms include bad headache and severe eye pain. You need treatment as soon as possible. Go to an emergency room or call an eye doctor, called an ophthalmologist, immediately.
Causes
Glaucoma develops when the optic nerve becomes damaged. As this nerve gradually gets worse, blind spots develop in your vision. For reasons that eye doctors don't fully understand, this nerve damage is usually related to increased pressure in the eye.
Raised eye pressure happens as the result of a buildup of fluid that flows throughout the inside of the eye. This fluid, called the aqueous humor, usually drains through a tissue located at the angle where the iris and cornea meet. This tissue is called the trabecular meshwork. The cornea is important to vision because it lets light into the eye. When the eye makes too much fluid or the drainage system doesn't work properly, eye pressure may increase.
Open-angle glaucoma
This is the most common form of glaucoma. The drainage angle formed by the iris and cornea remains open. But other parts of the drainage system don't drain properly. This may lead to a slow, gradual increase in eye pressure.
Acute angle-closure glaucoma
This form of glaucoma happens when the iris bulges. The bulging iris partially or completely blocks the drainage angle. As a result, fluid can't circulate through the eye and pressure increases. Angle-closure glaucoma may happen suddenly or gradually.
Normal-tension glaucoma
No one knows the exact reason why the optic nerve becomes damaged when eye pressure is healthy. The optic nerve may be sensitive or experience less blood flow. This limited blood flow may be caused by the buildup of fatty deposits in the arteries or other conditions that damage circulation. The buildup of fatty deposits in the arteries also is known as atherosclerosis.
Glaucoma in children
A child may be born with glaucoma or develop it in the first few years of life. Blocked drainage, injury or an underlying medical condition may cause optic nerve damage.
Pigmentary glaucoma
In pigmentary glaucoma, small pigment granules flake off from the iris and block or slow fluid drainage from the eye. Activities such as jogging sometimes stir up the pigment granules. That leads to a deposit of pigment granules on tissue located at the angle where the iris and cornea meet. The granule deposits cause an increase in pressure.
Glaucoma tends to run in families. In some people, scientists have identified genes related to high eye pressure and optic nerve damage.
Risk factors
Glaucoma can damage vision before you notice any symptoms. So be aware of these risk factors:
- High internal eye pressure, also known as intraocular pressure.
- Age over 55.
- Black, Asian or Hispanic heritage.
- Family history of glaucoma.
- Certain medical conditions, such as diabetes, migraine, high blood pressure and sickle cell anemia.
- Corneas that are thin in the center.
- Extreme nearsightedness or farsightedness.
- Eye injury or certain types of eye surgery.
- Taking corticosteroid medicines, especially eye drops, for a long time.
Some people have narrow drainage angles, putting them at increased risk of angle-closure glaucoma.
Prevention
These steps may help find and manage glaucoma in its early stages. That may help to prevent vision loss or slow its progress.
-
Get regular eye exams. Regular eye exams can help find glaucoma in its early stages, before a lot of damage occurs. As a general rule, the American Academy of Ophthalmology recommends a comprehensive eye exam every 5 to 10 years if you're under 40 years old; every 2 to 4 years if you're 40 to 54 years old; every 1 to 3 years if you're 55 to 64 years old; and every 1 to 2 years if you're older than 65.
If you're at risk of glaucoma, you'll need screening more often. Ask a healthcare professional to recommend the right screening schedule for you.
- Know your family's eye health history. Glaucoma tends to run in families. If you're at increased risk, you may need screening more often.
- Wear eye protection. Serious eye injuries can lead to glaucoma. Wear eye protection when using power tools or playing sports.
- Take prescribed eye drops regularly. Glaucoma eye drops can greatly reduce the risk that high eye pressure will progress to glaucoma. Use eye drops as prescribed by a healthcare professional even if you have no symptoms.
Nov. 05, 2024