Overview
Gingivitis is a common and mild form of gum disease, also called periodontal disease. It causes irritation, redness, swelling and bleeding of your gingiva, which is the part of your gum around the base of your teeth. It's important to take gingivitis seriously and treat it promptly. Gingivitis does not cause bone loss. But left untreated, it can lead to a much more serious gum disease, called periodontitis, and tooth loss.
The most common cause of gingivitis is not keeping your teeth and gums clean and healthy. Good oral health habits, such as brushing at least twice a day, flossing daily and getting regular dental checkups, can help prevent and reverse gingivitis.
Products & Services
Symptoms
Gingivitis
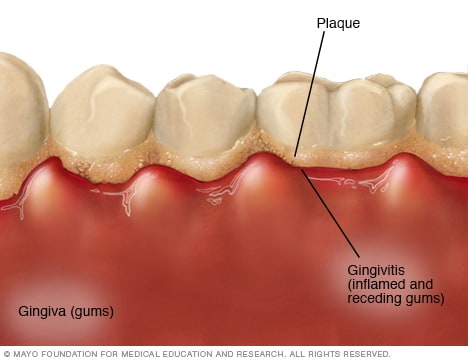
Gingivitis
Gingivitis can cause bright or dark red, swollen, tender gums that bleed easily, especially when you brush your teeth.
Healthy gums are firm and pale pink. They fit tightly around the teeth. Symptoms of gingivitis include:
- Swollen or puffy gums.
- Bright red or dark red gums, or gums that are darker than usual.
- Gums that bleed easily when you brush or floss.
- Tender gums.
- Bad breath.
When to see a dentist
If you notice any symptoms of gingivitis, schedule an appointment with your dentist as soon as possible. The sooner you seek care, the better your chances of reversing damage from gingivitis and not getting periodontitis. Your dentist may want you to see a periodontist if your symptoms aren't improving. This is a dentist with advanced training who specializes in treating gum diseases.
Causes
The most common cause of gingivitis is poor care of teeth and gums, which allows plaque to form on teeth. This causes swelling of the surrounding gum tissues.
Here's how plaque can lead to gingivitis:
- Plaque forms on your teeth. Plaque is a sticky film that has no color. It's mainly made up of bacteria that form on your teeth after eating starches and sugars in food. Plaque needs to be removed every day because it forms quickly.
- Plaque turns into tartar. Plaque that stays on your teeth can harden under your gumline into tartar. This tartar, also known as calculus, then collects bacteria. Tartar makes plaque harder to remove, creates a protective shield for bacteria and irritates the gumline. You need professional dental cleaning to remove tartar.
- Gingiva becomes irritated and swells. The gingiva is the part of your gum around the base of your teeth. The longer that plaque and tartar remain on your teeth, the more they irritate the gingiva. In time, your gums become swollen and bleed easily. This is called gingivitis. If not treated, gingivitis can lead to tooth decay, periodontitis and tooth loss.
Risk factors
Gingivitis is common, and anyone can develop it. Factors that can increase your risk of gingivitis include:
- Poor oral care habits.
- Smoking or chewing tobacco.
- Older age.
- Dry mouth.
- Poor nutrition, including not getting enough vitamin C.
- Repairs to teeth that don't fit properly or are in poor condition, such as fillings, bridges, dental implants or veneers.
- Crooked teeth that are hard to clean.
- Conditions that lower immunity, such as leukemia, HIV/AIDS or cancer treatment.
- Certain drugs, such as phenytoin (Dilantin, Phenytek, others) for epileptic seizures and some calcium channel blockers used for angina, high blood pressure and other conditions.
- Hormonal changes, such as those related to pregnancy, the menstrual cycle or use of birth control pills.
- Certain genes.
- Medical conditions, such as certain viral and fungal infections.
Complications
Untreated gingivitis can lead to gum disease that spreads to underlying tissue and bone, called periodontitis. This is a much more serious condition that can lead to tooth loss.
Ongoing gum disease may be related to some diseases that affect the entire body, such as respiratory disease, diabetes, coronary artery disease, stroke and rheumatoid arthritis. Some research suggests that the bacteria responsible for periodontitis can enter your bloodstream through gum tissue, possibly affecting your heart, lungs and other parts of your body. But more studies are needed to confirm a link.
Trench mouth, also known as necrotizing ulcerative gingivitis or NUG, is a severe form of gingivitis that causes painful, infected, bleeding gums and ulcers. Trench mouth is rare today in developed nations, though it's common in developing countries that have poor nutrition and poor living conditions.
Prevention
To prevent gingivitis:
- Practice good oral care. That means brushing your teeth for two minutes at least twice daily — in the morning and before going to bed — and flossing at least once a day. Better yet, brush after every meal or snack or as your dentist recommends. Flossing before you brush cleans away loosened food particles and bacteria.
- Go to the dentist regularly. See your dentist or dental hygienist regularly for cleanings, usually every 6 to 12 months. If you have risk factors that increase your chance of developing periodontitis — such as having dry mouth, taking certain medicines or smoking — you may need professional cleaning more often. Annual dental X-rays can help pinpoint diseases not seen by a visual dental exam and watch for changes in your dental health.
- Take steps to lead a healthy lifestyle. Practices such as healthy eating and managing blood sugar if you have diabetes, for example, also are important to supporting gum health.
Nov. 16, 2023