Diagnosis
An important part of diagnosing Alzheimer's disease includes being able to explain your symptoms. It may help to get input from a close family member or friend about your symptoms and their impact on your daily life. Tests of memory and thinking skills also help diagnose Alzheimer's disease.
Blood and imaging tests can rule out other potential causes of your symptoms. They also can check for proteins in the brain that are linked to Alzheimer's disease. The tests may help your healthcare team better identify the disease causing dementia symptoms.
In the past, Alzheimer's disease was diagnosed for certain only after death when plaques and tangles were found while looking at the brain with a microscope. Today, healthcare professionals and researchers are able to diagnose Alzheimer's disease during life with more certainty.
They do this by using a combination of tests that may include tests for biomarkers. Biomarkers can detect if plaques and tangles are present in the brain. Biomarker tests include specific types of positron emission tomography, also known as PET, scans of the brain. Amyloid and tau proteins also can be measured in the fluid part of the blood or in the fluid that surrounds the brain and spinal cord, known as cerebrospinal fluid. Recently, blood biomarker tests have become accurate enough to tell if someone is likely to have amyloid in the brain.
Biomarker tests were mainly used in clinical trials until recently. But healthcare professionals have started using them along with other tests to help diagnose Alzheimer's disease. Biomarker tests also can let healthcare professionals know if the disease is in the early or later stages.
Tests
Diagnosing Alzheimer's disease would likely include the following tests:
Physical and neurological exam
A healthcare professional gives you a physical and neurological exam. This may include testing:
- Reflexes.
- Muscle tone and strength.
- Ability to get up from a chair and walk across the room.
- Sense of sight and hearing.
- Coordination.
- Balance.
Lab tests
Blood tests may help rule out other potential causes of memory loss and confusion, such as a thyroid disorder or vitamin levels that are too low.
Newer blood tests can measure levels of beta-amyloid protein and tau protein. But these tests aren't available everywhere and may not be covered by insurance.
Mental status and neuropsychological testing
Your healthcare professional may give you a brief mental status test to check your memory and other thinking skills. Longer forms of this type of test may provide more details about mental function that can be compared with people of a similar age and education level. These tests can help establish a diagnosis and serve as a starting point to track symptoms in the future.
Brain imaging
Brain scan images for diagnosis of Alzheimer's disease
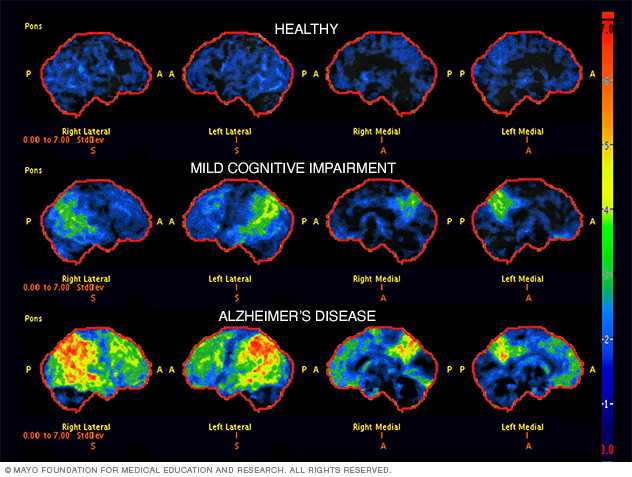
Brain scan images for diagnosis of Alzheimer's disease
Brain scans known as fluorodeoxyglucose PET, also called FDG PET, may be used to diagnose Alzheimer's disease. FDG PET scans show areas of the brain where nutrients aren't properly used for energy, known as metabolism. The scans in this image show a healthy brain, a brain with mild cognitive impairment and a brain with Alzheimer's disease. Areas that are black and blue represent healthy brain metabolism. Areas that are green, yellow and red represent worsening brain metabolism as the disease gets worse.
Images of the brain look for visible changes related to conditions other than Alzheimer's disease that may cause similar symptoms, such as strokes, injury or tumors. Newer imaging tests can help detect specific brain changes caused by Alzheimer's disease, such as amyloid plaques and neurofibrillary tangles. These newer tests are mainly used in major medical centers or in clinical trials.
Imaging of brain structures include:
- Magnetic resonance imaging (MRI). MRI uses radio waves and a strong magnetic field to produce detailed images of the brain. They may show shrinkage of some brain regions linked to Alzheimer's disease. MRI scans also can rule out other conditions that may be causing symptoms. An MRI is generally preferred to a CT scan to evaluate dementia. MRIs also are done before starting certain Alzheimer's medicines and throughout treatment to monitor for potential side effects.
- Computerized tomography (CT). A CT scan, a specialized X-ray technology, produces cross-sectional images of your brain. It's usually used to rule out tumors, strokes and head injuries.
A PET scan test can capture images of the disease process. During a PET scan, a low-level radioactive tracer is injected into the blood to reveal a particular feature in the brain. PET imaging may include:
- Fluorodeoxyglucose, also called FDG, PET imaging scans show areas of the brain where nutrients aren't properly being used for energy, known as metabolism. Finding patterns in the areas of low metabolism can help distinguish between Alzheimer's disease and other types of dementia.
- Amyloid PET imaging can measure amyloid plaques in the brain. This test is mainly used in research but may be used if a person has unusual or very early onset of dementia symptoms.
- Tau PET imaging measures neurofibrillary tangles in the brain.
Sometimes other tests may be used to measure amyloid and tau in the cerebrospinal fluid. This may be done if symptoms are quickly getting worse or if dementia is affecting someone at a younger age.
Future of diagnostic tests
Research has established that biomarker tests can measure biological signs of disease in the brain. The tests can be used with other tools to help diagnose Alzheimer's disease after symptoms begin. Although these tests can look for signs of Alzheimer's before symptoms begin, the tests aren't being used in people without symptoms. The availability of biomarker tests may vary widely.
Genetic tests aren't recommended for most people who might have Alzheimer's disease. But people with a family history of early-onset Alzheimer's disease may consider being tested. Meet with a genetic counselor to talk about the risks and benefits before getting a genetic test.
More Information
Treatment
Treatments for Alzheimer's disease include medicines that can help with symptoms and newer medicines that can help slow decline in thinking and functioning. These newer medicines are approved for people with early Alzheimer's disease.
Medicines
Alzheimer's medicines can help with memory symptoms and other cognitive changes. Two types of medicines used to treat symptoms include:
-
Cholinesterase inhibitors. These medicines work by boosting levels of cell-to-cell communication. The medicines preserve a chemical messenger that is depleted in the brain by Alzheimer's disease. These are usually the first medicines tried, and most people see modest improvements in symptoms.
Cholinesterase inhibitors may improve symptoms related to behavior, such as agitation or depression. The medicines are taken by mouth or through a patch on the skin. Commonly prescribed cholinesterase inhibitors include donepezil (Aricept, Adlarity), galantamine and rivastigmine transdermal patch (Exelon).
The main side effects of these medicines include diarrhea, nausea, loss of appetite and trouble with sleep. In people with certain heart conditions, serious side effects may include an irregular heartbeat.
- Memantine (Namenda). This medicine works in another brain cell communication network and slows the progression of symptoms with moderate to severe Alzheimer's disease. It's sometimes used in combination with a cholinesterase inhibitor. Relatively rare side effects include dizziness and confusion.
Other medicines have been approved by the Food and Drug Administration, also called FDA, to slow declines in thinking and functioning caused by Alzheimer's disease. The medicines prevent amyloid plaques in the brain from clumping. They're prescribed for people with mild Alzheimer's disease and mild cognitive impairment due to Alzheimer's disease.
These medicines include:
- Lecanemab-irmb (Leqembi). This medicine is given as an IV infusion every two weeks. Side effects may include infusion-related reactions such as fever, flu-like symptoms, nausea, vomiting, dizziness, changes in heart rate and trouble breathing.
- Donanemab-azbt (Kisunla). This medicine is given as an IV infusion every four weeks. Side effects may include flu-like symptoms, nausea, vomiting, headache, trouble breathing and changes in blood pressure.
People taking lecanemab or donanemab may have swelling in the brain or may get small bleeds in the brain. Rarely, brain swelling can be serious enough to cause seizures and other symptoms. Also in rare instances, bleeding in the brain can cause death. The FDA recommends getting a brain MRI before starting treatment and regularly during treatment to monitor for symptoms of brain swelling or bleeding.
People who carry a certain form of a gene known as APOE e4 appear to have a higher risk of these serious side effects. The FDA recommends testing for this gene before starting treatment.
If you take a blood thinner or have other risk factors for brain bleeding, talk to your healthcare professional before taking lecanemab or donanemab. Blood-thinning medicines may increase the risk of bleeds in the brain.
More research is being done on the potential risks of taking lecanemab and donanemab. Other research is looking at how effective the medicines may be for people at risk of Alzheimer's disease, including people who have a first-degree relative, such as a parent or sibling, with the disease.
Sometimes other medicines such as antidepressants may be prescribed to help manage the behavioral symptoms linked to Alzheimer's disease.
Creating a safe and supportive environment
An important part of any treatment plan is to adapt to the needs of a person with Alzheimer's disease. Create routine habits and cut down on tasks that require memory. These steps can make life much easier.
These are ways to support a person's sense of well-being and ability to function:
- Keep keys, wallets, mobile phones and other valuables in the same place at home so they don't become lost.
- Keep medicines in a secure location. Use a daily checklist to keep track of doses.
- Arrange for finances to be on automatic payment and automatic deposit.
- Have the person with Alzheimer's carry a mobile phone with location tracking. Program important phone numbers into the phone.
- Install alarm sensors on doors and windows.
- Make sure regular appointments are on the same day at the same time as much as possible.
- Use a calendar or whiteboard to track daily schedules. Build the habit of checking off completed items.
- Remove furniture, clutter and throw rugs that aren't needed.
- Install sturdy handrails on stairs and in bathrooms.
- Ensure that shoes and slippers are comfortable and provide good traction.
- Reduce the number of mirrors. People with Alzheimer's may find images in mirrors confusing or scary.
- Make sure that the person with Alzheimer's carries ID or wears a medical alert bracelet.
- Keep photos and other objects with meaning around the house.
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Alternative medicine
Herbal remedies, vitamins and other supplements are widely promoted for cognitive health or to prevent or delay Alzheimer's. But clinical trials have produced mixed results. There's little evidence to support them as effective treatments.
Some of the treatments that have been studied include:
-
Vitamin E. Although vitamin E doesn't prevent Alzheimer's, taking 2,000 international units daily may help delay symptoms from getting worse in people who already have mild to moderate disease. But study results have been mixed, with only some showing modest benefits. Further research into the safety of people with dementia taking 2,000 international units daily of vitamin E are needed before it can be routinely recommended.
Supplements promoted for cognitive health can interact with medicines you're taking for Alzheimer's disease or other health conditions. Work closely with your healthcare team to create a safe treatment plan. Tell your healthcare team about your prescriptions and any medicines or supplements taken without a prescription.
- Omega-3 fatty acids. Omega-3 fatty acids in fish or from supplements may lower the risk of dementia. But clinical trials have shown no benefit for treating Alzheimer's disease symptoms.
- Curcumin. This herb comes from turmeric and has anti-inflammatory and antioxidant properties that might affect chemical processes in the brain. So far, clinical trials have found no benefit for treating Alzheimer's disease.
- Ginkgo. Ginkgo is a plant extract. A large study funded by the National Institutes of Health found no effect in preventing or delaying Alzheimer's disease.
- Melatonin. This supplement helps with sleep. It's being studied to see if it can help people with dementia manage sleep symptoms. But some research has found that melatonin may worsen mood in some people with dementia. More research is needed.
Lifestyle and home remedies
Healthy lifestyle choices promote good overall health. They also may play a role in maintaining brain health.
Exercise
Regular exercise is an important part of a treatment plan. Activities such as a daily walk can help improve mood and maintain the health of joints, muscles and the heart. Exercise also promotes restful sleep and prevents constipation. It's beneficial for care partners, too.
People with Alzheimer's who have trouble walking may still be able to use a stationary bike, stretch with elastic bands or do chair exercises. You might find exercise programs for older adults at community centers or on TV, the internet or DVDs.
Nutrition
People with Alzheimer's may forget to eat, lose interest in meals or may not eat healthy foods. They may also forget to drink enough, leading to dehydration and constipation.
Offer the following:
- Healthy options. Buy favorite healthy food options that are easy to eat.
- Water and other healthy beverages. Encourage drinking several glasses of liquids every day. Don't offer beverages with caffeine, which can increase restlessness, affect sleep and trigger a need to urinate often.
- High-calorie, healthy shakes and smoothies. Serve milkshakes with protein powders or make smoothies. This is helpful when eating becomes very hard.
Social engagement and activities
Social activities can support preserved skills and abilities. They also help with overall well-being. Do things that are meaningful and enjoyable. Someone with dementia might:
- Listen to music or dance.
- Read or listen to books.
- Garden or do crafts.
- Go to social events at senior or memory care centers.
- Do activities with children.
Coping and support
People with Alzheimer's disease experience a mixture of emotions — confusion, frustration, anger, uncertainty, grief and depression.
If you're caring for someone with Alzheimer's, you can help them cope by being there to listen. Reassure the person that life can still be enjoyed, provide support, and do your best to help the person retain dignity and self-respect.
A calm and stable home environment can help reduce behavior problems. New situations, noise and large groups of people can cause anxiety. Being rushed or pressed to remember, or being asked to do complex tasks also may make someone with dementia anxious. When someone with Alzheimer's becomes upset, it's even harder to think clearly.
Caring for the caregiver
Caring for a person with Alzheimer's disease is physically and emotionally demanding. Feelings of anger, guilt, stress, worry, grief and social isolation are common.
Caregiving can even take a toll on the caregiver's physical health. Pay attention to your own needs and well-being. It's one of the most important things you can do for yourself and for the person with Alzheimer's.
If you're a caregiver for someone with Alzheimer's, you can:
- Learn as much about the disease as you can.
- Ask questions of healthcare professionals, social workers and others involved in the care of your loved one.
- Call on friends or other family members for help when you need it.
- Take a break every day.
- Spend time with your friends.
- Take care of your health by seeing your own healthcare professionals on schedule, eating healthy meals and getting exercise.
- Join a support group.
- Make use of a local adult care center, if possible.
Many people with Alzheimer's and their families benefit from counseling or local support services. Contact your local Alzheimer's Association affiliate to connect with support groups, healthcare professionals, occupational therapists, resources and referrals. You can find information about home care agencies, residential care facilities, a telephone help line and educational seminars.
Preparing for your appointment
Medical care for the loss of memory or other thinking skills usually requires a team or partner strategy. If you're worried about memory loss or related symptoms, ask a close relative or friend to go with you to an appointment with a healthcare professional. Having a partner can provide support and help you answer questions.
If you're going with someone who is having memory issues to a healthcare appointment, your role may be to provide some history or your thoughts on changes you have seen. This teamwork is an important part of medical care.
Your healthcare professional may refer you to a neurologist, psychiatrist, neuropsychologist or other specialist for further evaluation.
What you can do
You can prepare for your appointment by writing down as much information as possible to share. Information may include:
- Medical history, including any past or current diagnoses and family medical history.
- Medical team, including the name and contact information of any current physician, mental health professional or therapist.
- Medicines, including prescriptions, medicines you take without a prescription, vitamins, herbs or other supplements.
- Symptoms, including specific examples of changes in memory or thinking skills.
What to expect from your doctor
Your healthcare professional asks questions to understand changes in memory or other thinking skills. Your healthcare professional may ask:
- What kinds of memory symptoms are you having? When did you first notice them?
- Are they steadily getting worse, or are they sometimes better and sometimes worse?
- Have you stopped doing certain activities, such as managing finances or shopping, because these activities were too mentally challenging?
- How is your mood? Do you feel depressed, sadder or more anxious than usual?
- Have you gotten lost lately while driving or in a situation that's usually familiar to you?
- Has anyone expressed unusual concern about your driving?
- Have you noticed any changes in the way you tend to react to people or events?
- Do you have more energy than usual, less than usual or about the same?
- What medicines are you taking? Are you taking any vitamins or supplements?
- Do you drink alcohol? How much?
- Have you noticed any trembling or trouble walking?
- Are you having trouble remembering healthcare appointments or when to take your medicines?
- Have you had your hearing and vision tested recently?
- Did anyone else in your family ever have memory trouble? Was anyone ever diagnosed with Alzheimer's disease or dementia?
- Do you act out your dreams while sleeping? For example, do you punch, flail, shout or scream during sleep? Do you snore?