April 27, 2018
Blunt trauma to the eye
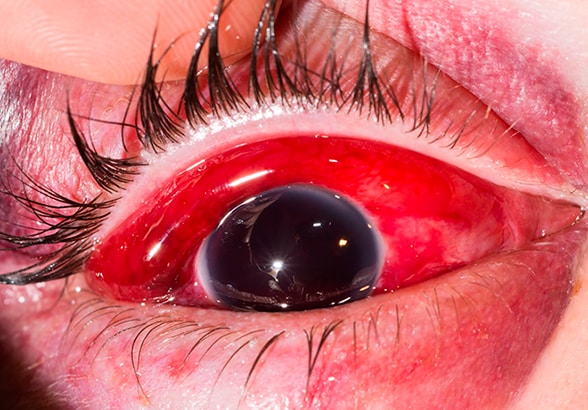
Blunt trauma to the eye
A close-up reveals blunt trauma to a patient's eye upon examination.
A softball to the eye, a tumble to the floor, a gunshot wound while hunting, or a wayward fist at a local watering hole all might send a patient to the trauma center with an orbital or ocular injury. In patients with facial fractures, 20 to 25 percent include orbital involvement at some level. Of this group, over 80 percent will include ocular trauma.
Profile of a patient with ocular or orbital trauma
The most common patient with ocular or orbital trauma is a young male involved in interpersonal violence. Geriatric patients commonly experience this injury through falls, and a wide variety of patients suffer ocular or orbital trauma from motor vehicle crashes. Athletes also incur these injuries, most commonly baseball, softball, soccer, ice hockey or rugby players.
"Today, our sports activities have become higher velocity and significantly higher risk, so we tend to see more orbital fractures and ocular injuries now than in the past with somewhat different epidemiology," says Christopher F. Viozzi, D.D.S., M.D., chair of Oral and Maxillofacial Surgery at Mayo Clinic's campus in Rochester, Minnesota.
Ocular or orbital injury types
Patients with ocular or orbital injuries may present with pain in and around the orbit, bruising, swelling, bleeding from lacerations, and facial numbness, and may complain of changes in vision. These injuries may require only observation or surgery spanning from simple to complex.
"With any of these injuries, it's a matter of energy transfer," says Dr. Viozzi, who has a background in mechanical engineering and notes similarities in vocabulary. "If a person falls, clunks their cheekbone and develops a crack in the orbital floor, energy transferred by the point their face hit the ground was fairly low. You contrast that with a ballistic injury where somebody's been shot in the cheekbone, and there's going to be a lot of involvement of the eye socket, the orbit and the globe itself."
In addition to energy transfer, mechanism of injury largely dictates risk and the severity of ocular and orbital injuries. Due to high velocity, the most destructive types of ocular or orbital injuries are high-speed motor vehicle collisions or ballistic injuries.
Also depending on injury mechanism, patients may have concurrent injuries. In a motor vehicle crash, for example, patients may have other facial injuries, including other fractures; soft tissue damage; laryngotracheal injury with potential airway compromise; or closed or open head injuries. Sometimes the severity of an ocular injury such as an open globe with acute vision loss can be very distracting to the physicians evaluating the patient. It's crucial to not miss other potentially life-threatening injuries.
Management of ocular or orbital injury
Dr. Viozzi, who sees all types of facial trauma, offers a few tips for treating ocular or orbital injuries:
Appearance
Ocular injuries, in particular, may be quite severe and cause stress for providers involved, as well as for the patient and family.
Pain
Most patients with any form of facial fracture — such as orbital — will experience moderate to severe pain, which needs to be managed. This is due to a relatively high density of sensory pain fibers in the facial and orbital regions, thus making pain symptoms significant.
Diagnosis
Orbital fractures can be obvious, but frequently are subtle and can therefore present a diagnostic challenge. If any suspicion for fracture is present, it's appropriate to order a CT scan to determine if orbital trauma exists. However, if a patient exceeds the capacity of the low-volume trauma center, imaging should be deferred, especially if life threats are present.
If the patient is unconscious, diagnosis is even more problematic absent patient interaction, and orbital injuries can be overlooked. Missing an orbital or ocular injury at the outset is also possible in polytrauma cases, where the primary focus is the trauma ABCs — concerns that might rapidly take the patient's life.
Immediate treatment
When a patient arrives with an obvious eye injury, a robust general trauma assessment is the first step in caring for the patient. Once more-serious injuries have been ruled out or addressed, one may consider evaluation and treatment of the ocular trauma. Evaluation of visual acuity, detection of soft tissue injuries, observation of epiphora, evaluation of extraocular muscle function and globe position, and palpation for bony deformities should proceed in a systematic manner.
With corneal abrasion, which is very common in orbital trauma, patients can be profoundly uncomfortable, making pain control particularly important. If there's a potential orbital floor injury, it's critical the patient avoids or takes great care with nose blowing, so nasal bacteria are not passed upward into the orbit. If the orbital injury is connected in any manner to the sinus or nasal cavity, administer antibiotics.
Treatment priorities
After the primary trauma evaluation to rule out life-threatening injuries, attention can be focused on any injury that might threaten the patient's vision or eye function, which would require rapid consult with an ophthalmologist. Examples of these types of injuries include: Retrobulbar hemorrhage: This bleeding behind the globe is an emergent issue, as the pressure in the eye socket can become so high that it hinders any blood flow to the retina, resulting in retinal ischemia and blindness.
Any obvious globe injury, such as open globe, lens dislocation or hyphema
Extraocular muscle entrapment from orbital floor fracture in a child: This is indicated by inability to move the eye in upward gaze, or sometimes downward gaze, and one may observe autonomic instability, the oculocardiac reflex. Patients less than approximately 10 years of age may need emergent surgery to release the muscle from the fracture to prevent acute hemodynamic instability as well as long-term ocular motility problems.
"Ninety-nine percent of the time, a fracture does not have to be dealt with emergently," says Dr. Viozzi. "There is usually plenty of time to repair orbital fractures, especially for a patient who comes in with multiple injuries."
Nontreatment in some cases
In cases where orbital fracture causes only facial contour deformity, this is a cosmetic problem, rather than functional — the patient is seeing fine and has no double vision, vision loss or other vision impairment — nonsurgical treatment is also a consideration. An older adult patient, for instance, may have other illnesses and be too fragile to have surgery for cosmetic reasons alone and frequently will be unimpressed by esthetic concerns. Other patients may not be bothered by a slight cheekbone flattening from the trauma and will not elect surgery. However, surgical repair is often performed in young patients with orbital region cosmetic changes.
Potential long-term effects of orbital and ocular injuries
Long-term functional effects of ocular or orbital injury are infrequent when appropriate treatment is rendered in the acute phase, or within the first three to four weeks of injury. Cosmetic effects, however, may still be present at some level.
"If you have surgery on the face, you can't cover it up — it's out there for everyone to see," says Dr. Viozzi. "It can create issues of anxiety and depression."
Other long-term effects of these traumas are functional, such as vision loss or chronic double vision. These issues hinder a patient's ability to drive, fly a plane or even work, if vision is an essential part of one's job. Dr. Viozzi notes there are very few jobs where visual loss is not severely impactful of full employment.
The question of transfer
Whether or not a patient with an ocular or orbital injury should be transferred to a higher level of care is highly dependent on the resources at the particular facility where the patient first arrives.
A couple of key questions to ask include:
- If examination or imaging indicates an injury that is an immediate threat to the patient's vision (see above): Is there an ophthalmologist on-call and available who could manage this case? If the answer is no, it's imperative to transfer the patient quickly to a hospital that can manage such an injury.
- If a patient presents with orbital fracture without ocular injury: Do you have a surgeon available to repair such a fracture? If not, then transfer.
A small hospital often will have very well-trained surgeons or ophthalmologists who can manage these injuries, according to Dr. Viozzi. A decision to transfer or keep the patient locally may depend on who's on call, where the on-call staff is located at patient arrival and support available to the surgeon — that very day in case of emergent ocular injury.
"Not every person is comfortable with every case," says Dr. Viozzi, commenting that this is perfectly reasonable and normal. "Each patient and their facial injuries are unique, so you have to make a determination of what is a fit for the patient, the particular injuries and the staff you have on hand."