June 13, 2018
Obesity is a life-limiting disorder associated with a number of comorbidities. Currently more than two-thirds of Americans are overweight (BMI ≥ 25 kg/m2) and over one-third are obese (BMI ≥ 30 kg/m2). Worldwide, 500 million adults are obese, and this number is estimated to increase to 1.12 billion by 2030.
Manpreet S. Mundi, M.D., with Endocrinology, Diabetes, Metabolism, and Nutrition at Mayo Clinic's campus in Rochester, Minnesota, says, "Although there are many ways to lose weight in the short term, less than 20 percent of individuals who try to lose weight are able to achieve and maintain a 10 percent reduction over a year, with the majority gaining it back within three to five years.
"With regain of weight, individuals experience relapse of weight-related medical comorbidities, thus contributing once more to socio-economic and direct health care costs. This cycle of weight loss and regain is frustrating to individuals, and despite our understanding of the biological and behavioral defenses mounted by the body to maintain weight, there still exists a pragmatic gap for individuals who are directly affected."
Weight-loss (bariatric) surgery is currently the most effective way to lose weight and has the highest rates of weight maintenance in the long term. The Swedish Obese Subjects study was an early reporter of bariatric surgery leading to sustainable weight loss and decreased overall mortality when compared with lifestyle intervention alone. Results of the study were published in The New England Journal of Medicine in 2007.
The Roux-en-Y gastric bypass (RYGB) is considered the gold standard for weight-loss surgeries, but, unfortunately, it is not without the possibility of weight regain. In a recent prospective, long-term study of patients who had undergone RYGB, 93 percent of patients maintained at least a 10 percent weight loss from base line, 70 percent maintained at least a 20 percent weight loss and only 40 percent maintained at least a 30 percent weight loss after 12 years.
Meera Shah, M.B., Ch.B., with Endocrinology, Diabetes, Metabolism, and Nutrition at Mayo Clinic in Rochester, Minnesota, notes, "Patients who regain weight after bariatric surgery feel that they have failed their last option, leading to a great deal of frustration, anger and even depression. As we learn more about weight regain after bariatric surgery, we are finding that this is not the case — there are a number of reversible causes of weight regain in this population. Options such as behavior intervention, medications approved for weight loss and endoscopic interventions serve to counter some of the factors that have resulted in weight regain."
Behavioral intervention
Karen Grothe, Ph.D., L.P., with Psychiatry and Psychology at Mayo Clinic in Rochester, Minnesota, explains, "Behavioral intervention for weight regain after bariatric surgery is based on the large nonsurgical lifestyle intervention literature. Emerging studies focus specifically on intervention for patients experiencing post-surgical regain, addressing psychological and behavioral factors that can contribute to such regain.
"In the multisite Longitudinal Assessment of Bariatric Surgery 2 (LABS-2) study, participants who continued graze eating, who ate beyond feeling full, and who did not engage in self-weighing before or after surgery lost significantly less weight at three years post-surgery compared with participants who made those healthy behavior changes (24.6 percent vs. 38.8 percent weight loss). Lack of physical activity, uncontrolled psychological disorders and life stressors have also been suggested as factors related to regain. Behavioral drift — the slow movement away from a behavior or skill — is common for any skill that receives less attention over time, such as speaking a second language or playing a sport. It is also common among patients experiencing post-surgical weight regain.
"Studies have examined the application of traditional behavioral weight management programs for patients with weight regain after bariatric surgery to programs specifically tailored to the post-bariatric surgery population. Many patients struggling with regain are lost to follow-up; therefore, a foundational component to such specialized programs should be an open, nonjudgmental approach that begins with the acknowledgement that weight regain can occur. From that starting point, it can be helpful to offer behavioral intervention specific to this subgroup, such as the Back on Track group program we developed from a research study examining behavior therapy to stop regain.
"Back on Track is a 12-week program offered throughout the year for any patient experiencing clinically significant weight regain (10 percent or more of weight lost). It includes curricula on nonjudgmental reflection on factors that played a role in regain, reducing behavioral drift, education about emerging weight-loss medications or post-surgical endoscopic procedures, emotion regulation strategies, and self-monitoring techniques. Others are also examining the inclusion of acceptance-based strategies and different modes of intervention delivery, such as online and by phone, in hopes of augmenting outcomes and reaching more patients."
Medications
Dr. Mundi reflects, "After removal of sibutramine from the market, the lipase inhibitor orlistat was the only FDA-approved weight-loss medication available for long-term use. However, since 2012, there have been four other medications approved for the primary indication of weight loss: lorcaserin hydrochloride, phentermine-topiramate, bupropion hydrochloride-naltrexone hydrochloride, and liraglutide. These medications are centrally acting appetite suppressants with the exception of liraglutide, which also has peripheral actions in the gastrointestinal tract and inhibits gastric emptying. In the nonbariatric surgery population, when compared with placebo and in conjunction with a comprehensive lifestyle modification program, these medications provide modest additional total body weight loss (in the 4-10 percent range)."
Dr. Shah continues, "Although large randomized prospective trials are lacking, many smaller short-term trials and retrospective analyses are revealing good efficacy with the use of medications for weight regain after surgery. When choosing among these appetite suppressants in the appropriate patient, care should be given to medication interaction as well as the side effect profile of the medication. These medications have all been approved for chronic use, although given the relatively short time they have been on the market, there is limited clinical experience with efficacy and safety in the long term."
Endoscopic approach
Barham K. Abu Dayyeh, M.D., M.P.H., a gastroenterologist who specializes in bariatric and metabolic endoscopy at Mayo Clinic in Rochester, Minnesota, says, "One of the most common anatomical changes over time is the enlargement of gastrojejunal stoma size, contributing to weight regain by a reduction in satiety and allowing the patient to increase volume of food consumed in one meal. Dilated gastrojejunal stoma can be treated surgically; however, this revision requires a technically difficult dissection and has a significant risk of morbidity and complications.
Transoral outlet reduction procedure
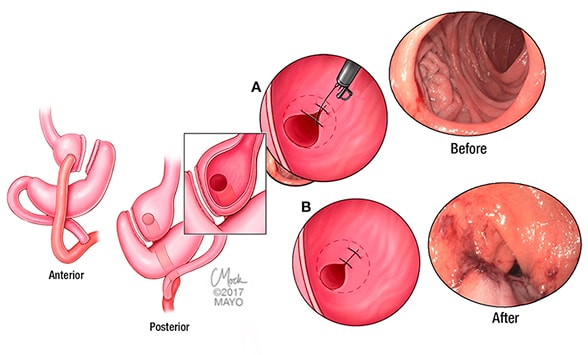
Transoral outlet reduction procedure
Anatomic relationships of Roux-en-Y gastric bypass is shown on the left. A and B. The transoral outlet reduction (TORe) endoscopy procedure. An endoscopic suturing system is used to plicate the gastrojejunal anastomosis (Before) and reduce its size to 1 cm (After), thus restoring the restrictive component of the gastric bypass. Image reprinted with permission from Endocrinology Update. Mayo Clinic. 2018;13(2):2.
"Recently, with advancements in endoscopic suturing devices, a novel approach to reduction of the stoma diameter has emerged: transoral outlet reduction (TORe) endoscopy. This procedure can be performed on an outpatient basis with a favorable risk profile compared with revisional bariatric surgery. An endoscopic suturing system is used to plicate the gastrojejunal anastomosis and reduce its size to 1 cm, thus restoring the restrictive component of the gastric bypass.
"A number of studies have shown efficacy in patients who are regaining weight. In a study published in Surgical Endoscopy in 2018, in 130 consecutive patients across three centers undergoing TORe with an endolumenal suturing device, the average weight lost at six, 12 and 18 months after TORe was 9.31 ± 6.7 kg (n = 84), 7.75 ± 8.4 kg (n = 70) and 8 ± 8.8 kg (n = 46), respectively."
Weight regain after bariatric surgery can be devastating to patients, as they often feel like failures and are at a loss for where to go next. There are now a number of options available to them, including cognitive behavioral therapy programs tailored to their needs, weight-loss medications, and endoscopic approaches such as TORe.
For more information
Sjöström L, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. The New England Journal of Medicine. 2007;357:741.
Vargas EJ, et al. Transoral outlet reduction with full thickness endoscopic suturing for weight regain after gastric bypass: A large multicenter international experience and meta-analysis. Surgical Endoscopy. 2018;32:252.