Overview
Possible signs of pink eye (conjunctivitis)
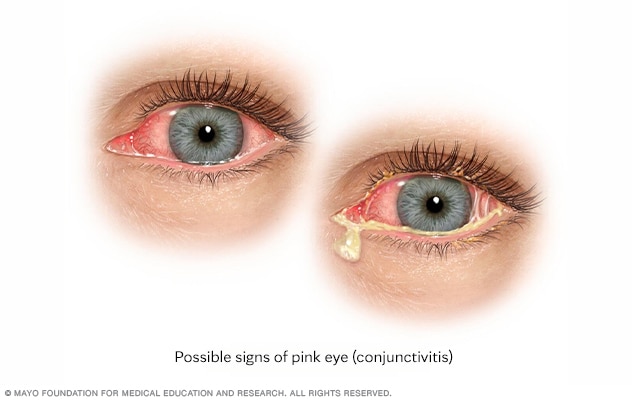
Possible signs of pink eye (conjunctivitis)
Pink eye is the inflammation or infection of the transparent membrane that lines your eyelid and eyeball. Typical symptoms include redness and a gritty sensation in your eye, along with itching. Often a discharge forms a crust on your eyelashes during the night.
Pink eye is an inflammation of the transparent membrane that lines the eyelid and eyeball. This membrane is called the conjunctiva. When small blood vessels in the conjunctiva become swollen and irritated, they're more visible. This is what causes the whites of the eyes to appear reddish or pink. Pink eye also is called conjunctivitis.
Pink eye is most often caused by a viral infection. It also can be caused by a bacterial infection, an allergic reaction or — in babies — an incompletely opened tear duct.
Though pink eye can be irritating, it rarely affects your vision. Treatments can help ease the discomfort of pink eye. Because pink eye can be contagious, getting an early diagnosis and taking certain precautions can help limit its spread.
Symptoms
The most common pink eye symptoms include:
- Redness in one or both eyes.
- Itchiness in one or both eyes.
- A gritty feeling in one or both eyes.
- A discharge in one or both eyes that forms a crust during the night that may prevent your eye or eyes from opening in the morning.
- Tearing.
- Sensitivity to light, called photophobia.
When to see a doctor
There are serious eye conditions that can cause eye redness. These conditions may cause eye pain, a feeling that something is stuck in your eye, blurred vision and light sensitivity. If you experience these symptoms, seek urgent care.
People who wear contact lenses need to stop wearing their contacts as soon as pink eye symptoms begin. If your symptoms don't start to get better within 12 to 24 hours, make an appointment with your eye healthcare professional to make sure you don't have a more serious eye infection related to contact lens use.
Causes
Causes of pink eye include:
- Viruses.
- Bacteria.
- Allergies.
- A chemical splash in the eye.
- A foreign object in the eye.
- In newborns, a blocked tear duct.
Viral and bacterial conjunctivitis
Most cases of pink eye are caused by adenovirus. It also can be caused by other viruses, including herpes simplex virus and varicella-zoster virus.
Both viral and bacterial conjunctivitis can occur along with colds or symptoms of a respiratory infection, such as a sore throat. Wearing contact lenses that aren't cleaned properly or aren't your own can cause bacterial conjunctivitis.
Both types are very contagious. They are spread through direct or indirect contact with the liquid that drains from the eye of someone who's infected. One or both eyes may be affected.
Allergic conjunctivitis
Allergic conjunctivitis affects both eyes. It is a response to an allergy-causing substance such as pollen. In response to allergens, your body produces an antibody called immunoglobulin E (IgE). IgE triggers special cells in the mucous lining of your eyes and airways to release inflammatory substances, including histamines. Your body's release of histamine can produce a number of allergy symptoms, including red or pink eyes.
If you have allergic conjunctivitis, you may experience intense itching, tearing and inflammation of the eyes. You also could have sneezing and watery nasal discharge. Most allergic conjunctivitis can be controlled with allergy eye drops. Allergic conjunctivitis is not contagious.
Conjunctivitis resulting from irritation
Irritation from a chemical splash or foreign object in the eye also is associated with conjunctivitis. Sometimes flushing and cleaning the eye to wash out the chemical or object causes redness and irritation. Symptoms, which may include watery eyes and a mucous discharge, usually clear up on their own within about a day.
If flushing doesn't resolve the symptoms, or if the chemical is a caustic one such as lye, see your healthcare professional or eye specialist as soon as possible. A chemical splash into the eye can cause permanent eye damage. Ongoing symptoms could indicate that you still have the foreign body in your eye. Or you also could have a scratch on the cornea or the membrane covering the eyeball, called the conjunctiva.
Risk factors
Risk factors for pink eye include:
- Exposure to someone infected with the viral or bacterial form of conjunctivitis.
- Exposure to something you're allergic to, for allergic conjunctivitis.
- Using contact lenses, especially extended-wear lenses.
Complications
In both children and adults, pink eye can cause inflammation in the cornea that can affect vision. Prompt evaluation and treatment by your healthcare professional can reduce the risk of complications. See your professional if you have:
- Eye pain.
- A feeling that something is stuck in the eye.
- Blurred vision.
- Light sensitivity.
Prevention
Preventing the spread of pink eye
Practice good hygiene to control the spread of pink eye. For instance:
- Don't touch your eyes with your hands.
- Wash your hands often.
- Use a clean towel and washcloth daily.
- Don't share towels or washcloths.
- Change your pillowcases often.
- Throw away old eye cosmetics, such as mascara.
- Don't share eye cosmetics or personal eye care items.
Keep in mind that pink eye is no more contagious than the common cold. It's okay to return to work, school or child care if you're able to practice good hygiene and avoid close contact. However, if work, school or child care involves close contact with others, it may be best to stay home until your or your child's symptoms clear up.
Preventing pink eye in newborns
Newborns' eyes are susceptible to bacteria present in the mother's birth canal. These bacteria often cause no symptoms in the mother. In some cases, these bacteria can cause infants to develop a serious form of conjunctivitis known as ophthalmia neonatorum. This condition needs immediate treatment to keep the baby's sight. That's why shortly after birth, an antibiotic ointment is applied to every newborn's eyes. The ointment helps prevent eye infection.
Jan. 10, 2025