Overview
Pericarditis
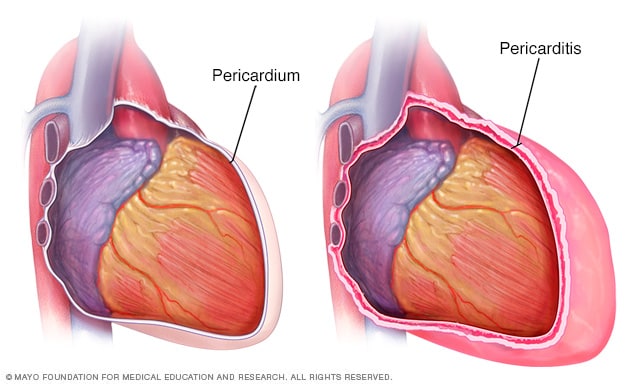
Pericarditis
The heart on the left shows the typical outer lining of the heart (pericardium). The heart on the right shows a swollen and infected lining (pericarditis).
Pericarditis is swelling and irritation of the thin, saclike tissue surrounding the heart. This tissue is called the pericardium. Pericarditis often causes sharp chest pain. The chest pain occurs when the irritated layers of the pericardium rub against each other.
Pericarditis often is mild. It may go away without treatment. Treatment for more-serious symptoms can include medicines and, very rarely, surgery. When healthcare professionals find and treat pericarditis early, that may help lower the risk of long-term complications from pericarditis.
Symptoms
Chest pain is the most common symptom of pericarditis. It usually feels sharp or stabbing. But some people have dull, achy or pressure-like chest pain.
Most often, pericarditis pain is felt behind the breastbone or on the left side of the chest. The pain may:
- Spread to the left shoulder and neck, or to both shoulders.
- Get worse when coughing, lying down or taking a deep breath.
- Get better when sitting up or leaning forward.
Other symptoms of pericarditis can include:
- Cough.
- Fatigue or general feeling of weakness or being sick.
- Swelling of the legs or feet.
- Low-grade fever.
- Pounding or racing heartbeat, also called heart palpitations.
- Shortness of breath when lying down.
- Swelling of the belly, also called the abdomen.
The specific symptoms depend on the type of pericarditis. Pericarditis is grouped into different categories, according to the pattern of symptoms and how long symptoms last.
- Acute pericarditis begins suddenly but doesn't last longer than four weeks. Future episodes can occur. It may be hard to tell the difference between acute pericarditis and pain due to a heart attack.
- Recurrent pericarditis occurs about 4 to 6 weeks after a bout of acute pericarditis. No symptoms happen in between.
- Incessant pericarditis lasts about 4 to 6 weeks but less than three months. The symptoms continue over this whole time.
- Chronic constrictive pericarditis usually develops slowly and lasts longer than three months.
When to see a doctor
Get medical care right away if you have new symptoms of chest pain.
Many of the symptoms of pericarditis are like those of other heart and lung conditions. It's important to be thoroughly checked by a healthcare professional if you have any type of chest pain.
Causes
The cause of pericarditis is often hard to determine. A cause may not be found. When this happens, it's called idiopathic pericarditis.
Pericarditis causes can include:
- Immune system response after heart damage due to a heart attack or heart surgery. Other names for this include Dressler syndrome, post-myocardial infarction syndrome and post-cardiac injury syndrome.
- Infections, such as those caused by viruses.
- Injury to the heart or chest.
- Lupus.
- Rheumatoid arthritis.
- Other long-term health conditions, including kidney failure and cancer.
- Some medicines, such as the seizure treatment phenytoin (Dilantin) and medicine called procainamide to treat an irregular heartbeat.
Complications
When pericarditis is found and treated early, the risk of complications usually becomes lower. Complications of pericarditis can include:
- Fluid buildup around the heart, also called pericardial effusion. The fluid buildup can lead to further heart complications.
- Thickening and scarring of the heart lining, also called constrictive pericarditis. Some people with long-term pericarditis develop permanent thickening and scarring of the pericardium. The changes prevent the heart from filling and emptying properly. This complication often leads to severe swelling of the legs and abdomen, and shortness of breath.
- Pressure on the heart due to fluid buildup, also called cardiac tamponade. This life-threatening condition prevents the heart from filling properly. Less blood leaves the heart, causing a large drop in blood pressure. Cardiac tamponade requires emergency treatment.
Prevention
There's no specific way to prevent pericarditis. But you can take these steps to prevent infections, which might help lower the risk of heart inflammation:
- Stay away from people who have a viral or flu-like illness until they've recovered. If you're sick with symptoms of a viral infection, try not to expose others. For instance, cover your mouth when you sneeze or cough.
- Follow good hygiene. Regular hand-washing can help prevent spreading illness. Scrub your hands with soap and water for at least 20 seconds.
- Get recommended vaccines. Stay up to date on the recommended vaccines, including those that protect against COVID-19, rubella and influenza. These are examples of viral diseases that can cause inflammation of the heart muscle, called myocarditis. Myocarditis and pericarditis can happen together due to a viral infection. Rarely, the COVID-19 vaccine can cause pericarditis and myocarditis, especially in males ages 12 through 17. Talk to your healthcare professional about the benefits and risks of vaccines.
History of infectious disease outbreaks and vaccines timeline.
Learn about the history of major disease outbreaks, epidemics and pandemics, as well as the impact vaccines and research had on many infectious diseases.
Find out more at History of infectious disease outbreaks and vaccines timeline.