Overview
Orchitis (or-KIE-tis) refers to infection or swelling and irritation, called inflammation, of one or both testicles. Infections are common causes of orchitis. These include sexually transmitted infections (STIs) and infection with the mumps virus.
Orchitis often is linked with an infection of the epididymis, which is the coiled tube at the back of the testicle that stores and carries sperm. The infection of the epididymis is called epididymitis. With orchitis, the condition is called epididymo-orchitis.
Orchitis may cause pain and swelling. It is typically treated with supportive underwear, cold packs, medicines called anti-inflammatories and, in some instances, medicines called antibiotics. But it can take several weeks or even months for tenderness in the scrotum to go away.
Rarely, severe orchitis can affect being able to have children, called fertility. This most often happens in people who get the infection during childhood or the teen years.
Products & Services
Symptoms
Orchitis symptoms most often come on quickly. They can include:
- Swelling in one or both testicles.
- Pain ranging from mild to very bad.
- Fever.
- Nausea and vomiting.
- Feeling ill, called malaise.
When to see a doctor
For pain or swelling in your scrotum that comes on quickly, see your healthcare professional right away.
A number of conditions can cause testicle pain. Many go away on their own. But some need treatment right away.
One such condition involves twisting of the spermatic cord, called testicular torsion. The pain of this might feel like the pain of orchitis. Your healthcare professional can do tests to find out which condition is causing your pain.
Causes
Male reproductive system
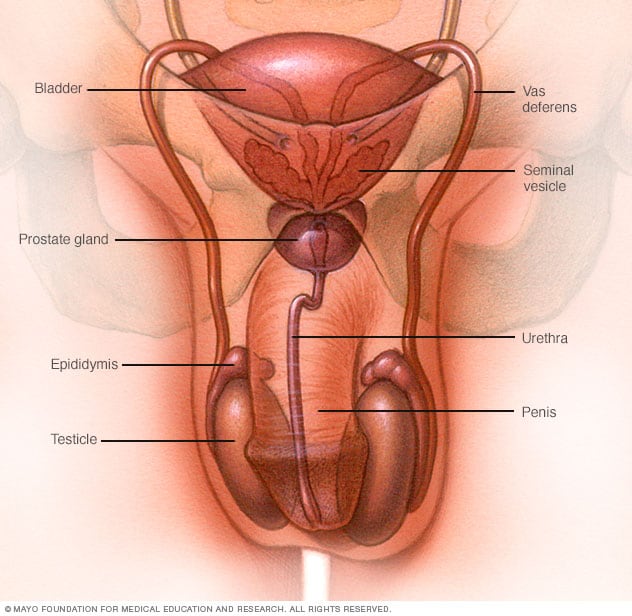
Male reproductive system
The male reproductive system makes, stores and moves sperm. Testicles produce sperm. Fluid from the seminal vesicles and prostate gland mixes with sperm to make semen. The penis ejaculates semen during sexual activity.
Infection with a virus or bacteria can cause orchitis. Sometimes a cause can't be found.
Bacterial orchitis
Most often, bacterial orchitis is linked with or is the result of epididymitis. An infection of the urethra or bladder that spreads to the epididymis most often causes epididymitis. Sometimes, an STI is the cause. But this is a less common cause of orchitis in adults.
Viral orchitis
The mumps virus most often causes viral orchitis. Nearly one-third of people assigned male at birth who get the mumps after puberty get orchitis. This most often happens 4 to 7 days after the mumps start. Thanks to routine childhood vaccinations for the mumps, mumps orchitis happens less often than it used to.
Risk factors
Factors that raise the risk of orchitis include untreated conditions that block the urinary tract. These include prostate enlargement or scar tissue in the urethra, called urethral stricture.
Procedures done through the urethra also raise the risk of orchitis. These include having a tube, called a catheter, or a scope in the bladder.
The main risk factor for mumps orchitis is not getting the mumps vaccine.
Sexual behaviors that can lead to STIs put you at risk of sexually transmitted orchitis. Those behaviors include having:
- More than one sexual partner.
- Sex with a partner who has an STI.
- Sex without a condom.
- A personal history of an STI.
Complications
Most often, orchitis gets better with supportive care. It can take several weeks or months before the pain and swelling go away. Rarely, complications of orchitis may include:
- Testicular atrophy. Over time, orchitis can cause the affected testicle to shrink.
- Scrotal abscess. The infected tissue fills with pus.
- Infertility. Sometimes, orchitis can cause you to not be able to have a child, called infertility. Or it can cause the body to make too little testosterone, a condition called hypogonadism. But these are less likely to happen if orchitis affects only one testicle.
Prevention
To help prevent orchitis:
- Get the vaccine against mumps, the most common cause of viral orchitis.
- Practice safe sex to help protect against STIs that can cause bacterial orchitis.
- Talk with your healthcare professional if you have trouble with urination. That may mean you have a blockage or other condition that can lead to orchitis.
Nov. 08, 2024