Overview
Medulloblastoma (muh-dul-o-blas-TOE-muh) is a cancerous, also called malignant, brain tumor that starts in the back and lower part of the brain.
This part of the brain is called the cerebellum. The cerebellum helps control balance, movement and coordination.
Medulloblastoma is the most common cancerous brain tumor in children, though it also can happen in adults.
Medulloblastoma forms when cells in the cerebellum develop changes in their DNA. These changes cause the cells to grow and multiply quickly. The tumor can press on nearby parts of the brain and may block the flow of cerebrospinal fluid. This can cause pressure to build up in the brain.
Medulloblastoma can spread, also known as metastasize, to other parts of the brain and spinal cord through cerebrospinal fluid. It rarely spreads outside the central nervous system.
There are four main types, also called molecular groups, of medulloblastoma. These groups are defined by the tumor’s genetic features. The four groups are WNT-activated, SHH-activated (including TP53-mutant and TP53-wildtype), group 3 and group 4.
Group 3 and group 4 tumors are sometimes described together as non-WNT and non-SHH tumors, although they are separate groups. Knowing the tumor type helps guide treatment.
Hearing this diagnosis can feel overwhelming. It may help to know that, with treatment, many children with medulloblastoma live well beyond five years after diagnosis.
Every child's situation is different. The outlook depends on several factors, including age, tumor type, whether the cancer has spread and how much of the tumor can be safely removed.
Products & Services
Types
The type of medulloblastoma is based on how the tumor cells look under a microscope and on lab tests that look at changes in the tumor's genes. The type of medulloblastoma helps guide treatment and can affect survival.
All medulloblastomas are considered grade 4 tumors. The subtypes below describe the tumor's molecular features, not its grade.
Molecular types
Most medulloblastomas can be grouped into four main types based on changes in their genes. These tumor types include:
- WNT-activated (wingless/integrated). WNT is the name of a cell signaling pathway involved in brain development. WNT-activated tumors are one of the less common medulloblastoma types. They often respond very well to treatment and are linked to the best survival rates. They are most often seen in older children and teens.
- SHH-activated (sonic hedgehog). Sonic hedgehog is the name of a cell growth signaling pathway involved in brain development. SHH medulloblastoma can occur in infants, children and adults. Survival varies depending on other tumor features and gene changes. Some SHH tumors, known as SHH-activated TP53-wildtype, behave less aggressively. Other SHH tumors, called SHH-activated TP53-mutant, may be harder to treat.
- Group 3. Group 3 medulloblastoma is more common in young children. These tumors are non-SHH and non-WNT molecular types. It tends to grow and spread more quickly than other types. It may be harder to treat and is often linked to lower survival rates compared with WNT tumors.
- Group 4. Group 4 medulloblastoma is the most common type. These tumors are non-SHH and non-WNT molecular types. It can occur in children and adults. Its behavior varies. Some tumors respond well to treatment, while others may spread at diagnosis.
The numbering starts at 3 and 4 because the first two groups were named WNT-activated and SHH-activated based on specific gene patterns.
Cell appearance types
Medulloblastoma also can be described based on how the cells look under a microscope although genetic and molecular features are increasingly used for diagnosis and understanding outcomes. These include:
- Classic.
- Desmoplastic or nodular.
- Large cell or anaplastic.
These features also help healthcare professionals understand how the tumor may behave.
How is medulloblastoma different from other brain tumors?
Medulloblastoma is different from many other types of brain tumors. These tumors differ in where they start, who they affect and how they are treated.
Here's how they compare:
- Medulloblastoma versus glioma. Medulloblastoma is not a glioma. Gliomas form from support cells in the brain called glial cells. Medulloblastoma forms from developing nerve cells in the cerebellum.
- Medulloblastoma versus glioblastoma. Glioblastoma is an aggressive brain tumor that usually affects adults and starts in the upper parts of the brain. Medulloblastoma is more common in children and often responds better to treatment.
- Medulloblastoma versus ependymoma. Ependymomas begin in cells that line the fluid-filled spaces of the brain and spinal cord. Medulloblastoma tends to grow in the cerebellum and is more likely to spread through cerebrospinal fluid.
Symptoms
Medulloblastoma
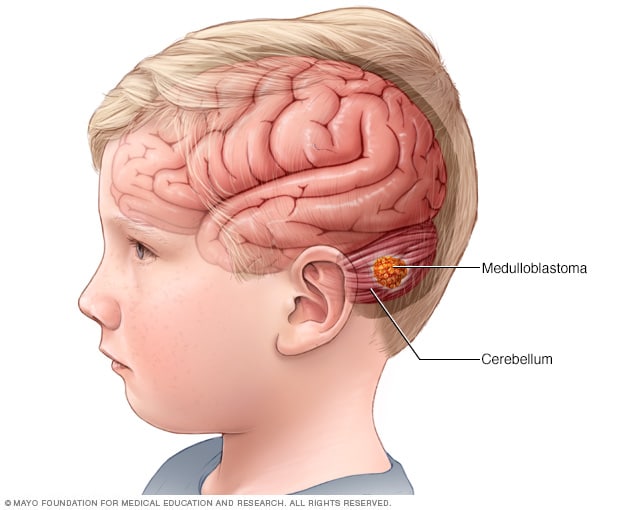
Medulloblastoma
Medulloblastoma is a type of brain cancer that starts in the part of the brain called the cerebellum. Medulloblastoma is the most common type of cancerous brain tumor in children.
Symptoms of medulloblastoma happen when the tumor grows and presses on parts of the brain. The tumor also can block the usual flow of cerebrospinal fluid. This can cause pressure to build inside the head.
Common signs and symptoms of medulloblastoma may include:
- Dizziness.
- Double vision or other vision changes.
- Headaches, which are often worse in the morning.
- Nausea or vomiting.
- Poor coordination.
- Tiredness.
- Difficulty with balance or an unsteady walk.
Headaches and vomiting often happen because of the buildup of pressure inside the skull.
Symptoms in young children and infants
In young children, symptoms may develop over several weeks. Children may have trouble walking, seem clumsy or lose balance. Infants may have an increase in head size, unusual sleepiness or feeding difficulties.
Symptoms in children and adults
Symptoms of medulloblastoma are generally similar in adults and children because the tumor usually starts in the same part of the brain. Both may have headaches, balance difficulties and nausea.
Can you feel a medulloblastoma tumor?
Medulloblastoma grows deep inside the brain. It does not usually cause a lump or bump that you can feel on the outside of the head.
When to see a doctor
Make an appointment with your healthcare professional if you or your child has symptoms that worry you, especially ongoing headaches, repeated vomiting, or new issues with balance or vision.
Causes
It's not clear what causes medulloblastoma. This cancer starts as a growth of cells in the lower back part of the brain, called the cerebellum.
DNA contains instructions that tell cells how to grow and function. In healthy cells, DNA controls how fast cells grow and when they die. In cancer cells, DNA changes give different instructions. These changes tell cancer cells to grow and multiply quickly. Cancer cells can keep living when healthy cells would die. This leads to too many cells that form a tumor.
The tumor can grow and press on nearby brain structures. Medulloblastoma cells also can metastasize to other parts of the brain and spinal cord through cerebrospinal fluid.
Risk factors
Risk factors are things that may increase the chance of developing medulloblastoma. Most people with medulloblastoma do not have a known risk factor.
- Young age. These tumors can happen at any age, but they happen most often in children.
- Inherited syndromes. Most cases of medulloblastoma are not inherited. However, the tumor happens more often in people with certain rare genetic conditions that increase cancer risk. These include Fanconi anemia, Gorlin syndrome, Li-Fraumeni syndrome, Rubinstein-Taybi syndrome and Turcot syndrome.
There are no known lifestyle or environmental risk factors for medulloblastoma.