Overview
Hydronephrosis
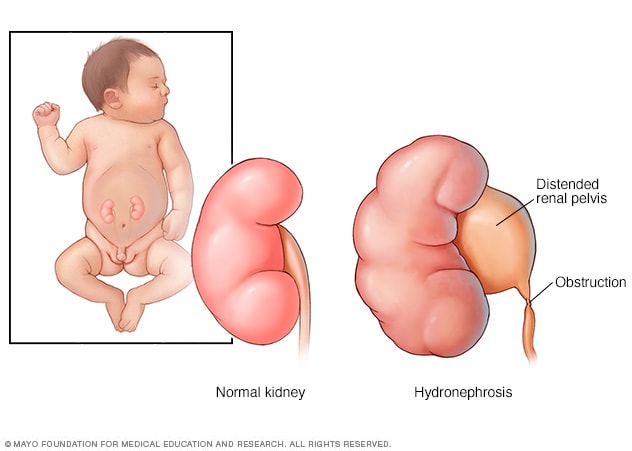
Hydronephrosis
Hydronephrosis happens when urine builds up in a kidney. Often, a blockage called an obstruction in the upper part of the urinary tract causes the buildup. Kidney swelling can result. This causes the part of the kidney called the renal pelvis to bulge, or become distended. It could lead to kidney scarring, and the kidney may not work as well as it should.
Hydronephrosis is swelling of one or both kidneys. It happens when urine can't drain from a kidney and builds up in the kidney as a result. The condition can be due to a blockage in the tubes that drain urine from the kidneys. It also can happen due to a difference present at birth that prevents urine from draining properly. In some people, hydronephrosis causes kidney damage over time.
Hydronephrosis can happen at any age. The condition often causes no symptoms. People who get symptoms may have side and back pain, painful urination, vomiting and fever. Healthcare professionals have various ways to spot hydronephrosis. Tests to find the condition can be done during infancy or sometimes before a baby is born.
Treatment for hydronephrosis depends on the condition's cause. Some people need medicine or surgery to feel better and prevent kidney damage. Mild hydronephrosis sometimes goes away on its own over time.
Symptoms
Hydronephrosis often causes no symptoms. But when symptoms happen, they can include:
- Pain in the side and back that may travel to the lower stomach area or groin.
- Pain with urination, or feeling a need to urinate that is urgent or happens often.
- Upset stomach and vomiting.
- Fever.
- Failure to thrive in infants.
- Weight loss or loss of appetite.
- Blood in urine.
When to see a doctor
Call your healthcare professional if you have any symptoms of hydronephrosis. Babies with the condition often don't have symptoms. But get your baby a healthcare checkup right away for symptoms such as high fever.
Causes
Female urinary system
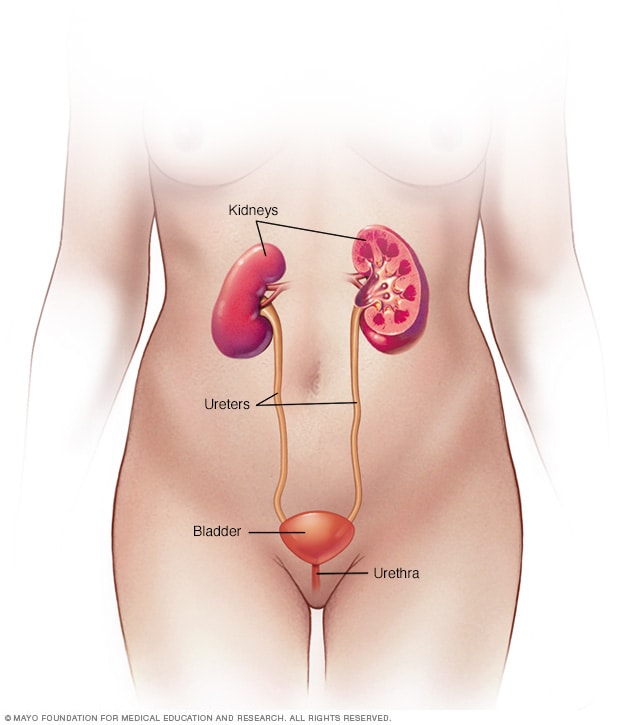
Female urinary system
Your urinary system includes the kidneys, ureters, bladder and urethra. The urinary system removes waste from the body through urine. The kidneys are located toward the back of the upper abdomen. They filter waste and fluid from the blood and produce urine. Urine moves from the kidneys through narrow tubes to the bladder. These tubes are called the ureters. The bladder stores urine until it's time to urinate. Urine leaves the body through another small tube called the urethra.
Male urinary system
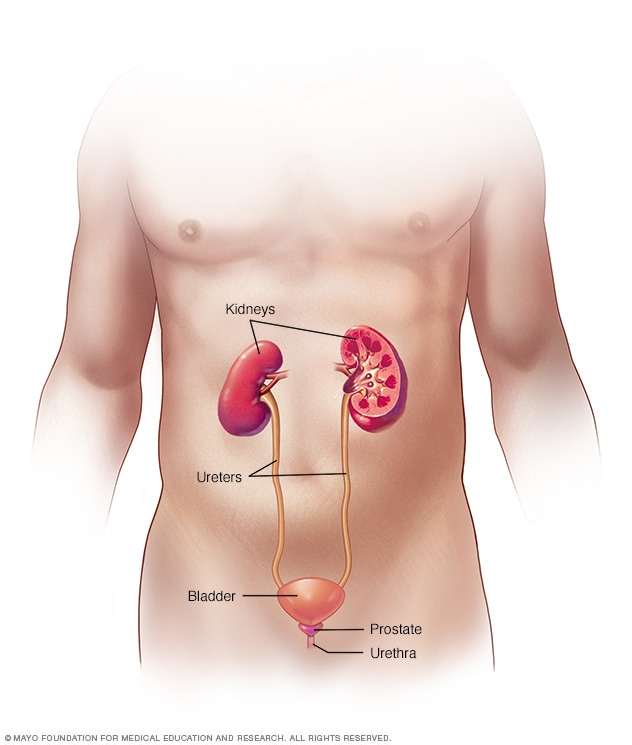
Male urinary system
Your urinary system includes the kidneys, ureters, bladder and urethra. The urinary system removes waste from the body through urine. The kidneys are located toward the back of the upper abdomen. They filter waste and fluid from the blood and produce urine. Urine moves from the kidneys through narrow tubes to the bladder. These tubes are called the ureters. The bladder stores urine until it's time to urinate. Urine leaves the body through another small tube called the urethra.
Causes of hydronephrosis include a blockage or other health issue that affects the urinary tract. The urinary tract includes the kidneys and the bladder. Urine flows from the kidneys to the bladder through tubes called ureters. Urine leaves the bladder and the body through another tube called the urethra.
A partly or fully blocked urinary tract can keep urine from leaving the kidneys and cause swelling. Other issues that disrupt the urinary tract can cause urine to flow backward through the ureters from the bladder up into the kidneys. When urine flows the wrong way, the condition is called vesicoureteral reflux.
Causes of hydronephrosis include the following:
Conditions present at birth. Some babies are born with a partial kidney blockage called a ureteropelvic junction obstruction. Most often, the blockage forms where a kidney attaches to one of the tubes that carry urine to the bladder. These tubes are called the ureters.
Other babies are born with a ureter that isn't typical in structure. Urine flows backward through the ureter from the bladder up into the kidney as a result. When backward urine flow happens, it's known as vesicoureteral reflux.
- Kidney stones. These are hard buildups of minerals and salts that form inside the kidneys.
- Enlarged prostate. A very enlarged prostate can cause the bladder to have trouble emptying urine. Urine may back up into the kidneys as a result.
- Injured or narrowed ureter. Pelvic surgery done with cuts through the stomach area could injure a ureter by accident. A ureter could become narrowed for reasons such as scarring after surgery or having radiation therapy for prostate cancer.
- Urinary tract infection. This type of infection can inflame any part of the urinary tract, including the kidneys.
- Pregnancy. Swelling of the kidneys' urine drainage system is common during pregnancy. Often, hydronephrosis in pregnant people doesn't cause symptoms and goes away after giving birth.
- Cancer. With some types of cancer, a tumor can cause a urinary tract blockage. These include cancers of the bladder, cervix, colon and prostate.
Risk factors
Hydronephrosis risk factors among adults ages 20 to 60 include being born female. The higher risk could be due to certain conditions that affect the uterus, such as pregnancy. It also could be due to conditions that affect the ovaries, such as cysts, buildups of pus and cancer. Risk factors for people older than age 60 include having an enlarged prostate or a urinary tract blockage from cancer.
Complications
Hydronephrosis can lead to other health conditions called complications. Without treatment, some people who have severe hydronephrosis develop lasting kidney damage. Rarely, the condition can cause an affected kidney to lose its ability to filter blood, also called kidney failure.
Nov. 06, 2024