Jan. 18, 2019
Understanding and treating all aspects of patellofemoral instability are key to preventing recurrence of instability and pain. "Patellofemoral instability is a multifactorial problem. Thorough diagnosis allows us to address all the anatomic issues and achieve an instability rate of less than 20 percent," says Todd A. Milbrandt, M.D., a pediatric orthopedic surgeon at Mayo Clinic in Rochester, Minnesota.
Early intervention is important for optimal outcomes. "Patellofemoral instability can occur even in young kids, and we don't want to wait until they're skeletally mature to treat it," Dr. Milbrandt says. "We have techniques to modify children's growth. For severe knock-knee, we can straighten the leg with a small plate and then do the patella reconstruction. If we wait until the child finishes growing, the patella and the trochlea deform and the reconstruction is much harder."
A quiver of treatment options
Most of the children seen at Mayo Clinic Children's Center for patellofemoral instability have sports-related injuries. Dr. Milbrandt cites one patient who was unable to climb stairs without dislocating her kneecap.
"We go from that extreme to kids who tend to dislocate when they play a certain sport. Those kids could potentially just change sports — from playing soccer to swimming, for example — but they don't want to do that," Dr. Milbrandt says. "For a lot of young people, their sport is their peer group and their definition of themselves."
To define all the components of an individual's patellofemoral instability, a child undergoes:
- A thorough physical evaluation, including rotation of the tibia and femur
- X-rays from the ankle to the hip, to evaluate standing alignment and knee position
- CT scans or MRI to determine where the patellar tendon attaches to the tibia and to establish the tibial tuberosity-trochlear groove distance
Dr. Milbrandt notes that Mayo Clinic Children's Center performs these tests, so testing before referral isn't necessary.
A surgical plan is then developed. "We have a quiver of treatment options, all the way from minor tightening to very complicated osteotomies around the tibia and fibula," Dr. Milbrandt says.
MRI of a 16-year-old boy with patellofemoral instability
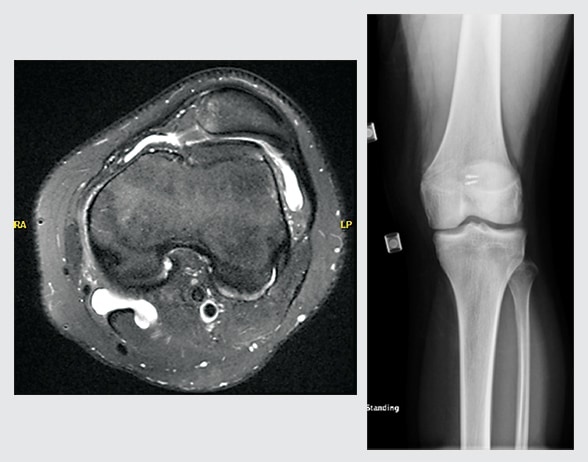
MRI of a 16-year-old boy with patellofemoral instability
On the left, MRI of a 16-year-old boy with patellofemoral instability shows lateral displacement of the patella. On the right, a postoperative image shows the patellar suture anchors and femoral fixation.
To reduce the risk of patella breakage, surgeons avoid drilling holes in the kneecap for ligament fixation. "We use metal suture anchors or screws in the kneecap, and we tension that on the femoral side. We tie the ligaments there so that they stay in place," Dr. Milbrandt says.
A complete physical therapy protocol is provided after surgery. "Once strength in the vastus medialis oblique is apparent, we do a series of functional tests — assessing the knee's movement when the patient hops and jumps down from a block. It's important to see how that kneecap functions," Dr. Milbrandt says.
To continually improve their technique, orthopedic surgery residents study and write up every patellofemoral instability case experience. Mayo Clinic's team approach also allows pediatric orthopedic specialists to consult their colleagues in adult practice. "We discuss our difficult cases, and team up as co-surgeons when needed," Dr. Milbrandt says. "We learn from one another and from our patient database, and that's a huge advantage."