March 20, 2018
Arthroscopy, the gold standard for diagnosis of intra-articular knee pathology, is typically performed in an operating room with the patient given regional or general anesthetics. Mayo Clinic now offers in-office knee arthroscopy that uses only local anesthetics yet provides images of sufficient quality to facilitate diagnosis of complex cases.
"This is an exciting technology that gives the surgeon a highly accurate view — often superior to an MRI — and that allows patients to avoid anesthesia and walk out of the office after the procedure," says Anikar Chhabra, M.D., a consultant in Orthopedic Surgery at Mayo Clinic in Phoenix, Arizona. "In our experience, this can be a safe and cost-effective adjunct to traditional methods to aid the physician to get an accurate diagnosis."
In-office arthroscopy shows a normal lateral compartment
In-office arthroscopy shows a normal lateral compartment
In-office arthroscopy shows a normal lateral compartment. The visualization has improved significantly with the new technology.
Small arthroscope with a 14-gauge needle
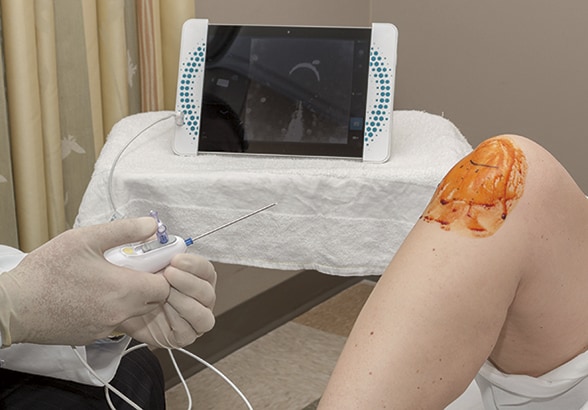
Small arthroscope with a 14-gauge needle
In-office knee arthroscopy involves a small arthroscope with a 14-gauge needle. The patient's knee has been anesthetized locally.
The new device, approved by the Food and Drug Administration, is an enhanced version of in-office arthroscopy designs dating back to the 1990s. Those designs were cumbersome, incorporating a tower, fluid irrigation systems and standard optics. The second-generation device forgoes the tower and uses a 14-gauge needle and digital optics.
"The old system just wasn't practical to use in the outpatient setting. But now the system is a small device hooked up to a tablet," Dr. Chhabra says. "The quality of the images has improved dramatically."
Indications for use
In-office arthroscopy is especially useful for patients whose MRIs are inconclusive. "That's almost always the case for a patient who has had previous meniscal and chondral knee surgery," Dr. Chhabra says. "The in-office arthroscopy is also useful for grading and judging cartilage with acute or chronic conditions, as MRIs are often inaccurate when it comes to articular cartilage of the knee."
In addition, in-office arthroscopy can be an option for people who cannot tolerate MRI due to claustrophobia or because they have pacemakers or other metal implants. Dr. Chhabra notes that, once the technique is mastered, in-office knee arthroscopy can be performed in about 15 minutes, and the images reviewed with the patient immediately afterward.
"This technology is an observational tool that can confirm diagnosis. If we know that a person has a knee problem that requires repair, we would do the arthroscopic procedure in the operating room," Dr. Chhabra says. "But in-office arthroscopy is an exciting option for people who have had an MRI that isn't conclusive."
He cites the example of a 43-year-old patient who came to Mayo Clinic with right knee pain eight years after a motor vehicle accident. She had undergone multiple MRIs and been evaluated by several other physicians at other centers. Her diagnosis was inconclusive, and her treatment relied on corticosteroid injections and anti-inflammatory medications to try to control her pain.
In-office arthroscopy of the patient's knee revealed lateral pathology including a 10-mm-by-10-mm grade IV chondral defect in the lateral femoral condyle and fraying of the anterior horn of the lateral meniscus. Further examination showed a 15-mm-by-15-mm grade IV chondral lesion of the medial condyle and grade III/IV fissuring degeneration of the lateral facet of the patella.
"It's possible that if direct visualization was used earlier, the patient might have had a wider array of cartilage treatment options available to her," Dr. Chhabra says. "With the correct diagnosis, we were able to give her appropriate nonoperative and operative options to her problem."
Mayo Clinic's campus in Arizona is participating in a multicenter clinical trial comparing the diagnostic accuracy of in-office knee arthroscopy with MRI. Dr. Chhabra has used in-office arthroscopy for about 16 months, with excellent results.
"In-office arthroscopy presents minimal risk, especially when compared with diagnostic arthroscopy in the outpatient setting," Dr. Chhabra says. "Although studies are ongoing, in-office arthroscopy appears to offer a cost-effective and safe diagnostic procedure."