Overview
A stye (sty) is a red, painful lump near the edge of your eyelid that may look like a boil or a pimple. Styes are often filled with pus. A stye usually forms on the outside of your eyelid, but sometimes it can form on the inner part of your eyelid.
In most cases, a stye will begin to disappear on its own in a couple days. In the meantime, you may be able to relieve the pain or discomfort of a stye by applying a warm washcloth to your eyelid.
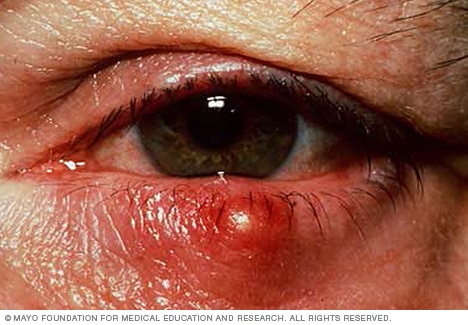
Stye
A stye is a bacterial infection involving one or more of the small glands near the base of your eyelashes. It is similar to a boil or a pimple and is often painful.
Symptoms
Signs and symptoms of a stye include:
- A red lump on your eyelid that is similar to a boil or a pimple
- Eyelid pain
- Eyelid swelling
- Tearing
Another condition that causes inflammation of the eyelid is a chalazion. A chalazion occurs when there's a blockage in one of the small oil glands near the eyelashes. Unlike a stye, a chalazion usually isn't painful and tends to be most prominent on the inner side of the eyelid. Treatment for both conditions is similar.
When to see a doctor
Most styes are harmless to your eye and won't affect your ability to see clearly. Try self-care measures first, such as applying a warm washcloth to your closed eyelid for five to 10 minutes several times a day and gently massaging the eyelid. Contact your doctor if:
- The stye doesn't start to improve after 48 hours
- Redness and swelling involves the entire eyelid or extends into your cheek or other parts of your face
From Mayo Clinic to your inbox
Causes
A stye is caused by an infection of oil glands in the eyelid. The bacterium staphylococcus is commonly responsible for most of these infections.
Risk factors
You are at increased risk of a stye if you:
- Touch your eyes with unwashed hands
- Insert your contact lenses without thoroughly disinfecting them or washing your hands first
- Leave on eye makeup overnight
- Use old or expired cosmetics
- Have blepharitis, a chronic inflammation along the edge of the eyelid
- Have rosacea, a skin condition characterized by facial redness
Prevention
To prevent eye infections:
- Wash your hands. Wash your hands with soap and warm water or use an alcohol-based hand sanitizer several times each day. Keep your hands away from your eyes.
- Take care with cosmetics. Reduce your risk of recurrent eye infections by throwing away old cosmetics. Don't share your cosmetics with others. Don't wear eye makeup overnight.
- Make sure your contact lenses are clean. If you wear contact lenses, wash your hands thoroughly before handling your contacts and follow your doctor's advice on disinfecting them.
- Apply warm compresses. If you've had a stye before, using a warm compress regularly may help prevent it from coming back.
- Manage blepharitis. If you have blepharitis, follow your doctor's instructions for caring for your eyes.
